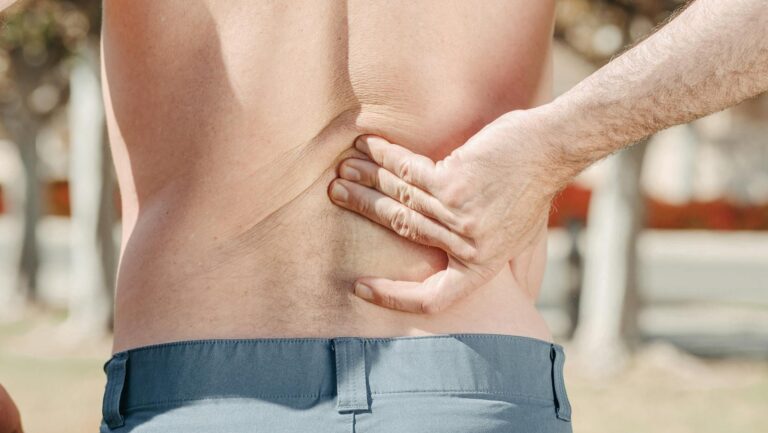
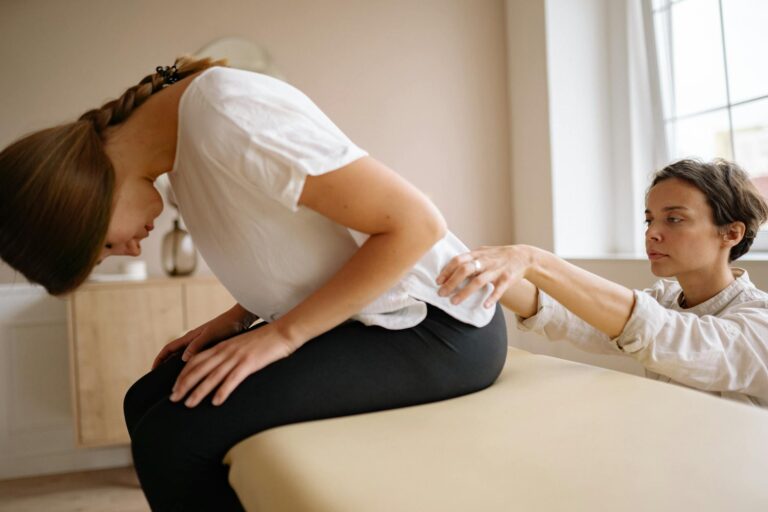
If you’re experiencing lower back pain that lingers for weeks or doesn’t respond to rest, disc-related issues could be the culprit. Disc herniation and bulging discs are common causes of persistent back pain, affecting 1-3% of the population annually, with peak occurrence between ages 30-50. The key to distinguishing disc-related pain from simple muscle strain is recognizing specific warning signs—particularly pain that radiates down your leg, numbness in your feet, or weakness that makes everyday tasks difficult. These symptoms indicate that a herniated or bulging disc is pressing on a nerve, and they deserve medical attention.
This article will walk you through the eight primary warning signs that your back pain may be disc-related, explain why each matters, and help you understand when to seek professional evaluation. Most people assume lower back pain will resolve on its own, but disc-related issues follow a different pattern. Unlike a pulled muscle that typically improves within days, pressure from a herniated disc tends to persist or worsen over time if left untreated. Understanding the distinction can help you avoid months of unnecessary suffering and identify when you need a doctor’s evaluation.
Table of Contents
- What Does Localized Lower Back Pain Tell You About Your Discs?
- Radiating Leg Pain—The Most Telltale Sign of Nerve Compression?
- Numbness and Tingling—When Nerve Compression Becomes Serious?
- Muscle Weakness—When Your Body Signals Nerve Damage?
- Movement-Triggered Pain—Why Certain Motions Intensify Everything?
- Persistent Symptoms Lasting Weeks or Months—When It’s Definitely Not Just a Strain?
- Stiffness and Reduced Flexibility—Why Your Range of Motion Shrinks?
- Emergency Warning Signs—Loss of Bowel or Bladder Control?
- Conclusion
What Does Localized Lower Back Pain Tell You About Your Discs?
The most obvious sign of a herniated disc affecting the lower spine is localized lower back pain concentrated in the lumbar region. This pain typically originates at the site of the disc herniation and may feel like a dull ache, sharp stabbing sensation, or muscle soreness. What distinguishes disc-related pain is its persistence—it doesn’t resolve within a few days of rest the way a strained muscle typically does. Localized lower back pain alone, however, doesn’t automatically mean you have a disc problem. Many conditions cause localized back pain, including muscle strains, ligament injuries, or facet joint inflammation.
For example, a person who lifted something awkwardly at the gym might experience identical localized pain from muscle strain, which usually resolves within a week. The difference emerges when you add other symptoms—particularly if that localized pain is accompanied by numbness, weakness, or radiating leg pain. When localized pain persists beyond two weeks without improvement, especially if it worsens with certain movements, disc involvement becomes more likely. The lower back bears most of your body’s weight and supports movement in multiple directions, making it vulnerable to disc problems. The L4-L5 and L5-S1 levels are the most frequent locations for lumbar disc herniation, simply because these lower vertebrae absorb the most mechanical stress.

Radiating Leg Pain—The Most Telltale Sign of Nerve Compression?
Radiating leg pain is one of the clearest indicators that a disc is compressing a nerve rather than causing simple inflammation. This pain travels from your lower back through your buttocks and down one or both legs, with intensity typically greatest in the buttocks, thigh, and calf areas. Patients often describe this sensation as sharp, burning, or throbbing, and it frequently follows a specific path—the pattern of pain distribution often corresponds to which nerve root the disc is pinching. However, not all radiating leg pain originates from the spine.
Piriformis syndrome, where a hip muscle compresses the sciatic nerve, can produce nearly identical symptoms. The key distinction is that disc-related pain usually follows a specific dermatomal pattern (matching nerve pathways), while muscular causes tend to produce more diffuse pain. Additionally, disc-related pain typically worsens with certain spinal movements—bending forward, twisting, or straining—whereas muscle-related pain might not show this clear movement pattern. If your leg pain is accompanied by numbness or tingling, this strengthens the likelihood of disc involvement, because the radiating pain then represents actual nerve compression rather than just inflammation. Conversely, if leg pain occurs only during specific activities and resolves completely with rest, muscle-related causes become more probable.
Numbness and Tingling—When Nerve Compression Becomes Serious?
Numbness and tingling sensations—often described as “pins and needles” or a burning feeling—indicate active nerve compression from a herniated disc. Unlike pain, which signals inflammation, numbness and tingling suggest the nerve itself is being pressured or irritated. These sensations typically appear in your legs and feet, following the specific nerve pathway affected by the disc herniation. The significance of numbness and tingling lies in what they reveal about urgency. While painful symptoms might resolve on their own, progressive numbness indicates worsening nerve compression that requires evaluation.
For instance, numbness that starts in your foot and gradually spreads up your leg suggests the herniation is enlarging or the nerve compression is intensifying. This progression is exactly when intervention becomes important—because prolonged nerve compression can eventually cause permanent damage if left untreated. One important limitation: mild, intermittent tingling doesn’t necessarily mean serious disc involvement. Lying in certain positions, poor circulation, or even anxiety can cause temporary tingling. However, when numbness and tingling are persistent, progressive, or accompanied by other warning signs like weakness or radiating pain, professional evaluation becomes necessary. Many people wait too long before seeking help because they underestimate what these sensations mean.

Muscle Weakness—When Your Body Signals Nerve Damage?
Weakness in the legs or feet is a particularly significant warning sign because it indicates the herniated disc isn’t just causing pain or sensory symptoms—it’s actually affecting nerve function. This weakness might manifest as difficulty lifting your foot when climbing stairs, trouble pointing your toes, weakness when attempting to lift or carry objects, or a feeling that your legs might “give way.” The specific muscles affected depend on which nerve root is compressed. This symptom demands more attention than pain alone. While pain typically improves with conservative treatment like physical therapy and rest, weakness that develops from nerve compression may not fully recover if the compression persists too long.
Consider the contrast: a patient with severe pain but no weakness might improve substantially with conservative care and time, while a patient with mild pain but progressive weakness might require earlier intervention to prevent permanent nerve damage. This distinction influences treatment decisions—some cases that might otherwise be managed conservatively need to be re-evaluated if weakness appears or worsens. If you notice new weakness, this is the point to contact your doctor rather than waiting for self-resolution. Weakness that appears suddenly or progresses over days to weeks warrants faster evaluation than pain that appears gradually.
Movement-Triggered Pain—Why Certain Motions Intensify Everything?
Disc-related lower back pain has a distinctive pattern: it intensifies when you bend forward, twist, cough, or sneeze. This happens because these movements change pressure within the disc itself and the space around compressed nerves. Forward bending, in particular, typically worsens disc-related pain because it shifts pressure toward the back of the disc—directly toward where the herniation often occurs. In contrast, standing and backward bending sometimes provide relief because they shift pressure away from the nerve. The movement-triggered pattern serves as a useful diagnostic clue, but it’s not foolproof.
Muscle strains also worsen with certain movements. The critical distinction is the pattern: disc-related pain usually worsens with forward bending and twisting but improves with backward bending, while muscle strains often improve with rest regardless of position. Additionally, pain triggered by coughing or sneezing is particularly suggestive of disc involvement, because these movements create sudden pressure changes throughout your spine. This characteristic also explains why people with disc problems often find that staying in certain positions—frequently lying down or backward bending—provides comfort, while common activities become surprisingly difficult. Someone might manage to sit through a movie but struggle to walk across a parking lot, or might find relief lying flat but extreme difficulty bending to pick something off the floor.

Persistent Symptoms Lasting Weeks or Months—When It’s Definitely Not Just a Strain?
If your lower back pain has persisted for more than two weeks without significant improvement, disc involvement becomes increasingly likely. Most muscle strains and minor soft tissue injuries improve within 5-10 days with rest and basic care. Pain that persists beyond this window, especially pain accompanied by any of the other warning signs mentioned here, indicates something more significant is happening—typically a disc pressing on a nerve that requires specific treatment to resolve. The duration itself carries diagnostic significance.
Research shows that symptoms persisting multiple weeks are much more likely to be disc-related than acute muscle injuries. Statistics on lumbar disc herniation show that roughly 40% of the population experiences lumbar disc herniation at some point in their lifetime, most commonly between ages 30-50, and those cases rarely resolve quickly without intervention. Persistent symptoms also affect treatment approach. While short-term pain might respond to over-the-counter medications and rest, longer-lasting symptoms typically require physical therapy targeting the specific movement patterns that cause problems with your herniated disc, possibly combined with anti-inflammatory medications or imaging to confirm the diagnosis.
Stiffness and Reduced Flexibility—Why Your Range of Motion Shrinks?
Stiffness and loss of flexibility, particularly noticeable after rest or prolonged sitting, represent another characteristic sign of disc problems. This stiffness differs from muscle soreness—it’s a feeling of rigidity that makes movement difficult to initiate, especially first thing in the morning or after sitting for extended periods. Your lower back may feel locked or resistant to bending, and simple movements like rolling over in bed or standing up from a chair become surprisingly challenging.
This stiffness exists because inflammation surrounding the herniated disc and the protective muscle spasming response both restrict movement. Additionally, you naturally avoid positions that cause pain, which further limits your range of motion—and limited motion creates additional stiffness in a feedback loop. Over time, this can lead to progressively worsening flexibility and strength if the underlying disc problem isn’t addressed.
Emergency Warning Signs—Loss of Bowel or Bladder Control?
While most disc-related symptoms are painful but not dangerous, one presentation represents a medical emergency: sudden loss of bowel or bladder control, particularly when accompanied by lower back pain and leg symptoms. This combination indicates cauda equina syndrome, a condition where a massive disc herniation compresses the nerve bundle at the base of your spine that controls these functions.
Cauda equina syndrome demands immediate emergency evaluation—delaying care by even hours can result in permanent paralysis or loss of bowel and bladder control. Contact emergency services immediately if you experience saddle anesthesia (numbness in the area that would contact a saddle if you were riding), loss of bowel or bladder control, or progressive bilateral leg weakness. These are the rare but serious presentations of disc disease, and they’re the only disc-related symptoms that constitute a true medical emergency.
Conclusion
Disc-related lower back pain presents a distinctive constellation of warning signs that differ from simple muscle strains or other back issues. The presence of radiating leg pain, numbness, tingling, weakness, or pain that persists for weeks despite rest suggests your doctor should evaluate your spine. Early evaluation can prevent unnecessary suffering and help determine whether conservative treatment like physical therapy will resolve your symptoms or whether additional intervention is needed.
If you’re experiencing any of these eight warning signs, particularly if multiple symptoms are present together, schedule an appointment with your primary care doctor or a spine specialist. They can order appropriate imaging, confirm whether disc involvement is occurring, and recommend the most effective treatment path. Remember: 90% of patients who undergo surgical treatment for symptomatic disc herniation report significant pain improvement within six months, and many cases resolve well with conservative care—but neither option works well if the problem isn’t accurately identified and addressed.