Doctors are prescribing prophylactic antibiotics — most commonly amoxicillin — before certain cardiac procedures because bacteria that enter the bloodstream during invasive work can lodge on damaged or artificial heart valves, causing a potentially fatal infection called infective endocarditis. For patients with specific heart conditions, a single dose of antibiotics taken roughly an hour before the procedure can dramatically reduce this risk. Consider a 72-year-old woman with a mechanical aortic valve who needs a dental extraction: without that pre-procedure antibiotic, oral bacteria dislodged during the extraction could colonize her prosthetic valve, leading to weeks of intravenous antibiotics or emergency open-heart surgery. For her, the one pill is a straightforward safeguard.
This practice, known as antibiotic prophylaxis, has been refined considerably over the past two decades. The American Heart Association narrowed its guidelines in 2007 and again in subsequent updates, limiting routine prophylaxis to only the highest-risk patients rather than the broad population that once received it. The shift reflects growing concern about antibiotic resistance and the recognition that everyday activities like brushing teeth introduce bacteria into the blood far more often than a single dental visit. This article covers who actually needs prophylactic antibiotics before cardiac procedures, which drugs are used, what the current evidence says about effectiveness, and why patients with cognitive decline or dementia face unique challenges in following these protocols.
Table of Contents
- Why Do Cardiologists Recommend Antibiotics Before Heart Procedures?
- Which Heart Conditions Actually Require Prophylactic Antibiotics?
- The Connection Between Oral Health, Heart Disease, and Cognitive Decline
- How Caregivers Can Manage Antibiotic Prophylaxis for Patients With Dementia
- Risks of Antibiotic Prophylaxis and When It May Do More Harm Than Good
- What Happens When Prophylaxis Is Missed
- Evolving Guidelines and What May Change in Coming Years
- Conclusion
- Frequently Asked Questions
Why Do Cardiologists Recommend Antibiotics Before Heart Procedures?
The core concern is infective endocarditis, an infection of the heart’s inner lining or valves that carries a mortality rate between 15 and 30 percent even with aggressive treatment. When a procedure disrupts tissue — whether it is a tooth extraction, a gum surgery, or certain respiratory or cardiac catheterization procedures — bacteria can enter the bloodstream in what is called a transient bacteremia. In most healthy people, the immune system clears these bacteria quickly. But in patients with prosthetic heart valves, a history of previous endocarditis, certain congenital heart defects, or cardiac transplant recipients who develop valve problems, those bacteria can attach to abnormal heart surfaces and multiply. The standard prophylactic regimen for most at-risk adults is a single two-gram dose of amoxicillin taken 30 to 60 minutes before the procedure. For patients allergic to penicillin, alternatives include azithromycin, clindamycin, or cephalexin.
Compared to a full therapeutic course of antibiotics — which might run seven to fourteen days — the prophylactic dose is minimal. The logic is straightforward: flood the bloodstream with enough antibiotic concentration at the exact moment bacteria are most likely to enter, then let the body handle the rest. It is not a prolonged treatment but a precisely timed shield. To put this in perspective, the risk of developing infective endocarditis after a dental procedure in a high-risk patient without prophylaxis is estimated at roughly 1 in 3,000 to 1 in 5,000. Those odds sound low until you consider that endocarditis treatment means four to six weeks of intravenous antibiotics, possible valve replacement surgery, and a significant chance of death. A single pill shifts those odds meaningfully.
Which Heart Conditions Actually Require Prophylactic Antibiotics?
The American Heart Association’s current guidelines — last updated with an advisory in 2021 — restrict prophylaxis to a narrow group of patients at highest risk for adverse outcomes from endocarditis. These include individuals with prosthetic cardiac valves or prosthetic material used in valve repair, patients with a previous episode of infective endocarditis, certain unrepaired cyanotic congenital heart defects, and cardiac transplant patients who develop valve disease. Notably, common conditions like mitral valve prolapse, bicuspid aortic valve, and rheumatic heart disease were removed from the prophylaxis recommendations in 2007. However, the picture is not uniform across the globe. The European Society of Cardiology and the National Institute for Health and Care Excellence in the United Kingdom have taken somewhat different positions.
NICE went as far as recommending against routine antibiotic prophylaxis entirely in 2008, though this was partially walked back after studies showed a modest increase in endocarditis cases following the policy change. If a patient with dementia is receiving care from physicians trained in different guideline traditions, the recommendations they receive may vary. Caregivers should clarify with the treating cardiologist which specific guideline is being followed and why. One important limitation: prophylaxis is recommended only before procedures that involve manipulation of gingival tissue, the periapical region of teeth, or perforation of the oral mucosa. Routine cleanings that do not involve bleeding, simple orthodontic adjustments, and most gastrointestinal or genitourinary procedures no longer carry a prophylaxis recommendation for heart patients. This narrowing surprises many patients and families who remember an era when anyone with a heart murmur took antibiotics before every dental appointment.
The Connection Between Oral Health, Heart Disease, and Cognitive Decline
Research over the past decade has increasingly linked poor oral health to both cardiovascular disease and cognitive decline, creating a triangle of risk that is especially relevant for older adults. The bacterium Porphyromonas gingivalis, a primary driver of periodontal disease, has been found in the brains of Alzheimer’s patients and in atherosclerotic plaques. While causation remains debated, the association is strong enough that maintaining oral health is now considered a modifiable risk factor for both heart disease and dementia. For patients already living with dementia, oral hygiene often deteriorates as the disease progresses.
A person in the moderate stages of Alzheimer’s may resist tooth brushing, forget dental appointments, or be unable to communicate tooth pain. this deterioration means more dental interventions, more opportunities for bacteremia, and a greater need for prophylactic antibiotics if the patient also has a qualifying heart condition. A 2019 study in the Journal of the American Geriatrics Society found that adults with dementia were 23 percent more likely to have untreated dental caries than cognitively intact peers of the same age. The practical implication is that caregivers of dementia patients with cardiac conditions need to be proactive about dental care — not just reactive. Regular cleanings and early treatment of cavities reduce the likelihood of needing more invasive procedures later, which in turn reduces the frequency of antibiotic prophylaxis and its associated risks.
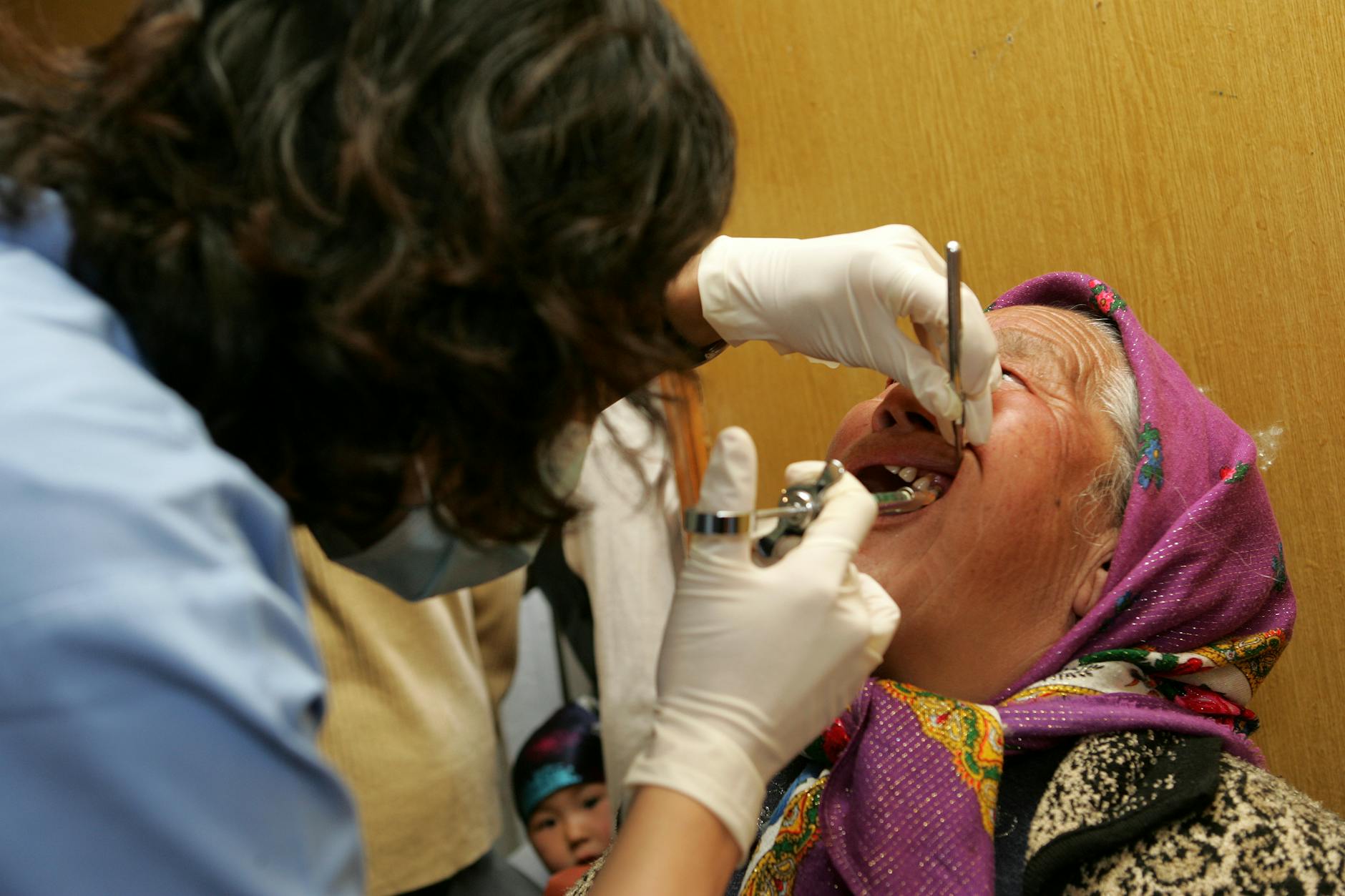
How Caregivers Can Manage Antibiotic Prophylaxis for Patients With Dementia
Managing prophylactic antibiotics requires coordination between the cardiologist, the dentist, and whichever family member or professional caregiver is managing the patient’s medications. The key practical challenge is timing: the antibiotic must be taken 30 to 60 minutes before the procedure, which means someone needs to remember, administer, and confirm the dose. For a patient living with dementia who may not understand why they are being given a pill before leaving for the dentist, this can become a point of resistance or confusion. One approach that works well is to keep a dedicated medical alert card or digital note that lists the patient’s cardiac condition and prophylaxis requirements. This card should travel with the patient to every medical and dental appointment.
Some caregivers also set a phone alarm for 90 minutes before the scheduled appointment — giving a 30-minute buffer for the administration window and any delays. The tradeoff between liquid and tablet formulations matters here. Amoxicillin is available as a suspension, which can be easier to administer to patients who have difficulty swallowing pills — a common issue in later-stage dementia. However, the volume required for a two-gram dose of liquid amoxicillin is substantial, roughly 40 milliliters of the 250mg/5mL concentration, and the taste may provoke refusal. Mixing it into a small amount of applesauce or yogurt can help, but caregivers should confirm with the pharmacist that this does not affect absorption.
Risks of Antibiotic Prophylaxis and When It May Do More Harm Than Good
While a single dose of amoxicillin is generally safe, it is not without risks. Allergic reactions, including rare anaphylaxis, are the most serious concern. For a patient with dementia who cannot clearly communicate symptoms like throat tightness, itching, or nausea, a mild allergic reaction could escalate before it is recognized. Caregivers should remain with the patient for at least 30 minutes after the antibiotic dose and know the signs of anaphylaxis. There is also the broader concern of antibiotic resistance. Critics of prophylaxis argue that the widespread use of antibiotics for a statistically uncommon outcome contributes to the growing resistance crisis. A 2022 Lancet review estimated that bacterial antimicrobial resistance was directly responsible for 1.27 million deaths globally in 2019.
Each unnecessary dose of antibiotics — even a single one — adds selection pressure on bacteria. This is precisely why the guidelines have been narrowed: the benefit must clearly outweigh the population-level cost. A less discussed limitation involves Clostridioides difficile infection. Even a single dose of a broad-spectrum antibiotic can disrupt gut flora enough to permit C. difficile overgrowth, particularly in older adults who have been recently hospitalized or are taking proton pump inhibitors. For a dementia patient who may already be nutritionally vulnerable, a bout of C. difficile diarrhea can lead to dehydration, hospitalization, and accelerated cognitive decline. This does not mean prophylaxis should be skipped when indicated, but it does mean the prescribing physician should weigh this risk and ensure the patient is genuinely in a high-risk cardiac category.

What Happens When Prophylaxis Is Missed
Occasionally, a caregiver forgets the pre-procedure dose, or a dental office proceeds before confirming the antibiotic was taken. The AHA guidelines address this: if the antibiotic was not taken before the procedure, it can still be administered up to two hours afterward and retain some protective benefit. Beyond that window, the value diminishes significantly.
If a procedure is completed without any prophylaxis and the patient develops a fever, chills, night sweats, or unexplained fatigue in the days or weeks following, medical attention should be sought promptly. Infective endocarditis can have a delayed presentation — sometimes two to four weeks after the inciting event — and early detection changes the outcome dramatically. For dementia patients, caregivers should watch for behavioral changes, new confusion beyond baseline, or refusal to eat, as these may be the only visible signs of systemic infection.
Evolving Guidelines and What May Change in Coming Years
The field of endocarditis prophylaxis is not settled. Ongoing research, including large observational studies in Scandinavia and randomized trials in the UK, may shift the guidelines again within the next five to ten years. Some researchers are investigating whether targeted antiseptic mouth rinses — such as chlorhexidine used immediately before dental work — could replace antibiotic prophylaxis for some patient groups, eliminating the resistance concern entirely.
There is also growing interest in individualized risk scoring that accounts for factors beyond the valve condition alone — including age, frailty, immune status, and oral health baseline. For dementia patients, who often carry multiple comorbidities and have limited ability to participate in their own care decisions, a more personalized approach could reduce both overtreatment and undertreatment. Until then, the existing guidelines remain the standard, and the single pre-procedure antibiotic dose remains a small intervention with outsized protective value for the right patients.
Conclusion
Prophylactic antibiotics before cardiac procedures exist because infective endocarditis, though uncommon, is devastating when it occurs. The current guidelines appropriately limit this practice to the highest-risk patients — those with prosthetic valves, prior endocarditis, certain congenital defects, and transplant-related valve disease. For patients with dementia, the intersection of declining oral health, communication difficulties, and complex medication management makes this seemingly simple protocol a genuine caregiving challenge that requires planning and coordination.
The most important steps for caregivers are knowing whether their loved one qualifies for prophylaxis, maintaining that information in an accessible format for every healthcare provider, ensuring the timing of the dose is correct, and watching for signs of infection afterward. Oral health maintenance — daily brushing assistance, regular dental visits, and early intervention for decay — remains the best long-term strategy to reduce the need for invasive procedures in the first place. Talk to the patient’s cardiologist and dentist together if there is any uncertainty about whether prophylaxis is indicated.
Frequently Asked Questions
Does my parent with dementia need antibiotics before every dental cleaning?
Not necessarily. Prophylaxis is only recommended for patients with specific high-risk cardiac conditions, and only before procedures that involve gum manipulation or bleeding. A routine cleaning without significant gum work may not require it. Confirm with the cardiologist.
What if the patient spits out the antibiotic or vomits shortly after taking it?
If vomiting occurs within 30 minutes of the dose, the antibiotic likely was not absorbed and the dose should be repeated. If the patient consistently refuses oral medication, ask the dentist about intramuscular or intravenous antibiotic options that can be administered at the appointment.
Can antibiotic prophylaxis interact with dementia medications like donepezil or memantine?
Amoxicillin has no significant drug interactions with standard dementia medications including donepezil, rivastigmine, galantamine, or memantine. However, clindamycin and azithromycin can interact with other medications common in older adults, so a pharmacist review of the full medication list is always wise.
Are there alternatives to antibiotics for preventing endocarditis?
Currently, no alternative has enough evidence to replace antibiotic prophylaxis for high-risk patients. Chlorhexidine mouth rinses before procedures are sometimes used as an adjunct but are not considered a substitute. Research is ongoing.
How do I know if my family member’s heart condition qualifies for prophylaxis?
The qualifying conditions are specific: prosthetic heart valves, prior infective endocarditis, certain unrepaired congenital heart defects, and cardiac transplant with valve dysfunction. Common conditions like mitral valve prolapse or aortic stenosis do not qualify under current AHA guidelines. Ask the cardiologist directly.