Lumbar spine instability occurs when the vertebrae in the lower back lose their ability to maintain normal alignment and controlled movement under everyday loads, and the eight signs most commonly associated with it are recurrent episodes of the back “giving way,” pain that worsens with prolonged sitting or standing, a catching or locking sensation during movement, muscle spasms that seem disproportionate to the activity, pain that temporarily improves with a change of position but always returns, difficulty transitioning from sitting to standing, a visible shift in posture during flare-ups, and neurological symptoms like tingling or weakness in the legs. A 68-year-old woman who finds herself gripping the armrests every time she stands from a chair because her lower back feels like it might buckle is not simply dealing with “normal aging.” That pattern, especially when it comes and goes unpredictably, points toward a spine that has lost some of its mechanical integrity.
This matters on a dementia care and brain health website because lumbar spine instability directly increases fall risk, limits physical activity, disrupts sleep, and compounds cognitive decline in older adults. Pain that is poorly managed or misunderstood often leads to social withdrawal, reduced exercise, and increased reliance on medications that carry their own cognitive side effects. The article ahead breaks down each of the eight warning signs in detail, explains how they differ from ordinary back pain, discusses the connection between spinal instability and brain health, and outlines both conservative and surgical options so caregivers and patients can have informed conversations with their medical teams.
Table of Contents
- What Are the Early Warning Signs of Lumbar Spine Instability?
- How Lumbar Instability Differs from Ordinary Lower Back Pain
- The Connection Between Spinal Instability and Cognitive Health in Older Adults
- Conservative Treatment Options and Their Tradeoffs
- When Surgery Becomes Part of the Conversation
- How Caregivers Can Monitor and Document Symptoms
- Emerging Approaches and What to Watch For
- Conclusion
- Frequently Asked Questions
What Are the Early Warning Signs of Lumbar Spine Instability?
The earliest and most telling sign is what clinicians call “instability catch,” a sudden, sharp pain during a specific arc of movement, often bending forward or straightening up, that forces you to pause or shift direction mid-motion. Unlike a pulled muscle, which tends to hurt consistently, this catch appears at one particular angle and then vanishes once you move past it. The second early sign is recurrent episodes of the lower back “giving way,” where the spine momentarily feels unsupported, as though the muscles have simply quit. A retired schoolteacher might notice this while bending to load the dishwasher: one day the back holds fine, the next day the same motion triggers a frightening sensation of collapse. The unpredictability is the hallmark. Ordinary disc pain is more constant and position-dependent.
Instability pain is episodic, positional, and often accompanied by a reflexive muscle spasm the body uses as an emergency braking system. The third early indicator is pain that temporarily resolves with a change in position but never stays gone. Someone with lumbar instability might feel relief the moment they recline, only to have the pain return the instant they sit upright again. This differs from spinal stenosis, where walking triggers symptoms and sitting provides lasting relief, or from a herniated disc, where one specific posture is consistently worse. With instability, the common thread is that no single position holds for long. Caregivers should pay attention to a loved one who seems to be constantly fidgeting, shifting weight, or standing up and sitting back down repeatedly. That restlessness is often not anxiety or cognitive agitation; it is a spine that cannot find a stable resting state.

How Lumbar Instability Differs from Ordinary Lower Back Pain
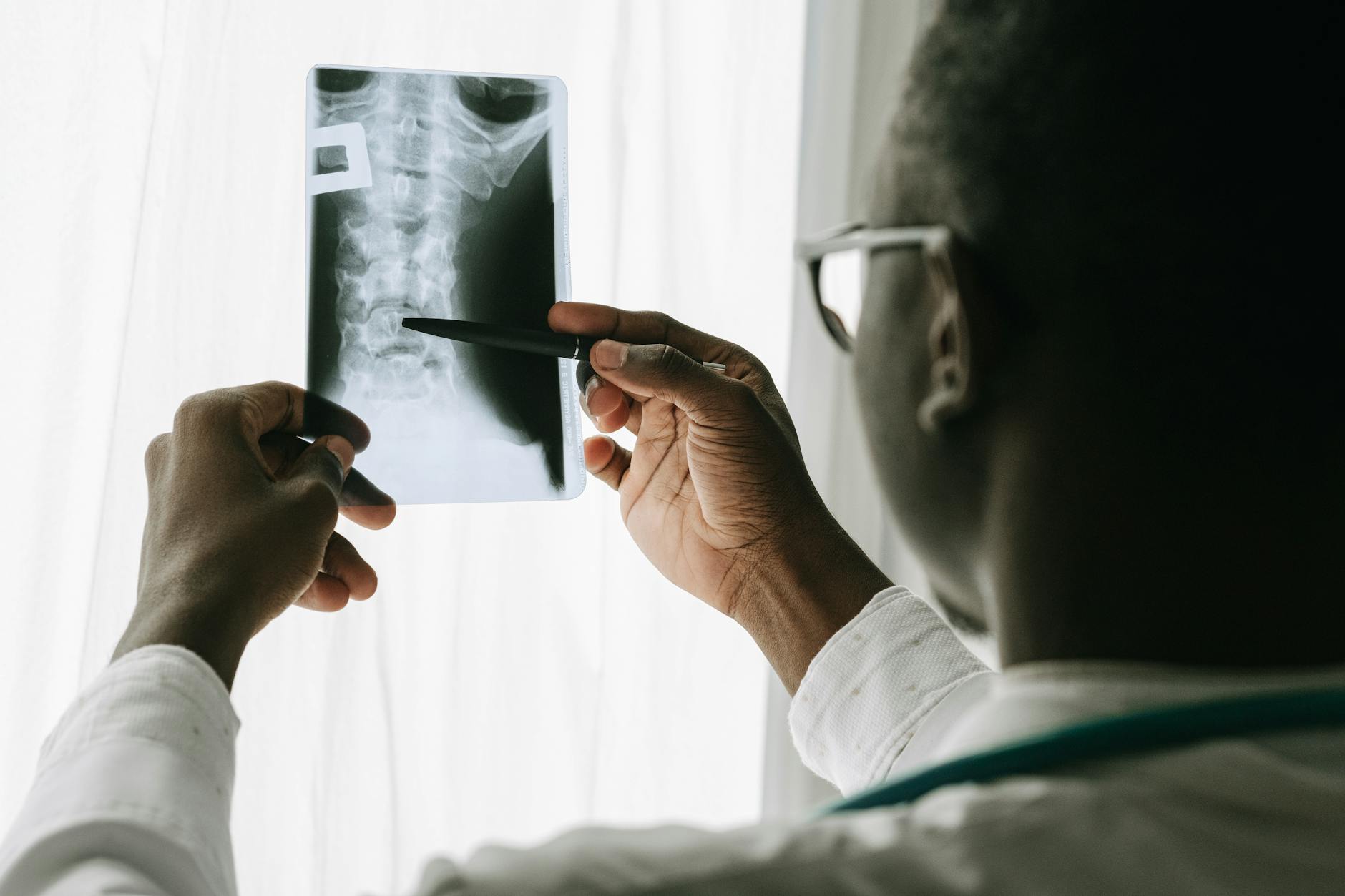
Ordinary mechanical low back pain, the kind that follows a weekend of yard work or an awkward lift, tends to follow a predictable course: it hurts, it gradually improves with rest and anti-inflammatories, and it resolves within a few weeks. Lumbar instability does not behave this way. Its fourth hallmark sign is a pattern of recurrence where flare-ups seem to arrive without a proportionate trigger. A person may feel fine for a week or two and then experience severe pain after something as minor as reaching for a coffee cup. Imaging studies help clarify the distinction. Flexion-extension X-rays, where the patient bends forward and then arches backward while films are taken, can reveal abnormal translation, meaning one vertebra sliding more than about three millimeters relative to its neighbor.
MRI may show disc degeneration or facet joint arthropathy, but these findings alone do not confirm instability. Many people over sixty have degenerative discs on MRI and no symptoms whatsoever. However, if a patient has both the clinical pattern of episodic, position-shifting pain and imaging that shows segmental hypermobility, the diagnosis becomes much more reliable. The fifth sign, muscle spasms that seem disproportionate to the activity, is the body’s attempt to splint an unstable segment. These spasms can be severe enough to make someone look “locked up,” unable to straighten fully for hours or even days. In older adults, particularly those with mild cognitive impairment, these episodes are sometimes mistaken for a stroke or a fall-related injury because the person may not be able to clearly articulate what happened. Caregivers should be aware that a sudden inability to stand upright, combined with visible paraspinal muscle tightness, warrants evaluation for spinal instability rather than an automatic trip to the neurologist for stroke workup, though stroke should always be ruled out when there is any doubt.
The Connection Between Spinal Instability and Cognitive Health in Older Adults
The sixth sign, difficulty transitioning from sitting to standing, has outsized consequences for brain health. Research consistently shows that reduced physical mobility accelerates cognitive decline, in part because cardiovascular fitness supports cerebral blood flow, and in part because social engagement drops when a person cannot move comfortably. A 2019 study in the Journal of the American Geriatrics Society found that older adults with chronic low back pain scored lower on tests of processing speed and executive function compared to pain-free peers, even after adjusting for age, education, and depression. The mechanism is not fully settled, but chronic pain is known to alter the structure of the prefrontal cortex and hippocampus over time, the same regions that deteriorate in Alzheimer’s disease. For someone already living with early-stage dementia, lumbar spine instability creates a vicious feedback loop. The pain limits walking.
Less walking means less aerobic exercise, which is one of the few interventions with consistent evidence for slowing cognitive decline. Reduced mobility increases fall risk, and falls are the leading cause of traumatic brain injury in adults over 65. The fear of falling leads to further activity restriction, social isolation, depression, and faster cognitive deterioration. A practical example: a man with moderate Alzheimer’s who also has an unstable L4-L5 segment may stop attending his weekly walking group because his back “acts up” unpredictably. Within months, his caregiver notices increased confusion, sundowning, and agitation. The cognitive worsening is not necessarily the natural progression of his disease alone; it is compounded by the loss of his most important non-pharmacological therapy, regular physical movement.
Conservative Treatment Options and Their Tradeoffs
The seventh sign, a visible shift in posture during flare-ups, often motivates patients and families to seek treatment. The first-line approach is almost always conservative: physical therapy focused on core stabilization, activity modification, and sometimes bracing. The goal of physical therapy is to train the deep stabilizing muscles, particularly the multifidus and transversus abdominis, to compensate for what the passive structures (discs, ligaments, facet joints) can no longer control. When it works, and it does work for a meaningful percentage of patients, the results can be durable. A well-designed stabilization program practiced consistently for twelve to sixteen weeks can reduce pain episodes by half or more. The tradeoff is that physical therapy demands consistent participation and a certain baseline cognitive capacity.
A person with moderate to advanced dementia may not be able to follow verbal cuing for specific muscle activation, remember to do home exercises, or even understand why they are being asked to lie on a mat and contract their abdomen. In these cases, caregivers and therapists need to shift toward simpler movement strategies: supported walking programs, aquatic therapy where the buoyancy offloads the spine, and functional training that focuses on safe sit-to-stand mechanics rather than isolated muscle drills. Bracing is a double-edged tool. A lumbar corset can reduce pain during activities, but wearing one for extended periods weakens the very muscles that need to get stronger. The general recommendation is to use a brace during high-demand tasks, grocery shopping, longer walks, and to leave it off during rest and light activity at home. For patients who cannot manage this on-and-off schedule independently, a caregiver needs to take on that responsibility.
When Surgery Becomes Part of the Conversation
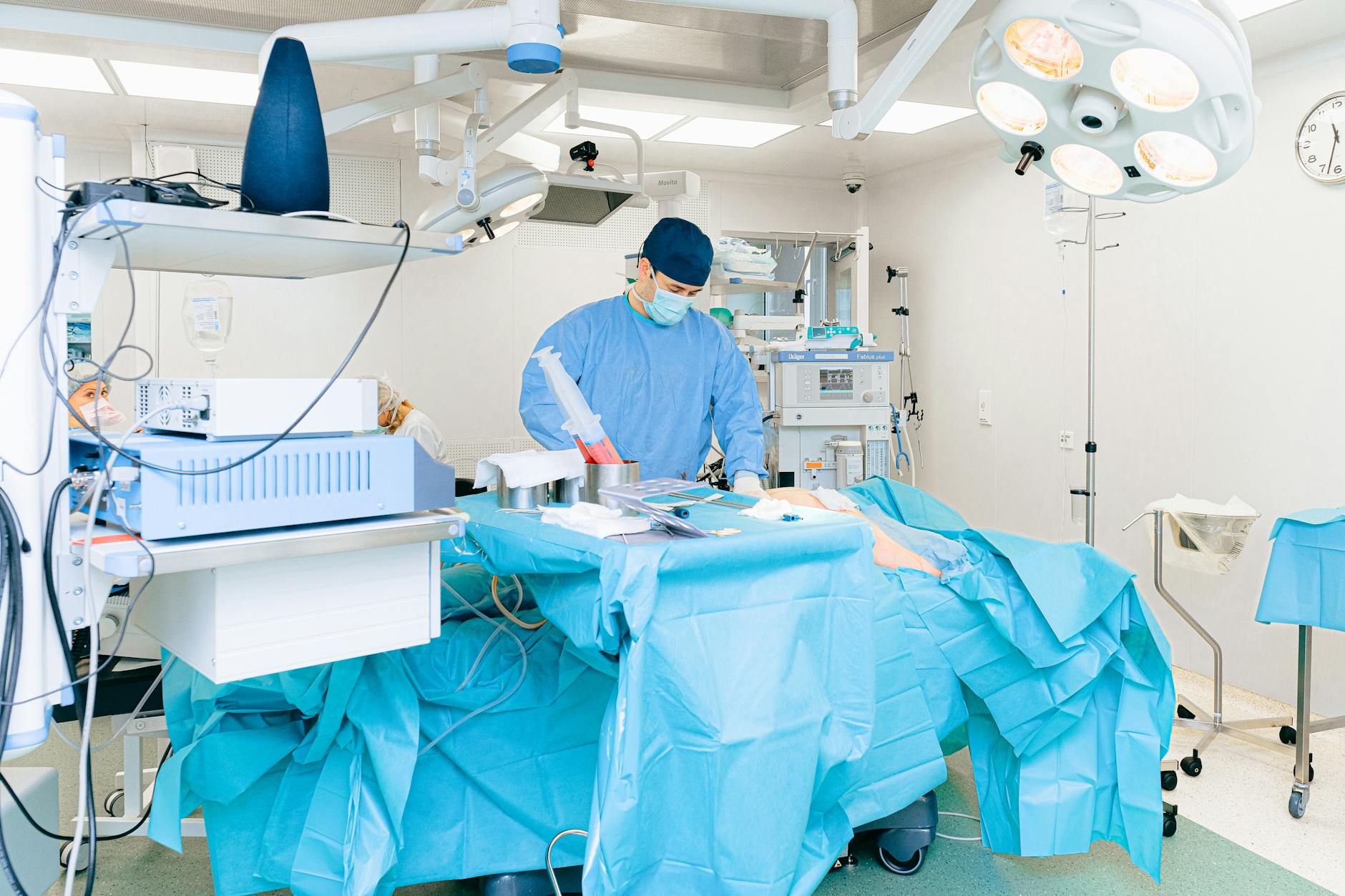
The eighth and most concerning sign is neurological involvement: tingling, numbness, or frank weakness in one or both legs, sometimes accompanied by changes in bladder or bowel control. When instability causes a vertebra to shift enough to compress nerve roots or the spinal canal itself, conservative treatment may not be sufficient. Spinal fusion, the most common surgical intervention for lumbar instability, aims to permanently lock the unstable segment in place using hardware and bone graft. Success rates for pain relief hover around 70 to 80 percent in well-selected patients, but the surgery carries real risks for older adults: infection, hardware failure, adjacent segment degeneration (where the levels above or below the fusion break down faster because they now absorb more stress), and the general anesthetic risks that increase with age and comorbidity. For patients with dementia, the surgical calculus becomes especially difficult.
General anesthesia is associated with postoperative cognitive dysfunction, a temporary but sometimes prolonged worsening of confusion, memory, and orientation. In someone whose cognitive reserves are already depleted, “temporary” can stretch into weeks or months, and the postoperative rehabilitation demands, including movement restrictions, wound care, and medication management, fall almost entirely on caregivers. This does not mean surgery is never appropriate in a person with cognitive impairment. If a patient is losing the ability to walk because of nerve compression and conservative measures have failed, fusion may preserve functional independence that would otherwise be permanently lost. The decision requires an honest conversation between the surgeon, the primary care physician, the patient (to whatever extent they can participate), and the family about goals of care, risk tolerance, and what “success” realistically looks like for that individual.
How Caregivers Can Monitor and Document Symptoms
Caregivers are often the first to notice the signs of lumbar instability because the patient, particularly one with cognitive impairment, may not report symptoms accurately or consistently. Keeping a simple symptom diary can be invaluable for medical appointments.
Note the date, what the person was doing when symptoms appeared, which signs were present (catching, giving way, spasm, postural shift, leg symptoms), how long the episode lasted, and what helped. For example: “March 4, stood up from recliner, grabbed table edge, said back ‘went out,’ walked hunched for about twenty minutes, improved after lying flat.” Two or three weeks of entries like this give a spine specialist far more diagnostic information than a single office visit where the patient may feel fine and move normally.
Emerging Approaches and What to Watch For
The treatment landscape for lumbar instability is shifting. Regenerative approaches, including platelet-rich plasma injections into damaged facet joints and ongoing clinical trials of disc cell therapies, aim to restore some structural integrity without fusion. None of these are standard of care yet, and older adults should be cautious about clinics marketing unproven stem cell treatments at high out-of-pocket cost.
More immediately promising is the growing integration of wearable inertial sensors that can objectively measure spinal movement patterns outside the clinic. Within the next several years, it may become routine for a patient to wear a small sensor on their lower back for a week, generating data that quantifies exactly how much abnormal motion is occurring and during which daily activities. For caregivers managing a loved one with both spinal instability and cognitive decline, this kind of objective monitoring could replace the guesswork that currently dominates the diagnostic process and help clinicians intervene earlier, before a fall changes everything.
Conclusion
Lumbar spine instability is not just a back problem. In older adults, and particularly in those with cognitive impairment, it is a mobility problem, a fall-risk problem, a sleep problem, and ultimately a brain health problem. The eight signs, episodic giving way, instability catch, position-dependent pain that never settles, disproportionate muscle spasms, recurrence without proportionate triggers, difficulty with sit-to-stand transitions, visible postural shifts, and neurological symptoms in the legs, form a recognizable pattern that distinguishes this condition from the ordinary aches of aging. Early recognition matters because early intervention is simpler and more effective.
A targeted physical therapy program started when symptoms are mild has a much better chance of succeeding than one initiated after months of deconditioning and pain avoidance. Caregivers should document what they observe, advocate for flexion-extension imaging when the clinical picture fits, and have direct conversations with medical providers about how treatment plans will account for any cognitive limitations. The spine and the brain do not exist in separate silos. Protecting one means protecting both.
Frequently Asked Questions
Can lumbar spine instability cause falls in people with dementia?
Yes. The episodic nature of instability, where the back suddenly gives way without warning, is a direct fall risk. In someone with dementia who may already have impaired balance, slower reaction times, and difficulty processing spatial information, an unstable lumbar segment significantly increases the likelihood of a fall. This is one of the strongest reasons to pursue diagnosis and treatment rather than attributing symptoms to “just getting older.”
Is it safe to do physical therapy if someone has moderate dementia?
It can be, but the program needs to be adapted. Traditional core stabilization exercises require the patient to understand and follow specific instructions for muscle activation, which may not be feasible. Therapists experienced with cognitively impaired patients focus on functional movements, walking programs, sit-to-stand practice with support, and aquatic therapy. Caregiver involvement in sessions is usually essential so exercises can be reinforced at home.
How is lumbar instability diagnosed if the person cannot describe their symptoms clearly?
Observation and imaging carry most of the diagnostic weight. Caregivers can provide symptom diaries documenting what they see: episodes of the back giving way, difficulty standing, postural changes. Flexion-extension X-rays are the key imaging study and require only that the patient bend forward and backward, which can usually be accomplished with guidance. MRI provides supplementary information about disc and nerve status.
Does lumbar fusion worsen dementia?
Fusion surgery does not cause dementia, but general anesthesia is associated with postoperative cognitive dysfunction that can temporarily worsen confusion and memory in people who already have cognitive impairment. The effect is usually reversible over weeks to months, but in some cases the recovery is prolonged. This risk needs to be weighed against the potential benefit of preserving mobility.
Are there medications specifically for lumbar instability?
No medication treats the mechanical instability itself. Medications are used to manage symptoms: NSAIDs or acetaminophen for pain, muscle relaxants for spasm, and in some cases gabapentin or pregabalin for nerve-related leg symptoms. In older adults with dementia, medication choices must account for cognitive side effects. Muscle relaxants and gabapentinoids can both increase confusion and fall risk, so they should be used cautiously and at the lowest effective dose.
When should a caregiver push for a specialist referral?
If a primary care provider attributes recurrent episodes of the back giving way, progressive difficulty walking, or new leg weakness to “normal aging” without ordering flexion-extension X-rays or referring to a spine specialist, it is reasonable to advocate for further evaluation. These symptoms are not a normal part of aging and have specific, treatable causes.





