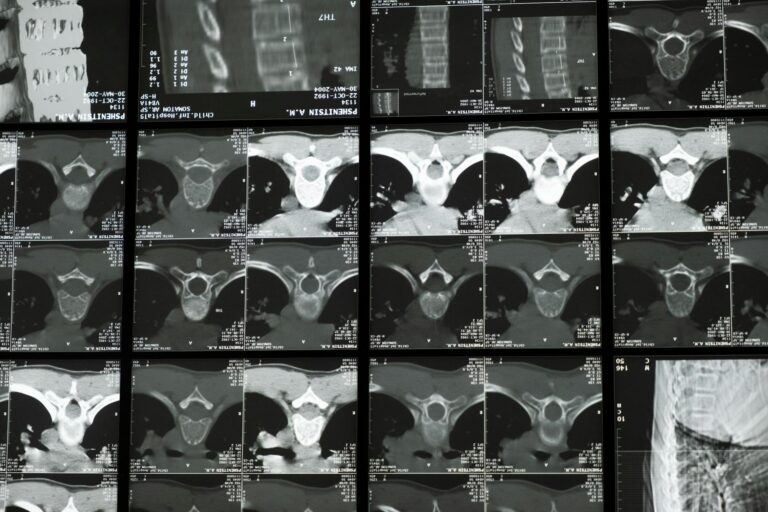
Spine degeneration is driven by eight primary causes, and the most important thing to understand is that nearly all of them interact with each other. Aging tops the list, followed by disc dehydration, genetics, injuries, obesity, smoking, repetitive occupational stress, and a sedentary lifestyle. By age 50, roughly 80 percent of people already show signs of disc degeneration on imaging, and by age 80, that figure climbs to 96 percent, according to data from Vanderbilt Health and the Cleveland Clinic. If you are over 40, the odds are strong that some degree of degeneration is already underway in your spine — whether or not you feel it. What makes this topic especially relevant for brain health and dementia care is the cascade of consequences that follow.
Chronic pain from spinal degeneration limits mobility, disrupts sleep, and contributes to social isolation — all recognized risk factors for cognitive decline. A person caring for a loved one with dementia may also be managing their own back pain, and understanding why the spine breaks down can inform better decisions about movement, posture, and long-term physical resilience. An estimated 266 million people worldwide are affected by degenerative spine conditions each year, making this one of the most common musculoskeletal problems on the planet. This article breaks down each of the eight causes in detail, examines how they overlap, and offers practical context for people navigating aging, caregiving, or both. We will look at who is most affected, which risk factors you can actually control, and where the science stands on slowing the process down.
Table of Contents
- What Are the Leading Causes of Spine Degeneration and Why Does It Start So Early?
- How Genetics and Family History Shape Your Risk for Disc Degeneration
- How Injuries and Trauma Can Trigger a Degenerative Cascade
- Obesity, Smoking, and the Modifiable Risks You Can Actually Address
- How Repetitive Stress and Sedentary Living Wear Down the Spine
- Gender Differences in Spine Degeneration
- What the Future Holds for Treating and Slowing Spine Degeneration
- Conclusion
- Frequently Asked Questions
What Are the Leading Causes of Spine Degeneration and Why Does It Start So Early?
The short answer is that your spine starts aging before you do. Research shows that 37 percent of people already have detectable disc degeneration on MRI by age 20 — long before most would associate themselves with “back problems.” The spine’s intervertebral discs, which serve as shock absorbers between vertebrae, begin losing water content from early adulthood. At birth, those discs are roughly 80 percent water. Over the decades, they gradually desiccate, becoming thinner, less flexible, and more prone to tearing. This disc dehydration is the primary physical mechanism behind degeneration, according to the Cleveland Clinic and WebMD. Aging and dehydration work together in a way that is essentially unavoidable. Think of a kitchen sponge left out on the counter for months — it stiffens, cracks, and cannot absorb anything the way it once could.
Your discs undergo a similar transformation, albeit over years rather than weeks. One-third of adults aged 40 to 59 already have moderate to severe degenerative disc disease, according to research highlighted by ScienceDaily. The important caveat here is that degeneration on imaging does not always mean pain. Many people walk around with significantly worn discs and feel nothing, while others experience debilitating symptoms from relatively minor changes. The remaining six causes on this list — genetics, injury, obesity, smoking, occupational stress, and inactivity — are best understood as accelerators layered on top of this baseline aging process. Some you can modify. Others you cannot. But knowing what drives the process gives you a better foundation for making decisions, especially when someone in your household is already dealing with mobility limitations from dementia or another chronic condition.

How Genetics and Family History Shape Your Risk for Disc Degeneration
If your parents or grandparents had significant back problems, your own spine may be wired for trouble. Research published in the Journal of Clinical Medicine found that genetic factors play the “main role” in the pathology of diseases associated with disc degeneration — even more than environmental factors. Johns Hopkins Medicine similarly identifies family history as a meaningful risk factor for degenerative disc disease. The implication is humbling: you can do many things right and still be predisposed to faster-than-average spinal wear. However, genetics is not destiny in isolation. What the research actually shows is that genetic predisposition interacts with environmental and lifestyle factors to determine outcomes.
A person with a strong family history of disc disease who also works a physically demanding job, carries excess weight, and smokes is compounding inherited vulnerability with controllable risk. Conversely, someone with the same genetic profile who maintains a healthy weight, stays active, and avoids tobacco may experience far less severe degeneration. The limitation here is that we cannot yet screen for specific “disc degeneration genes” in any routine clinical way, so family history remains the most practical proxy. For caregivers of people with dementia, this genetic overlap matters in a practical sense. The same family that shares a predisposition for Alzheimer’s or vascular dementia may also share spinal vulnerability. If you are a middle-aged adult caring for a parent with both cognitive decline and chronic back pain, paying attention to your own spinal health is not vanity — it is prevention.
How Injuries and Trauma Can Trigger a Degenerative Cascade
A single fall, a rear-end collision, or a sports injury can set off a chain of events in the spine that unfolds over years. According to the Cleveland Clinic and UPMC, spinal trauma causes swelling, soreness, and instability in the affected discs. Even injuries that seem minor at the time — a hard landing while jogging, an awkward twist during yard work — can initiate or accelerate degeneration. The disc does not heal the way a broken bone does. It has very limited blood supply, so once it is damaged, the repair process is slow and often incomplete. Consider someone who slips on ice at age 35 and herniates a lumbar disc. The acute pain may resolve within weeks or months, but the structural damage remains.
That disc is now thinner, less hydrated, and more vulnerable to further injury. Ten or fifteen years later, the same person may develop chronic low back pain and be told they have degenerative disc disease — a condition that feels like it appeared from nowhere but actually traces back to that single fall. This is the degenerative cascade in action: an initial insult that compounds over time. For older adults, the injury risk multiplies. People with dementia are significantly more prone to falls due to balance impairment, spatial disorientation, and medication side effects. Each fall carries the potential to accelerate existing spinal degeneration or create new damage. This is one reason why fall prevention programs are so heavily emphasized in dementia care — the consequences extend far beyond bruises and fractures.

Obesity, Smoking, and the Modifiable Risks You Can Actually Address
Among the eight causes of spine degeneration, obesity and smoking stand out because they are modifiable — difficult to change, certainly, but within the realm of personal and medical intervention. A large Medicare study published in Nature’s Scientific Reports in 2021 found that diagnosed obesity is a significant factor in the prevalence of spinal degenerative disease, with overall diagnosed prevalence at 27.3 percent across the Medicare population and rates increasing with both age and BMI. The mechanical explanation is straightforward: excess body weight puts additional compressive force on discs and vertebrae with every step, every bend, and every hour spent sitting. Smoking, meanwhile, attacks the spine from the inside. According to Cedars-Sinai and the Cleveland Clinic, tobacco use reduces blood flow to spinal discs, effectively starving them of the nutrients and oxygen they need to maintain themselves. It also impairs the body’s ability to heal from disc injuries.
The tradeoff for smokers considering quitting is worth stating plainly: while quitting will not reverse existing degeneration, it can slow the progression and improve the body’s response to any treatment pursued later. The comparison between these two risk factors is instructive. Losing weight produces relatively quick mechanical relief for the spine — every pound lost reduces compressive force on lumbar discs. Quitting smoking, on the other hand, produces slower but deeper biological improvements in disc nutrition and healing capacity. Neither is easy. Both matter. And for caregivers managing their own health while supporting a family member with dementia, addressing even one of these factors can meaningfully change the trajectory of spinal aging.
How Repetitive Stress and Sedentary Living Wear Down the Spine
Jobs or daily routines involving repetitive bending, heavy lifting, or prolonged sitting put continuous strain on the spine that compounds over months and years. Harvard Health and Mayfield Brain and Spine both identify occupational factors as significant contributors to disc degeneration, with improper lifting techniques being a particularly common accelerator. A warehouse worker lifting boxes all day and an office worker sitting at a desk for ten hours are damaging their spines through different mechanisms but arriving at a similar destination. The sedentary side of the equation is equally concerning and often overlooked. Research from PMC on aging populations and spine care shows that reduced mobility and diminished muscle activity lead to weakened spinal support structures and significant bone density loss. This combination heightens the risk of disc degeneration, vertebral fractures, and spinal stenosis.
The warning here is that inactivity can be as damaging as overuse — a point that is critical for dementia caregivers who may find themselves sitting for long periods during medical appointments, hospital visits, or simply while keeping watch over a loved one. The limitation of addressing occupational stress is that people often cannot change their jobs. A home health aide, for instance, may spend years transferring patients and bending over beds — activities that are inherently hard on the spine. In these cases, body mechanics training and core-strengthening exercise can mitigate but not eliminate the risk. For sedentary individuals, the prescription is simpler in theory: move more, sit less. But for anyone managing the around-the-clock demands of dementia caregiving, carving out time for exercise can feel impossible, which is why even brief daily walks or simple stretching routines carry outsized value.

Gender Differences in Spine Degeneration
The data on gender and spine degeneration reveals a pattern that deserves more attention. Disc degeneration has been found in 71 percent of men and 77 percent of women under age 50, with both sexes exceeding 90 percent prevalence after 50. More striking is the finding that progression of degeneration occurs 40 to 70 percent more frequently in women than in men.
Hormonal changes after menopause, differences in bone density, and variations in spinal biomechanics all appear to contribute. This gender gap is relevant for dementia care planning because women make up the majority of both dementia patients and dementia caregivers. A 60-year-old woman caring for a spouse with Alzheimer’s is statistically more likely to be dealing with her own advancing spinal degeneration — and less likely to have time to address it. Recognizing this disparity can inform more realistic care plans that account for the caregiver’s physical limitations, not just the patient’s.
What the Future Holds for Treating and Slowing Spine Degeneration
The current medical consensus is that spine degeneration cannot be reversed, but it can be slowed and managed. Research into regenerative approaches — including stem cell therapy, growth factor injections, and bioengineered disc replacements — is advancing, though none of these are standard care yet. For now, the most effective strategies remain the fundamentals: maintaining a healthy weight, staying physically active, avoiding tobacco, using proper body mechanics, and seeking early treatment for injuries rather than ignoring them. For the aging population, and particularly for people navigating dementia in their families, the forward-looking message is one of agency within limits. You cannot stop your discs from aging, and you cannot rewrite your genetic code.
But the modifiable causes on this list — obesity, smoking, inactivity, and poor body mechanics — represent real levers that can shape how your spine ages over the next decade. The 266 million people affected by degenerative spine conditions each year are not a monolith. Some will experience minimal symptoms. Others will face chronic pain that reshapes their daily lives. Where you land on that spectrum is not entirely predetermined.
Conclusion
Spine degeneration is driven by a combination of factors that range from the completely uncontrollable — aging, genetics — to the meaningfully modifiable — weight, smoking, activity level, and injury prevention. The statistics are sobering: nearly everyone over 50 shows degeneration on imaging, and progression hits women harder than men. But the presence of degeneration on a scan is not the same as a sentence of chronic pain, and many of the accelerating factors respond to intervention.
If you are managing your own spinal health while caring for someone with dementia, the most practical step is to address what you can without waiting for a crisis. Strengthening your core, maintaining movement throughout the day, managing your weight, and avoiding tobacco are not glamorous interventions, but they are the ones backed by the strongest evidence. Talk to your physician about what is realistic given your caregiving responsibilities, and do not dismiss back pain as an inevitable part of aging that does not warrant attention. Your spine’s future is not fully written yet.
Frequently Asked Questions
Is degenerative disc disease actually a “disease”?
Despite the name, it is not a disease in the traditional sense. It is a condition describing the natural breakdown of spinal discs over time. The term can be misleading because it implies something was “caught” or could be “cured,” when in reality it describes a nearly universal aging process.
At what age does spine degeneration typically begin?
Earlier than most people expect. Imaging studies show that 37 percent of people have detectable disc degeneration by age 20, according to Vanderbilt Health data. By 50, roughly 80 percent show signs, and by 80, the figure reaches 96 percent.
Can exercise make spine degeneration worse?
It depends on the type of exercise. High-impact activities or heavy lifting with poor form can accelerate disc wear. However, regular moderate exercise — walking, swimming, core strengthening — generally supports spinal health by maintaining muscle support and disc nutrition. Inactivity is typically more harmful than appropriate exercise.
Does spine degeneration cause dementia or cognitive decline?
Spine degeneration does not directly cause dementia. However, the chronic pain, reduced mobility, sleep disruption, and social isolation that often accompany severe spinal degeneration are all independently associated with increased risk of cognitive decline.
Is surgery necessary for degenerative disc disease?
In most cases, no. The majority of people with degenerative disc disease are managed with conservative treatment — physical therapy, weight management, pain management, and activity modification. Surgery is generally reserved for cases with severe nerve compression or instability that does not respond to other approaches.
Are women more affected by spine degeneration than men?
The data suggests yes. While both sexes show high rates of degeneration after 50, progression occurs 40 to 70 percent more frequently in women than in men, likely influenced by hormonal changes, bone density differences, and biomechanical factors.