Pelvic instability occurs when the bones, ligaments, and muscles that form the pelvic ring lose their ability to maintain proper alignment and support, and the seven most common causes are ligamentous laxity, traumatic fractures, pregnancy-related changes, sacroiliac joint dysfunction, muscular weakness or imbalance, degenerative joint disease, and postoperative complications following pelvic surgery. For older adults, particularly those living with dementia or cognitive decline, pelvic instability carries outsized risks because it dramatically increases the likelihood of falls, chronic pain, and progressive immobility — all of which can accelerate cognitive deterioration and reduce quality of life. Consider a 74-year-old woman with moderate Alzheimer’s disease who begins refusing to walk.
Her caregivers assume the reluctance is behavioral, but an evaluation reveals that degenerative changes in her sacroiliac joints have created enough pelvic instability that standing causes significant pain she cannot articulate. This scenario plays out regularly in memory care settings, where communication barriers mask treatable physical conditions. Understanding the specific causes of pelvic instability matters because each one demands a different clinical response, and misidentification — or worse, no identification at all — leads to unnecessary suffering and functional decline. This article examines each of the seven causes in detail, explains how they intersect with aging and cognitive impairment, and outlines what caregivers and clinicians should watch for.
Table of Contents
- What Causes Pelvic Instability in Older Adults and Why Does It Matter?
- Ligamentous Laxity and How It Undermines the Pelvic Ring
- Traumatic Pelvic Fractures and Their Long-Term Consequences
- Sacroiliac Joint Dysfunction Versus Muscular Weakness — Distinguishing Between Causes
- Degenerative Joint Disease and Postoperative Complications
- Pregnancy-Related Pelvic Changes That Persist Decades Later
- Emerging Approaches and What the Future Holds for Pelvic Stability in Aging Populations
- Conclusion
- Frequently Asked Questions
What Causes Pelvic Instability in Older Adults and Why Does It Matter?
The pelvis is not a single bone but a ring of three major structures — the two innominate bones and the sacrum — held together by some of the strongest ligaments in the human body. Stability depends on the interplay between these bony structures, the ligaments that bind them, and the muscles that control movement across the pelvic joints. When any component of this system fails, the entire ring becomes compromised. In younger populations, high-energy trauma is the usual culprit. In older adults, the causes tend to be slower and more insidious: gradual ligament degeneration, muscle wasting from inactivity, osteoporotic bone loss, or the cumulative effects of joint disease. What makes pelvic instability particularly dangerous in dementia care is the feedback loop it creates. Pain and instability reduce mobility.
Reduced mobility accelerates muscle loss and bone weakening. Weaker muscles and bones increase instability further. For a person with dementia who already struggles with balance, spatial awareness, and the ability to report symptoms, this cycle can progress rapidly before anyone recognizes what is happening. Research published in the Journal of the American Geriatrics Society has shown that pelvic pain is significantly underdiagnosed in patients with cognitive impairment, partly because standard assessment tools rely on self-reporting. Compared to hip or knee instability, pelvic instability is harder to detect on routine examination. There is no single obvious joint to test. The pelvis moves subtly, and its dysfunction often presents as vague low back pain, groin discomfort, or simply a change in gait that gets attributed to “old age” or the progression of dementia itself.

Ligamentous Laxity and How It Undermines the Pelvic Ring
The sacroiliac ligaments, the sacrospinous and sacrotuberous ligaments, and the pubic symphysis ligaments all work together to keep the pelvic ring stable under load. When these ligaments become lax — whether from hormonal changes, chronic inflammation, or the natural loss of collagen density that accompanies aging — the joints they support begin to move beyond their normal range. This excess motion, even if measured in millimeters, is enough to generate pain and alter how forces travel through the pelvis during walking and standing. Ligamentous laxity as a cause of pelvic instability is particularly relevant in women, who have naturally wider pelvic anatomy and who may carry the lasting effects of pregnancies that stretched these ligaments decades earlier.
However, it is a mistake to assume this is exclusively a female problem. Men with chronic inflammatory conditions such as ankylosing spondylitis can develop significant ligamentous damage over time, and prolonged corticosteroid use — common in many older adults for conditions ranging from COPD to autoimmune disease — weakens connective tissue throughout the body, including the pelvic ligaments. One important limitation of treating ligamentous laxity is that once ligaments have stretched or degenerated beyond a certain point, they do not tighten back up on their own. Strengthening the surrounding muscles can compensate to a degree, but if a patient with dementia cannot participate meaningfully in a rehabilitation program, the options narrow considerably. Prolotherapy and other injection-based treatments have shown some promise in research settings, but evidence remains mixed, and these procedures require a patient who can communicate their pain levels during and after treatment — a significant barrier in advanced dementia.
Traumatic Pelvic Fractures and Their Long-Term Consequences
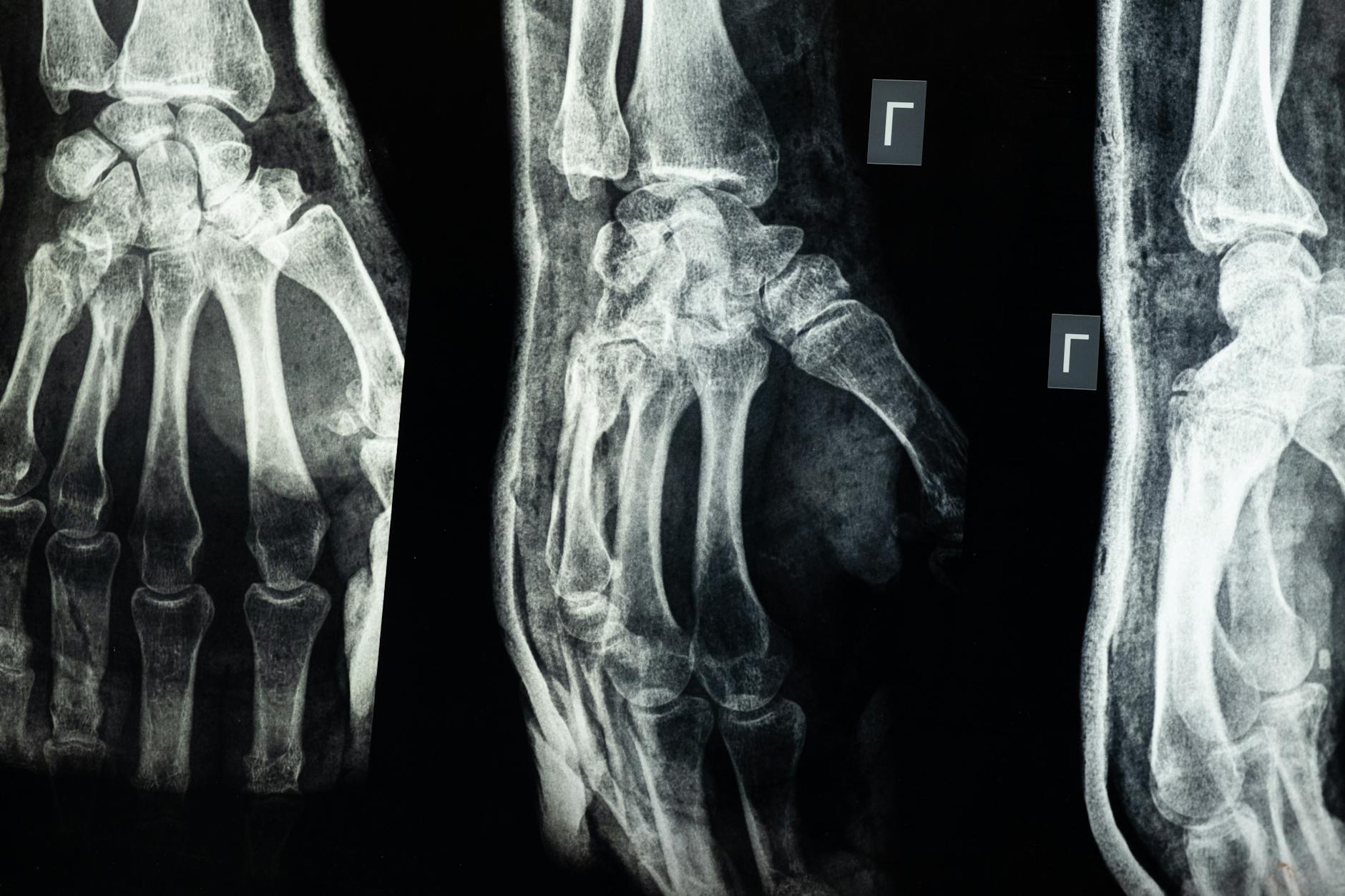
Falls are the leading cause of traumatic pelvic fractures in people over 65, and people with dementia fall at roughly twice the rate of cognitively intact older adults. The fractures that result are often different from those seen in younger patients. Rather than the high-energy ring disruptions caused by car accidents, elderly patients typically sustain insufficiency fractures — breaks through bone that has already been weakened by osteoporosis. These fractures may involve the pubic rami, the sacrum, or both, and they frequently go undiagnosed initially because they do not always appear on standard X-rays. CT scans or MRI are often needed to confirm the injury.
A specific and common example involves sacral insufficiency fractures, which account for an estimated 1 to 5 percent of all fragility fractures but are missed on initial imaging in up to 60 percent of cases. The patient presents with vague low back or buttock pain, the X-ray looks unremarkable, and the pain gets attributed to muscle strain or arthritis. In a dementia patient who cannot clearly describe where the pain is or how it started, weeks can pass before the fracture is identified — if it is identified at all. Even when pelvic fractures heal, the resulting scar tissue and subtle changes in alignment can leave permanent instability. The pelvis may bear weight asymmetrically, altering gait mechanics and placing abnormal stress on the hip joints, lumbar spine, and the opposite side of the pelvis. For someone already navigating the cognitive challenges of dementia, this physical asymmetry adds another layer of fall risk that compounds over time.
Sacroiliac Joint Dysfunction Versus Muscular Weakness — Distinguishing Between Causes
Sacroiliac joint dysfunction and core muscular weakness are frequently confused with each other because they produce overlapping symptoms: low back pain, difficulty with transitions like sitting to standing, and an unsteady gait. The distinction matters because the treatments diverge significantly. SI joint dysfunction often responds to manual therapy, joint stabilization belts, or in refractory cases, surgical fusion. Muscular weakness requires progressive strengthening, which means sustained physical therapy engagement. The tradeoff for clinicians managing dementia patients is that accurate diagnosis typically requires the patient’s active participation. Provocative tests for SI joint dysfunction — such as the FABER test, Gaenslen’s test, or the compression test — rely on the patient reporting where and when they feel pain.
In someone with moderate to severe dementia, these tests become unreliable. Diagnostic injections into the SI joint, which are considered the gold standard for confirming SI joint pathology, require informed consent and post-procedure pain reporting that may exceed the patient’s cognitive capacity. Muscular weakness in the pelvic stabilizers — the gluteus medius, gluteus maximus, deep hip rotators, and the muscles of the pelvic floor — develops predictably with inactivity. A person with dementia who spends most of the day seated will lose roughly 1 to 3 percent of muscle mass per week during periods of immobility, according to data from the European Working Group on Sarcopenia. The resulting weakness does not just affect the pelvis; it reshapes the entire kinetic chain, often manifesting first as a Trendelenburg gait pattern where the pelvis drops on one side during single-leg stance. Caregivers may notice this as a pronounced limp or waddle before any formal assessment takes place.
Degenerative Joint Disease and Postoperative Complications
Osteoarthritis of the pubic symphysis and sacroiliac joints progresses slowly but relentlessly in many older adults. The cartilage surfaces that normally allow smooth, minimal motion at these joints break down, bone spurs form, and the joint capsules stiffen unevenly. Paradoxically, this stiffening can create instability rather than prevent it, because the joint loses its ability to distribute forces evenly and begins to move abnormally under load. In the pubic symphysis, degenerative changes can widen the joint gap, creating a measurable instability that worsens with walking. Postoperative pelvic instability is a less common but serious cause that deserves attention.
Patients who have undergone pelvic surgery — for cancer, fracture fixation, or gynecological or urological procedures — may develop instability if hardware fails, bone grafts do not incorporate, or surgical removal of tissue changes the balance of forces across the pelvic ring. A warning that applies specifically to dementia care: patients with cognitive impairment are at higher risk of noncompliance with postoperative weight-bearing restrictions. A patient who does not remember they had surgery three days ago may attempt to stand and walk without assistance, placing catastrophic loads on a pelvis that has not yet healed. This is one area where dementia-specific care planning makes a genuine difference. Postoperative protocols for cognitively intact patients assume the person understands and will follow instructions. For someone with dementia, the care plan must account for the likelihood that the patient will not remember the restrictions, and environmental modifications — bed alarms, low beds, physical barriers, one-to-one supervision during the healing period — become essential rather than optional.
Pregnancy-Related Pelvic Changes That Persist Decades Later
While pregnancy is typically associated with younger women, its effects on pelvic stability can persist for life and become clinically significant in old age. The hormone relaxin, produced during pregnancy to loosen the pelvic ligaments for delivery, causes structural changes that do not always fully reverse postpartum.
Women who experienced symphysis pubis dysfunction or significant pelvic girdle pain during pregnancy are at elevated risk of developing chronic pelvic instability later in life, particularly as the muscular compensation they developed over the years erodes with age-related sarcopenia. A telling example is the woman in her late seventies who reports that her pelvic pain “feels exactly like it did when I was pregnant fifty years ago.” This is not coincidence or imagination — the same structural vulnerability that caused symptoms during pregnancy has resurfaced because the muscles that were compensating for the ligamentous laxity have weakened below the threshold needed to maintain stability. In dementia care, this history may be available from family members even when the patient can no longer provide it, making thorough intake conversations with families especially valuable.
Emerging Approaches and What the Future Holds for Pelvic Stability in Aging Populations
Research into pelvic instability in older adults is increasingly recognizing the role of the neuromuscular system — not just whether muscles are strong enough, but whether the brain can coordinate them effectively. This is directly relevant to dementia care, because the same neurodegenerative processes that impair memory and cognition also degrade the motor planning and proprioceptive feedback loops that keep the pelvis stable during movement. Early-stage trials of neuromuscular electrical stimulation for pelvic stabilization in patients who cannot participate in traditional exercise programs have shown modest but encouraging results.
There is also growing interest in wearable sensor technology that can detect changes in gait symmetry and pelvic motion before they become clinically obvious. For dementia care facilities, these tools could provide early warning of developing pelvic instability, allowing intervention before the first fall rather than after. The technology is not yet widely available or validated for this specific application, but several clinical trials are underway, and the trajectory of the field suggests that passive monitoring will become a standard component of fall prevention in memory care settings within the next decade.
Conclusion
Pelvic instability in older adults arises from a convergence of causes — ligament degeneration, fractures, joint disease, muscular atrophy, surgical complications, hormonal legacies, and neuromuscular decline — that rarely occur in isolation. For people living with dementia, every one of these causes is harder to detect, harder to treat, and more dangerous in its consequences. The communication barriers inherent in cognitive impairment mean that caregivers and clinicians must be proactive rather than reactive, looking for behavioral changes, gait alterations, and reluctance to move as potential signals of an underlying structural problem.
The most important step any caregiver or care team can take is to resist the assumption that mobility decline in a person with dementia is simply “part of the disease.” It may be, but it may also be a treatable mechanical problem that, once identified, can be managed in ways that meaningfully preserve independence and reduce suffering. A thorough musculoskeletal assessment, including imaging when indicated, should be part of the evaluation whenever a dementia patient shows a significant change in mobility, balance, or willingness to bear weight. Early identification of pelvic instability does not guarantee a fix, but it opens the door to targeted interventions that can slow the cycle of decline.
Frequently Asked Questions
Can pelvic instability cause dementia symptoms to worsen?
Indirectly, yes. Chronic pain from pelvic instability can increase agitation, disrupt sleep, and reduce mobility — all of which are associated with faster cognitive decline in dementia. Pain itself consumes cognitive resources, and in a brain already under siege from neurodegeneration, that additional burden can noticeably affect function.
How is pelvic instability diagnosed in someone who cannot describe their symptoms?
Clinicians rely on observational signs: changes in gait pattern, reluctance to bear weight, guarding behavior during transfers, facial grimacing, and increased agitation. Imaging — particularly CT or MRI of the pelvis — can identify structural causes without requiring patient participation. Diagnostic SI joint injections are sometimes used but require careful consideration of consent issues in dementia.
Is pelvic instability the same as a hip problem?
No, though they are frequently confused. The hip joint is where the femur meets the pelvis; pelvic instability involves the joints within the pelvic ring itself — the sacroiliac joints and the pubic symphysis. However, the two conditions can coexist and exacerbate each other, and pain from one can be referred to the region of the other.
What is the best exercise for pelvic stability in older adults?
For those who can participate, targeted strengthening of the gluteus medius, transverse abdominis, and pelvic floor muscles provides the most direct benefit. Exercises like clamshells, bridges, and supported single-leg stance are commonly prescribed. However, the “best” exercise is the one the patient will actually perform consistently, which in dementia care often means simplified movements incorporated into daily routines rather than formal exercise sessions.
Should a pelvic support belt be used for someone with dementia and pelvic instability?
Pelvic support belts can provide meaningful symptom relief for SI joint dysfunction and pubic symphysis instability. In dementia care, the practical challenge is that patients may remove the belt, find it distressing, or not understand its purpose. A well-fitted belt worn during weight-bearing activities can help, but it should be introduced gradually and monitored for skin integrity, especially in patients who cannot report discomfort from an ill-fitting device.





