When you stop taking acid blockers — specifically proton pump inhibitors like omeprazole, pantoprazole, or esomeprazole — your stomach fights back by producing more acid than it did before you ever started the medication. This phenomenon, called rebound acid hypersecretion, can leave you with heartburn, nausea, and reflux symptoms that are actually worse than what drove you to take the drug in the first place. It happens because your body adapted to the suppressed acid environment by ramping up its acid-producing machinery, and once the drug is removed, that machinery runs unchecked for weeks or even months. This rebound effect is not rare or theoretical.
In a study of healthy volunteers who had never had acid problems before, 44 percent developed new acid-related symptoms like heartburn and regurgitation after stopping PPI therapy, compared to just 15 percent in a placebo group. That means the drug itself created a problem that did not previously exist. For the millions of Americans who have been on these medications far longer than recommended, the withdrawal period can be genuinely miserable — and it often tricks people into thinking they still need the drug. This article breaks down the science behind rebound acid hypersecretion, what symptoms to expect and how long they last, the risks of staying on PPIs indefinitely, and a step-by-step approach to tapering off safely. If you or someone you care for has been taking acid blockers for months or years, understanding this process is the first step toward getting free of the cycle.
Table of Contents
- Why Does Your Stomach Overproduce Acid After Stopping Acid Blockers?
- What Symptoms Should You Expect During PPI Withdrawal?
- How Many Americans Are Taking PPIs Beyond Safe Limits?
- How to Safely Taper Off Acid Blockers Without Triggering Rebound
- Long-Term Risks of Staying on PPIs Indefinitely
- What Caregivers Should Watch for During a PPI Taper
- Rethinking Acid Blockers as a Long-Term Strategy
- Conclusion
- Frequently Asked Questions
Why Does Your Stomach Overproduce Acid After Stopping Acid Blockers?
The mechanism is straightforward but poorly understood by most patients and, frankly, by many prescribers. PPIs work by shutting down the proton pumps in your stomach lining that produce hydrochloric acid. When acid levels drop, your body interprets this as a deficit and responds by releasing more of a hormone called gastrin. Elevated gastrin over weeks and months causes the enterochromaffin-like cells in your stomach wall to physically grow larger and multiply — a process called ECL cell hypertrophy. These enlarged cells are primed to produce acid at a much higher rate than normal. The moment you remove the PPI, those cells flood your stomach with acid, often exceeding your pre-medication baseline. Daily PPI use for as little as four weeks is enough to trigger this rebound response, which typically begins around 15 days after discontinuation.
For people who have been on PPIs for a year or more, rebound symptoms can persist for 8 to 26 weeks — roughly two to six months. Research suggests it takes approximately three months for acid secretion to return to the levels your stomach maintained before you ever took the drug. During that window, the excess acid can cause genuine tissue irritation, not just discomfort. To put this in perspective, consider someone who started taking omeprazole for occasional heartburn after heavy meals. After a year on the drug, they try to quit cold turkey. Within two weeks, they experience daily burning pain, bloating, and acid washing into their throat — symptoms far more severe than the occasional post-dinner heartburn that started the whole thing. Their doctor may even tell them this proves they need the medication, when in reality, their body is simply going through withdrawal.
What Symptoms Should You Expect During PPI Withdrawal?
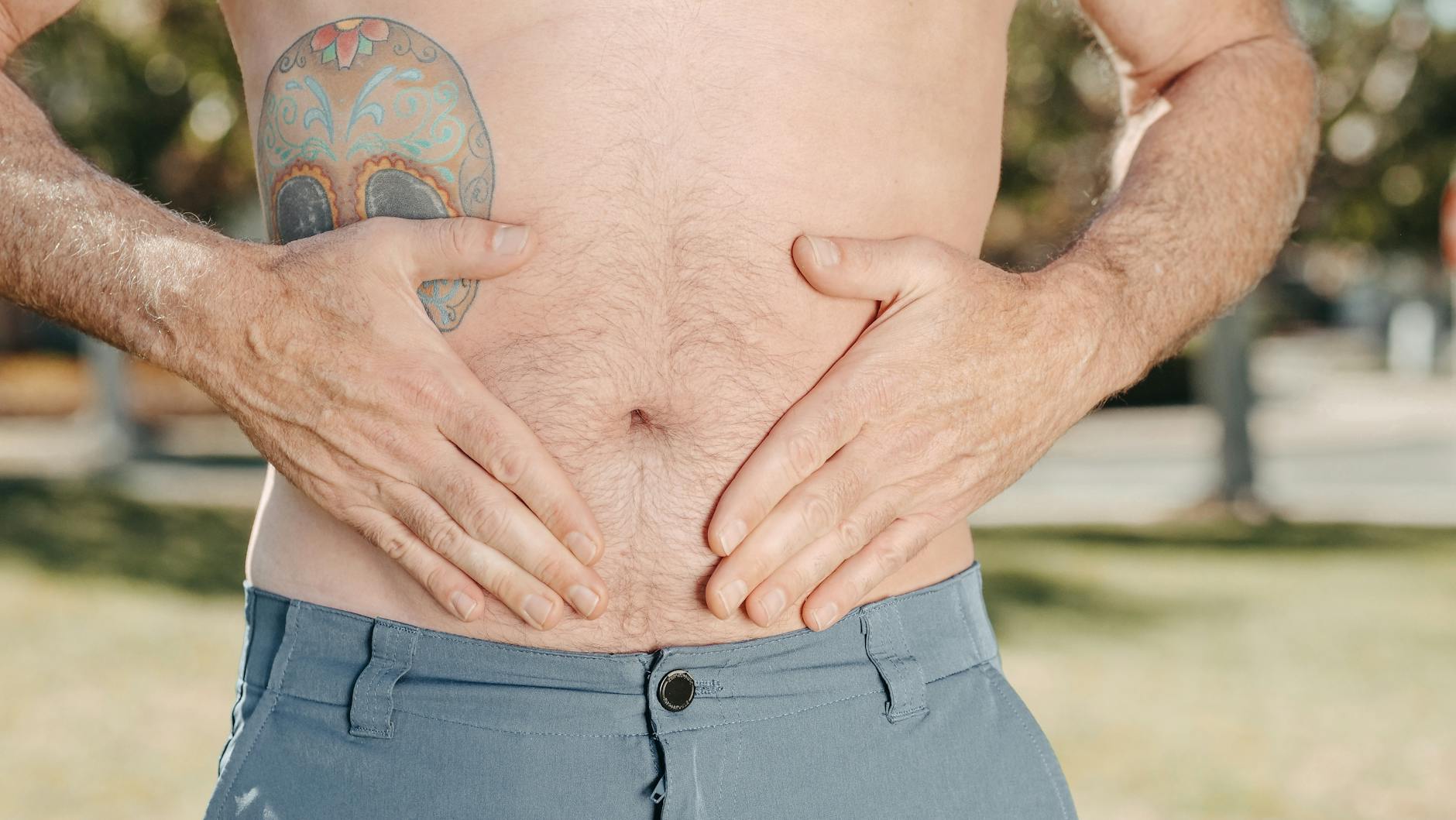
The most common rebound symptoms include worsened heartburn, acid reflux that may reach the throat, stomach pain, bloating, nausea, and general indigestion. Many people describe the experience as feeling like their original condition has returned with a vengeance. The intensity varies from person to person, but it is important to understand that these symptoms are usually temporary and driven by the rebound mechanism rather than by an underlying disease getting worse. However, if you have a diagnosed condition like Barrett’s esophagus, severe erosive esophagitis, or a history of gastrointestinal bleeding, stopping PPIs without medical supervision is not advisable. For these patients, the rebound acid surge could cause real tissue damage, not just discomfort. The distinction matters: someone who was put on a PPI for mild, occasional reflux faces a very different risk profile than someone with documented esophageal erosion.
If you are unsure which category you fall into, this is a conversation to have with a gastroenterologist before making changes. The psychological dimension of withdrawal deserves attention as well. The VA Whole Health Library specifically warns that rebound symptoms create a cycle of PPI dependence. Patients restart the medication thinking their condition requires it, when the symptoms are actually caused by withdrawal. This cycle can keep people on PPIs for years or even decades beyond what was ever intended. Recognizing that the discomfort is temporary and expected — not a sign that something is wrong — is half the battle.
How Many Americans Are Taking PPIs Beyond Safe Limits?
The scale of long-term PPI use in the United States is staggering. Approximately 15 million Americans take proton pump inhibitors daily, and roughly 7 million of those are using over-the-counter PPIs longer than the FDA-recommended limit. The FDA’s guidance is clear: OTC PPIs should be limited to 14-day courses, repeated no more than three times per year. That is a maximum of 42 days per year. Yet millions of people take them every single day, year after year, often without any ongoing medical oversight. Since 2010, the FDA has issued seven separate safety warnings about PPIs, addressing bone fractures of the hip, wrist, and spine; dangerously low magnesium levels; Clostridium difficile infections; vitamin B12 deficiency; acute interstitial nephritis; and lupus-like autoimmune events.
Each warning added to a growing body of evidence that these drugs, while effective for short-term acid suppression, carry meaningful risks when used chronically. For a dementia care audience, the nutrient depletion angle is particularly relevant — B12 deficiency and magnesium depletion are both associated with cognitive symptoms, and older adults are already at higher risk for these deficiencies. A practical example: a 72-year-old woman on omeprazole for three years begins showing signs of confusion and fatigue. Her family assumes it is early dementia. Lab work eventually reveals critically low B12 and magnesium — both linked to her long-term PPI use. Once the deficiencies are corrected and the PPI is tapered, her cognitive symptoms improve. this is not a rare scenario, and it illustrates why anyone involved in caring for older adults should understand what these medications do over time.

How to Safely Taper Off Acid Blockers Without Triggering Rebound
The most important practical takeaway is this: do not stop PPIs abruptly. A gradual taper over two to four weeks significantly reduces or may even prevent rebound acid hypersecretion entirely. One study using the alkaline tide method in patients with dyspepsia and reflux found that gradual cessation could prevent rebound altogether. The typical taper schedule looks like this: if you are taking the PPI twice daily, drop to once daily for one to two weeks, then to every other day for another one to two weeks, then stop. Some clinicians recommend switching to an H2 blocker like famotidine during the taper period. H2 blockers suppress acid through a different mechanism and are generally considered safer for short-term use.
They provide enough acid control to ease the transition without perpetuating the rebound cycle. Yale Medicine notes that this step-down approach — PPI to H2 blocker to nothing — can make the process considerably more tolerable. The tradeoff is that famotidine is less potent than a PPI, so patients may still experience some breakthrough symptoms, but these are usually mild and manageable. The comparison between cold-turkey cessation and a structured taper is stark. Stopping abruptly after long-term use almost guarantees weeks of miserable rebound symptoms and a high likelihood of restarting the drug. Tapering with medical guidance offers a realistic path off the medication with manageable discomfort. For caregivers managing an older adult’s medication regimen, coordinating this taper with the prescribing physician and the broader care team is essential — the last thing you want is a frail patient dealing with severe reflux symptoms on top of other health challenges.
Long-Term Risks of Staying on PPIs Indefinitely
For people who decide the rebound period sounds too difficult and choose to stay on their PPI, the risks accumulate. Long-term use is associated with increased bone fracture risk, particularly of the hip, wrist, and spine — a serious concern for older adults already prone to falls. Chronic PPI use also raises the risk of Clostridium difficile infections and pneumonia, both of which can be life-threatening in elderly or immunocompromised patients. Progressive chronic kidney disease has been linked to prolonged PPI therapy, and disruption of the gut microbiome is now well documented. The nutrient depletion issue deserves special emphasis for anyone in the dementia care space. Vitamin B12, iron, and magnesium all require adequate stomach acid for proper absorption. Suppress that acid for years, and deficiencies develop silently.
Low B12 can mimic or worsen dementia symptoms. Low magnesium affects muscle function, heart rhythm, and cognition. Low iron leads to anemia and fatigue. These are not theoretical risks — they are predictable consequences of long-term acid suppression, and they are frequently overlooked in older patients whose symptoms get attributed to aging rather than medication side effects. A limitation worth noting: not everyone on a long-term PPI is taking it inappropriately. Some conditions — Zollinger-Ellison syndrome, severe Barrett’s esophagus, certain post-surgical states — genuinely require ongoing acid suppression. The concern is with the vast majority of long-term users who were started on a PPI for mild reflux, never had their prescription reassessed, and have been refilling it on autopilot for years.
What Caregivers Should Watch for During a PPI Taper
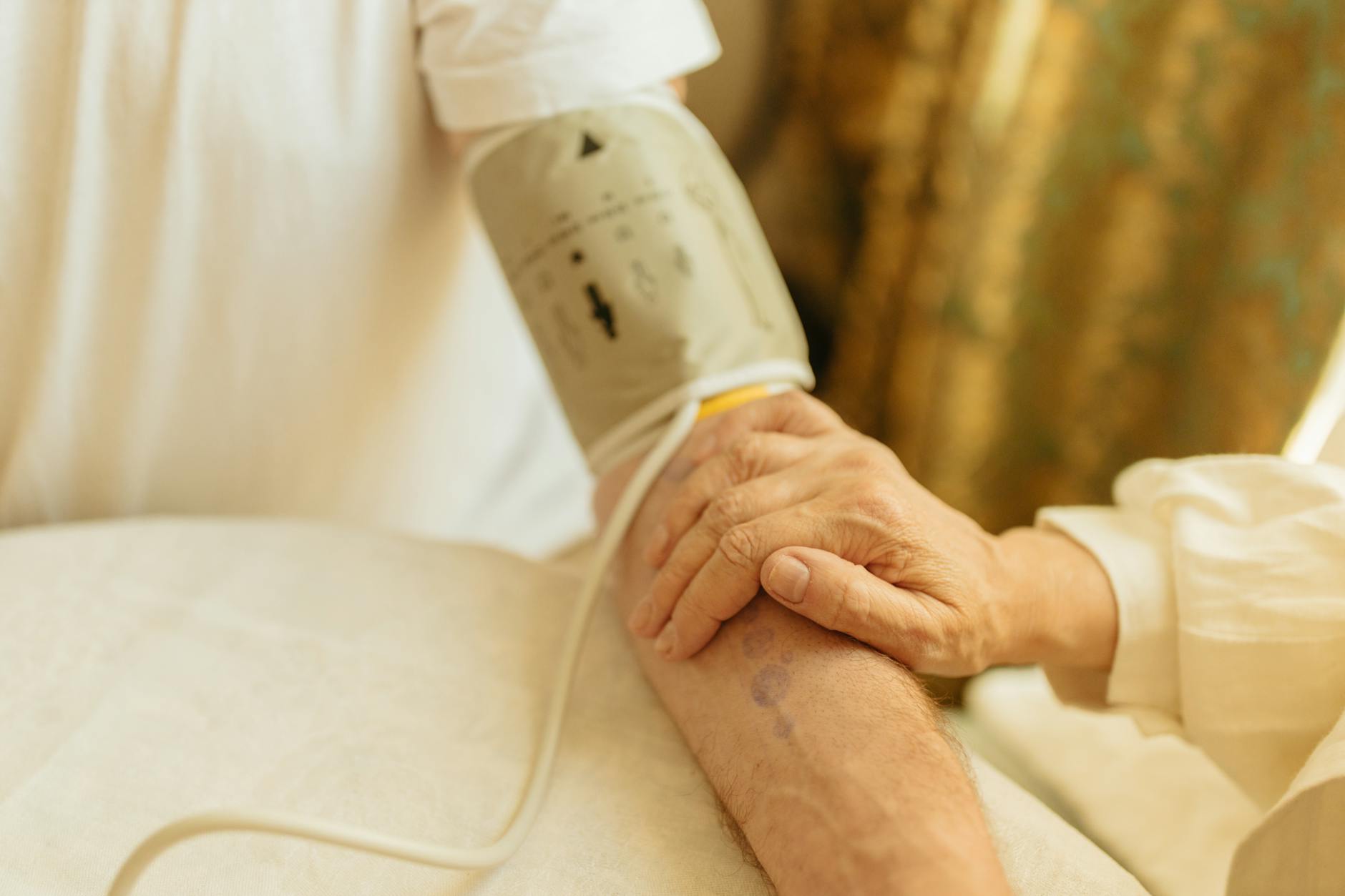
If you are managing medications for someone with dementia or cognitive impairment, a PPI taper requires extra vigilance. The person may not be able to articulate that they are experiencing increased heartburn or stomach pain. Watch for behavioral changes — increased agitation, refusal to eat, disrupted sleep, or grimacing during or after meals. These can all signal acid-related discomfort.
Keep a simple log of symptoms and share it with the prescribing doctor at each check-in. It is also worth reviewing the full medication list with a pharmacist. PPIs interact with several common drugs, including clopidogrel (Plavix), certain antifungals, and some anti-seizure medications. Removing or reducing a PPI may change how other drugs are absorbed, which could require dosage adjustments elsewhere.
Rethinking Acid Blockers as a Long-Term Strategy
The medical community is slowly shifting its stance on long-term PPI use. More gastroenterologists now advocate for periodic reassessment — asking whether the patient still needs the drug rather than automatically renewing it. Guidelines increasingly emphasize using the lowest effective dose for the shortest possible duration.
For many patients, lifestyle modifications like elevating the head of the bed, avoiding late-night eating, and identifying trigger foods can manage mild reflux without any medication at all. Looking ahead, better patient education about rebound acid hypersecretion could break the cycle of unnecessary long-term use. If people understood before starting a PPI that stopping it would temporarily worsen their symptoms, they might make different choices about starting one in the first place — or at minimum, they would be prepared for what comes next and less likely to interpret withdrawal as proof that they need the drug forever.
Conclusion
Stopping acid blockers after weeks or months of use triggers a well-documented rebound effect in which your stomach produces significantly more acid than it did before you started the medication. This rebound can last two to six months and creates symptoms that are often worse than the original problem, trapping millions of people in a cycle of unnecessary long-term use. The FDA has issued seven safety warnings about PPIs since 2010, and roughly 7 million Americans are using OTC versions beyond recommended limits.
The path forward is a gradual taper over two to four weeks, ideally under medical supervision, with the possible addition of a milder H2 blocker like famotidine during the transition. For caregivers of older adults, especially those with cognitive impairment, understanding this process is critical — both because the taper requires careful monitoring and because the long-term nutrient depletion caused by PPIs can directly affect brain health. Talk to a gastroenterologist, make a plan, and expect some temporary discomfort on the way to a stomach that regulates itself again.
Frequently Asked Questions
How long does rebound acid last after stopping a PPI?
For most people, rebound acid hypersecretion begins about 15 days after stopping the medication and can last 8 to 26 weeks, depending on how long you were on the PPI. Acid secretion generally returns to pre-drug baseline levels within about three months.
Can rebound acid hypersecretion happen even if I never had acid problems before?
Yes. A study of healthy volunteers with no prior acid issues found that 44 percent developed new acid-related symptoms after stopping PPI therapy, compared to 15 percent in a placebo group. The drug itself can create the problem.
Is it safe to stop a PPI cold turkey?
It is not recommended, especially after more than four weeks of daily use. Abrupt cessation is far more likely to cause severe rebound symptoms. A gradual taper over two to four weeks — reducing from twice daily to once daily to every other day — is the safer approach.
Should I switch to an H2 blocker like famotidine when tapering off a PPI?
Many gastroenterologists recommend this. H2 blockers provide milder acid suppression through a different mechanism and can ease the transition. They are generally considered safer for short-term use and do not carry the same rebound risk as PPIs.
Can long-term PPI use affect brain health?
Indirectly, yes. Long-term PPIs impair absorption of vitamin B12 and magnesium, both of which are important for cognitive function. B12 deficiency in particular can mimic or worsen dementia symptoms, making this a significant concern for older adults and their caregivers.
How long does the FDA say you should take OTC PPIs?
The FDA recommends OTC PPIs be limited to 14-day courses, no more than three times per year. That is a maximum of 42 days annually — far less than the continuous daily use that millions of Americans maintain.





