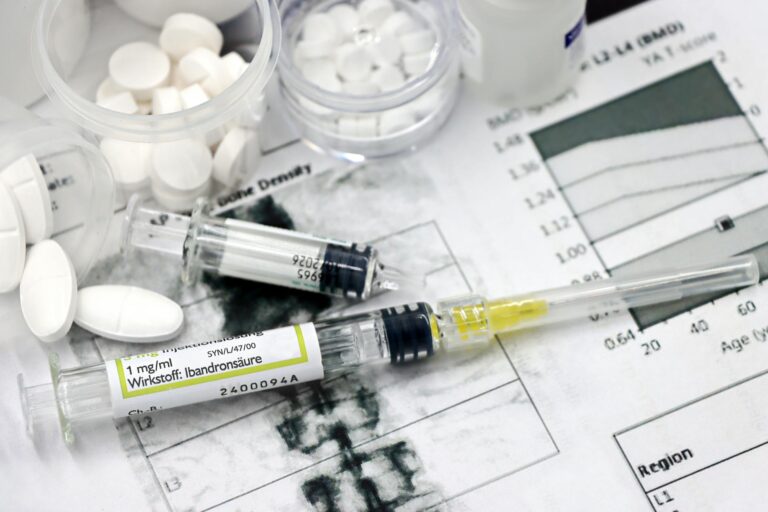
The drug generating the most excitement in heart failure treatment right now is finerenone, marketed as Kerendia, which earned FDA approval on July 14, 2025, for a patient population that has been notoriously difficult to treat. In the landmark FINEARTS-HF trial involving 6,001 patients, finerenone delivered a 16% relative risk reduction in the composite of cardiovascular death and total heart failure events compared to placebo over a median follow-up of 2.7 years. What makes this particularly remarkable is that it targets heart failure with preserved ejection fraction, a condition that for decades had cardiologists essentially shrugging their shoulders because almost nothing worked. But finerenone is not the only drug reshaping the landscape.
Aficamten, now sold as Myqorzo, received FDA approval in December 2025 for obstructive hypertrophic cardiomyopathy, and semaglutide — yes, the same compound behind the weight loss drug Wegovy — is showing striking results in heart failure patients who are also obese. For readers of this site, the connection between heart health and brain health is not abstract. Heart failure is one of the strongest risk factors for cognitive decline and dementia, and any drug that meaningfully reduces cardiovascular events has downstream implications for the brain. This article breaks down the most significant new heart failure treatments, what the clinical trials actually showed, who these drugs help (and who they may not), and what is still coming down the pipeline in 2026.
Table of Contents
- What Is the New Heart Failure Drug Outperforming Previous Treatments, and Why Does It Matter?
- How Heart Failure Drugs Affect Brain Health and Dementia Risk
- Myqorzo and the New Approach to Hypertrophic Cardiomyopathy
- Semaglutide for Heart Failure — Where Weight Loss Meets Cardiac Treatment
- Kidney Risks, Drug Interactions, and What Caregivers Need to Watch
- What Is Coming Next in the Heart Failure Pipeline
- The Bigger Picture for Heart and Brain Health
- Conclusion
- Frequently Asked Questions
What Is the New Heart Failure Drug Outperforming Previous Treatments, and Why Does It Matter?
Kerendia (finerenone) is the first and only nonsteroidal mineralocorticoid receptor antagonist approved for heart failure. That distinction matters because older MRAs like spironolactone, while effective, come with a well-known set of side effects — including hormonal disruptions that many patients find intolerable. Finerenone was designed to sidestep those problems. Its approval specifically covers adults with heart failure whose left ventricular ejection fraction is 40% or greater, a category that includes both heart failure with mildly reduced ejection fraction (HFmrEF) and heart failure with preserved ejection fraction (HFpEF). The reason this is being called a breakthrough is historical context. HFpEF accounts for roughly half of all heart failure cases, and until recently, clinicians had almost no pharmacological tools that demonstrated clear benefit in rigorous trials.
Patients were managed with diuretics and lifestyle modifications, but nothing was genuinely altering outcomes. The FINEARTS-HF trial changed that calculus. Across 6,001 randomized patients followed for a median of 2.7 years, finerenone reduced the combined endpoint of cardiovascular death and total heart failure events by 16% relative to placebo. However, finerenone is not without trade-offs. Worsening renal function was reported in 18% of patients taking the drug compared to 12% on placebo. For patients who already have compromised kidney function — which is common in older adults with heart failure — this is a serious consideration that requires close monitoring. The drug outperforms in the aggregate, but individual risk profiles still matter enormously.

How Heart Failure Drugs Affect Brain Health and Dementia Risk
The relevance of heart failure treatment to a brain health audience is not a stretch. Chronic heart failure reduces cardiac output, which means less blood flow reaches the brain over months and years. this chronic hypoperfusion has been linked in multiple studies to accelerated cognitive decline, increased white matter lesions, and higher rates of both vascular dementia and Alzheimer’s disease. Put simply, a failing heart starves the brain. Any drug that reduces heart failure hospitalizations and cardiovascular death is, by extension, potentially protective of cognitive function.
The 16% risk reduction seen with finerenone in the FINEARTS-HF trial translates to fewer acute decompensation events — episodes where blood pressure drops, organs are underperfused, and the brain takes a hit. For caregivers managing a loved one with both heart failure and cognitive impairment, this is not a marginal improvement. Fewer hospitalizations also mean fewer episodes of delirium, which is itself a risk factor for accelerated dementia progression. That said, no heart failure drug has been specifically studied with cognitive outcomes as a primary endpoint. The brain benefits are inferred from cardiovascular improvements, not directly measured. If your loved one has both heart failure and dementia, the conversation with their cardiologist should explicitly include cognitive considerations — something that does not happen as often as it should.
Myqorzo and the New Approach to Hypertrophic Cardiomyopathy
Aficamten, branded as Myqorzo, earned FDA approval on December 19, 2025, for adults with symptomatic obstructive hypertrophic cardiomyopathy (oHCM) and became available in U.S. pharmacies in late January 2026. This is a different kind of heart disease than the chronic heart failure treated by finerenone, but it is no less debilitating. In oHCM, the heart muscle is abnormally thick, obstructing blood flow and causing symptoms ranging from severe shortness of breath to dangerous arrhythmias. In the SEQUOIA-HCM trial, aficamten improved peak oxygen uptake by 1.8 mL/kg/min over placebo at 24 weeks, alongside meaningful improvements in NYHA functional class and symptom scores.
It works as an oral, once-daily, selective, reversible cardiac myosin inhibitor — essentially dialing down the excessive contraction force that causes the obstruction. Aficamten competes directly with mavacamten (Camzyos), which was the first cardiac myosin inhibitor to reach the market, giving patients and clinicians a second option in a class that did not exist a few years ago. One critical detail: Myqorzo is available only through a Risk Evaluation and Mitigation Strategy (REMS) program because of the risk of systolic dysfunction. Patients must be enrolled and monitored, which adds a layer of logistical complexity. For older patients or those with cognitive impairment, navigating a REMS program can be genuinely burdensome, and caregivers should be prepared to manage the monitoring requirements.

Semaglutide for Heart Failure — Where Weight Loss Meets Cardiac Treatment
Semaglutide, already well known as the active ingredient in Wegovy for weight loss, is emerging as a potentially transformative treatment for heart failure with preserved ejection fraction in patients who are also obese. It is not yet FDA-approved for heart failure, but a potential approval for HFpEF in obese patients is anticipated in 2026 based on compelling trial data. The STEP-HFpEF trial demonstrated that semaglutide 2.4 mg produced approximately 11% greater weight loss compared to placebo over 52 weeks, but the story goes well beyond the scale. Patients experienced significantly improved symptoms, better physical function, greater six-minute walk distances, and higher quality-of-life scores as measured by the Kansas City Cardiomyopathy Questionnaire. A pooled analysis combining data from the SELECT, FLOW, STEP-HFpEF, and STEP-HFpEF DM trials further showed that semaglutide reduced the risk of the combined endpoint of cardiovascular death or worsening heart failure events.
The comparison with finerenone is instructive. Finerenone works regardless of body weight and targets the neurohormonal pathways driving heart failure. Semaglutide, by contrast, appears to derive much of its cardiac benefit from weight reduction and metabolic improvements, meaning its effects may be most pronounced in patients with obesity-related HFpEF. These are complementary approaches, not competitors, and some patients may eventually benefit from both. However, semaglutide’s gastrointestinal side effects — nausea, vomiting, diarrhea — can be particularly problematic in elderly patients, especially those who are already frail or have difficulty maintaining adequate nutrition.
Kidney Risks, Drug Interactions, and What Caregivers Need to Watch
The most significant safety concern with finerenone is its effect on kidney function. In the FINEARTS-HF trial, 18% of patients on finerenone experienced worsening renal function compared to 12% on placebo. For the dementia caregiving audience, this is particularly relevant because kidney disease and heart failure frequently coexist in older adults, and many dementia patients are already taking medications that affect kidney function. Hyperkalemia — dangerously elevated potassium levels — is another risk associated with MRAs, including finerenone. Patients on ACE inhibitors, ARBs, or potassium supplements require especially careful monitoring.
The practical implication for caregivers is straightforward: if a loved one starts finerenone, expect more frequent blood draws to check kidney function and potassium levels, particularly in the first few months. This can be distressing for patients with dementia who may not understand why they are being subjected to repeated lab work. Myqorzo carries its own distinct warning. The REMS requirement exists because cardiac myosin inhibitors can, in some patients, reduce the heart’s pumping ability too much, leading to systolic dysfunction. Regular echocardiograms are part of the monitoring protocol. For any patient with cognitive impairment, the question is whether the monitoring burden is manageable and whether the symptomatic benefits justify it.

What Is Coming Next in the Heart Failure Pipeline
Two pipeline developments are worth tracking in 2026. VS-041, developed by Vasa Therapeutics, is an oral small molecule targeting fibroinflammation in HFpEF. It has received FDA Fast Track designation, and its trial is expected to complete by July 2026. If successful, it would represent yet another mechanistic approach to HFpEF, attacking the inflammatory and fibrotic processes that stiffen the heart muscle.
The other is the FUROSCIX ReadyFlow Autoinjector (SCP-111), a subcutaneous furosemide injection that can be administered in under 10 seconds for edema management in chronic heart failure. Its PDUFA target action date is July 26, 2026. This device could be a practical game-changer for home-based care. Currently, many heart failure patients with severe fluid overload must visit an infusion center or emergency department for intravenous diuretics. A self-administered subcutaneous option could reduce hospital visits substantially — a meaningful benefit for dementia patients and their caregivers who find each hospital trip disorienting and exhausting.
The Bigger Picture for Heart and Brain Health
The convergence of new heart failure treatments arriving in 2025 and 2026 represents the most productive period in heart failure pharmacology in over a decade. For the first time, HFpEF patients have a dedicated approved therapy in finerenone, oHCM patients have a second myosin inhibitor option in aficamten, and the potential approval of semaglutide for cardiac indications could blur the lines between metabolic and cardiovascular medicine in ways that benefit both. For families navigating the intersection of heart disease and cognitive decline, these advances matter concretely.
Every prevented hospitalization is a disruption avoided. Every improvement in exercise capacity is a patient who can remain more active, more independent, and potentially more cognitively engaged. The drugs themselves will not reverse dementia, but they address one of its most powerful accelerants. The conversation between cardiologists, neurologists, and primary care physicians needs to catch up to the science — and caregivers may need to be the ones who push for it.
Conclusion
The heart failure treatment landscape has shifted meaningfully. Finerenone (Kerendia) stands out as the most significant recent approval, delivering a 16% reduction in cardiovascular death and heart failure events in a population — HFpEF patients — that previously had almost no effective pharmacological options. Alongside it, aficamten (Myqorzo) offers a new tool for hypertrophic cardiomyopathy, and semaglutide may soon earn approval for heart failure in obese patients based on the STEP-HFpEF data. Each drug carries its own risk profile, from finerenone’s kidney effects to Myqorzo’s REMS requirements to semaglutide’s gastrointestinal burden.
For caregivers and families dealing with both heart failure and dementia, the practical takeaway is to have direct conversations with the care team about whether these newer treatments are appropriate. Ask specifically about finerenone if your loved one has HFpEF. Ask about the monitoring burden and whether it is realistic given the patient’s cognitive status. And keep an eye on the 2026 pipeline — the FUROSCIX autoinjector in particular could make home-based heart failure management significantly more feasible.
Frequently Asked Questions
Is finerenone (Kerendia) the same as spironolactone?
No. Both are mineralocorticoid receptor antagonists, but finerenone is nonsteroidal, which means it avoids many of the hormonal side effects associated with spironolactone, such as breast tenderness and menstrual irregularities. They work on similar pathways but have different safety profiles.
Can semaglutide treat heart failure in patients who are not obese?
The current trial evidence, specifically the STEP-HFpEF data, focused on patients with HFpEF and obesity. Whether semaglutide benefits non-obese heart failure patients is not yet established, and it is not currently approved for any heart failure indication.
Does treating heart failure actually slow dementia progression?
No heart failure drug has been studied with dementia progression as a primary outcome. However, reducing heart failure hospitalizations and improving cardiac output may protect brain perfusion and reduce delirium episodes, both of which are associated with cognitive decline.
What is a REMS program, and why does Myqorzo require one?
A Risk Evaluation and Mitigation Strategy is an FDA-mandated safety program for drugs with serious potential risks. Myqorzo requires REMS because cardiac myosin inhibitors can cause systolic dysfunction — meaning the heart may pump too weakly — necessitating regular monitoring with echocardiograms.
How is Kerendia different from other heart failure drugs like sacubitril/valsartan (Entresto)?
Entresto is approved primarily for heart failure with reduced ejection fraction (HFrEF), while Kerendia is approved for patients with ejection fraction of 40% or greater (HFmrEF and HFpEF). They target different patient populations and work through different mechanisms, and in some cases may be used together.