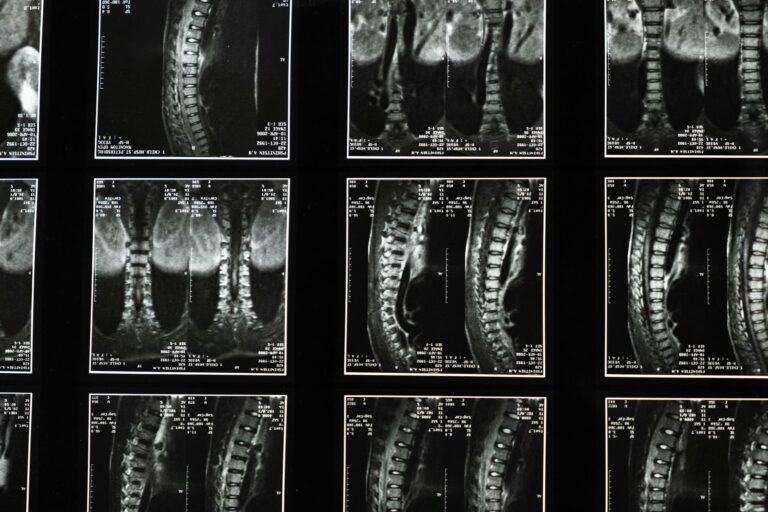
Lumbar spine degeneration is an inevitable part of aging for most people, affecting more than 80 percent of adults by age 50. Doctors identify nine main causes driving this process: age-related water loss in spinal discs, genetic predisposition, obesity, mechanical stress from work and daily activities, smoking, previous injuries, menopause-related hormone changes in women, repetitive twisting motions, and psychological stress. These factors don’t work in isolation—a 55-year-old construction worker with a family history of disc problems faces different risks than a sedentary office worker of the same age. Understanding what causes disc degeneration matters because it helps explain why some people develop painful symptoms while others with similar imaging results remain completely pain-free.
Most people worry that disc degeneration automatically means chronic pain or disability. That’s not accurate. Research shows that while over 90 percent of people over 50 have evidence of spinal degeneration on imaging, only about 5 percent actually experience symptomatic back pain from it. The difference lies in how these nine contributing factors accumulate in each person’s spine and how their body adapts to changes. This article walks through each cause doctors recognize, explains the mechanisms behind them, and shows how multiple factors interact to affect long-term spinal health.
Table of Contents
- How Genetics Shape Your Spinal Aging Timeline
- Weight, Cholesterol, and Metabolic Acceleration of Disc Aging
- Occupational and Mechanical Stressors Throughout Your Career
- How Smoking Accelerates the Degeneration Timeline
- Injury History and the Accumulation of Spinal Trauma
- Psychological Stress and Its Physical Effects on Spinal Health
- How These Nine Factors Interact and Progress
- Conclusion
How Genetics Shape Your Spinal Aging Timeline
Genetic predisposition stands out as the single most important predictor of lumbar disc degeneration—more influential than any lifestyle factor. Your inherited blueprint determines not only how quickly your discs age but also how your immune system responds to disc changes and inflammation. If your parents or grandparents experienced early disc problems, your risk increases substantially, regardless of how carefully you treat your back. The genetic component affects disc structure itself, the water content that discs naturally lose, and how vulnerable your discs are to injury.
This genetic reality shapes when degeneration appears. Some people show disc changes on imaging by age 20 (about 37 percent at this age), while others maintain healthier discs well into their 50s despite similar jobs and lifestyles. Recognizing your genetic risk doesn’t mean accepting inevitable pain—it means you have a baseline understanding of your spine‘s aging pattern. Someone with a strong family history of disc problems should pay particular attention to the modifiable factors like weight, ergonomics, and smoking, knowing that these protective measures matter more for their spine than for someone with a favorable genetic profile.

Weight, Cholesterol, and Metabolic Acceleration of Disc Aging
Obesity and elevated BMI directly accelerate lumbar disc degeneration, working alongside high LDL cholesterol to speed up the aging process. Extra weight increases mechanical load on the lower spine, which bears most of your body’s weight—the lumbar region handles disc degeneration in roughly 90 percent of cases because it absorbs forces with every step, bend, and movement. A person carrying 50 extra pounds isn’t just placing that load temporarily; they’re increasing compression on discs during hours of daily activity, from sitting to walking.
The metabolic component adds another layer. High cholesterol affects disc nutrition and may accelerate inflammatory processes within the disc itself. Here’s the important caveat: weight loss benefits the spine, but very rapid weight loss can sometimes cause muscle weakness that reduces spinal support—a reason why gradual, exercise-supported weight management typically works better than crash dieting for spine health. Even modest weight loss shows benefits, so someone 60 pounds overweight doesn’t need to reach an ideal weight to protect their discs; moving toward a healthier weight through sustainable changes provides measurable improvements in spinal loads and degeneration risk.
Occupational and Mechanical Stressors Throughout Your Career
Heavy lifting, forceful bending, vibration exposure, and poor ergonomics contribute significantly to disc degeneration, with certain occupations showing higher rates. Machine operators, carpenters, construction workers, and people who spend years in uncomfortable postures all face elevated risk. Repetitive torsional stress—the twisting motions involved in assembly line work, certain sports, or jobs requiring constant rotation—places particular strain on disc structures. The pattern is clear: repeated stress accumulates over decades, moving the degeneration timeline earlier than it would progress genetically alone.
A practical example: a warehouse worker performing heavy lifting for 25 years likely shows more disc degeneration at age 50 than a desk worker of the same age, despite both having the same genetic predisposition. However, socioeconomic factors confound this picture—people in physically demanding jobs often have less access to preventive healthcare, fitness facilities, and ergonomic interventions, making it difficult to isolate occupational stress from broader lifestyle factors. The protective approach involves addressing what you can control: using proper lifting technique, taking movement breaks, and investing in ergonomic workspace setup. For someone whose job requires repetitive stress, this becomes especially important.

How Smoking Accelerates the Degeneration Timeline
Smoking emerges as a recognized risk factor for lumbar disc degeneration, affecting both the mechanical resilience of discs and the body’s healing responses. The mechanism isn’t fully understood, but smoking likely impairs disc nutrition, reduces oxygen delivery to disc cells, and interferes with the anti-inflammatory processes that normally protect discs. Someone who smoked for 30 years might show disc degeneration patterns typical of someone 10 years older, depending on how heavily they smoked.
The important distinction: quitting smoking reduces future degeneration risk, but it doesn’t reverse existing disc damage. Someone discovering disc degeneration on an imaging study at age 55 who then quits smoking doesn’t erase past changes—but they do slow the progression of further degeneration. This distinction matters psychologically and practically. Smoking cessation remains valuable for spine health, even once degeneration is already visible, which means it’s never too late to reduce this particular risk factor.
Injury History and the Accumulation of Spinal Trauma
Previous back injuries, even minor ones, contribute to disc degeneration by accelerulating the timeline and increasing vulnerability to further damage. A person who experienced a significant back injury at age 25 may show degeneration patterns at 50 that would normally appear at 60 in someone without that injury history. The injury disrupts the disc’s internal structure, affects healing patterns, and may leave the spine with reduced resilience to future stress. Trauma doesn’t need to be severe—repeated minor injuries from sports, falls, or accidents accumulate over time.
Women experience a particular vulnerability window during menopause. The loss of estrogen that occurs during the climacteric (the 15-year transition period around menopause) is associated with accelerated lumbar disc degeneration. Estrogen appears to protect disc structure and support the inflammatory responses that normally maintain disc health; the hormonal shift can trigger rapid degeneration changes precisely when other aging factors are also accelerating. This isn’t just back pain—the hormonal component represents a distinct biological mechanism that affects spinal aging differently in women than in men, making menopause a notable inflection point for women’s spinal health.
Psychological Stress and Its Physical Effects on Spinal Health
Psychological distress and chronic stress emerge as recognized contributors to lumbar disc degeneration, operating through multiple pathways. Stress increases muscle tension in the back and neck, affects inflammatory markers throughout the body, and influences how people move and hold their posture. Someone experiencing prolonged anxiety or depression may unconsciously stiffen their back, creating sustained muscle tension that increases spinal loads. Socioeconomic stress compounds this—financial insecurity, work strain, and environmental stressors all correlate with increased disc degeneration risk.
The mechanism involves both direct physical effects and behavioral pathways. Stressed individuals may be less likely to exercise regularly, more likely to maintain poor posture during work, and more prone to develop habits (like smoking or poor sleep) that independently affect spine health. Addressing psychological well-being therefore has measurable spinal health benefits, though it’s rarely framed this way in discussions of back pain. Someone managing stress through regular movement, sleep improvement, and stress-reduction practices supports their spine alongside whatever genetic or occupational risks they carry.
How These Nine Factors Interact and Progress
Understanding lumbar disc degeneration requires recognizing that these nine causes don’t operate independently—they interact and amplify each other. A 52-year-old woman with genetic predisposition, elevated BMI, a 30-year history of shift work with poor ergonomics, previous back injuries, menopause occurring right now, and chronic work stress faces a very different degeneration picture than a 52-year-old man with the same genes but a desk job, healthy weight, and lower stress. The combination of factors determines both the pace of degeneration and the likelihood of symptomatic pain.
The progression follows a predictable pattern for most people. Disc water content naturally diminishes with age, visible on imaging by early adulthood in many people. By age 50, 80 percent of the population shows disc degeneration on MRI or CT, yet remain completely asymptomatic. The real clinical question becomes not whether degeneration will develop—it almost certainly will—but whether modifiable factors are controlled well enough to prevent symptomatic pain and maintain function across decades of life.
Conclusion
Lumbar spine degeneration represents one of the most common age-related changes doctors observe, driven by a combination of genetic, mechanical, metabolic, hormonal, and psychological factors. While genetics sets the baseline timeline, the other eight causes offer genuine opportunities for intervention: weight management, occupational ergonomics, smoking cessation, stress management, and preventing repeat injuries all slow progression. Someone with strong genetic risk can substantially delay symptoms by controlling modifiable factors; conversely, even favorable genetics don’t guarantee protection if someone combines occupational stress, obesity, smoking, and poor ergonomics. The most important takeaway is the distinction between having disc degeneration and developing pain from it.
Over 90 percent of adults over 50 have degenerative changes visible on imaging, yet most never experience symptoms. This gap between imaging findings and actual symptoms means that detecting degeneration doesn’t automatically warrant aggressive treatment or lifestyle restriction. Instead, it provides an opportunity for informed prevention—managing weight, maintaining activity and movement, addressing psychological stress, and protecting the spine from trauma or poor ergonomics. These factors matter most not in the early stages when imaging shows changes but no pain exists, but in maintaining functional capacity across the decades when degeneration naturally progresses.