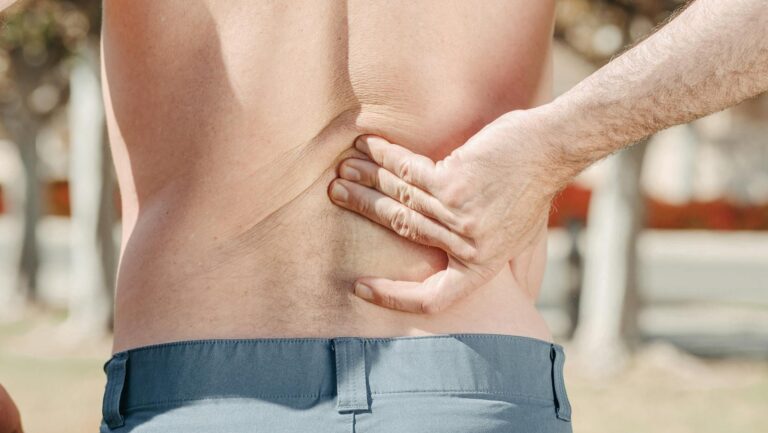
Lumbar disc bulges affect daily movement through 11 distinct symptoms that range from localized lower back pain to radiating leg pain, numbness, tingling, muscle weakness, instability, and movement-specific triggers like pain when coughing or bending. A person with a lumbar disc bulge might find they can no longer bend over to tie their shoes without sharp pain, or they experience a shooting sensation down their leg when they try to pick up their groceries. These symptoms develop because the gel-like nucleus of the intervertebral disc presses against the surrounding nerve roots, irritating them and triggering pain signals that travel throughout the lower back and legs. This article examines all 11 symptoms in detail, explains why they occur, when they’re most likely to appear, and what the research shows about recovery and prognosis.
Lumbar disc bulges are remarkably common—affecting 5 to 20 out of every 1,000 adults annually—and they increase substantially with age, with 84% of 80-year-olds showing disc abnormalities on MRI scans. What’s important to understand is that many people have disc bulges visible on imaging but experience no pain whatsoever. The presence of a bulge on an MRI doesn’t automatically predict suffering; symptoms depend on whether and how much the bulge compresses nerve tissue. For most people who do develop symptoms, the good news is that 85 to 90% of patients experience significant relief within 6 to 12 weeks without surgery, though this recovery timeline varies by individual and severity.
Table of Contents
- What Are the Primary Pain Symptoms in Lower Back and Legs?
- How Nerve Compression Creates Numbness, Tingling, and Burning Sensations
- Muscle Weakness and Instability That Disrupts Balance and Movement
- How Difficulty Walking and Standing Progresses with Activity
- When Symptoms Signal Cauda Equina Syndrome or Other Complications
- Understanding Why MRI Findings Don’t Always Match Symptoms
- Recovery Timeline and Long-Term Prognosis
- Conclusion
What Are the Primary Pain Symptoms in Lower Back and Legs?
Lower back pain is the most common symptom of a lumbar disc bulge, and it typically presents as either continuous discomfort or sharp, intermittent pain that worsens with movement, coughing, sneezing, or prolonged standing. The pain can range from mild soreness to severe, debilitating pain that makes even simple tasks like getting dressed difficult. A key distinction is that this pain is usually localized to the lower back initially, though it may radiate downward depending on the location and severity of the bulge. Sciatica, or radiating leg pain, develops when the bulging disc compresses the sciatic nerve, causing pain to shoot from the buttock down the back of the leg toward the calf or foot. This pain is often described as sharp, burning, or electric in nature, and it may occur on one side of the body or both sides depending on the disc’s position.
The pain with sciatica is frequently worse when sitting, bending forward, or lifting objects—movements that increase pressure on the affected nerve. Unlike simple leg pain, sciatic pain typically follows the path of the nerve itself, making it distinctly different from general muscle soreness. Pain with specific movements—bending over, lifting, bringing knees to the chest while lying on the back—represents a fourth distinct symptom because it appears predictably in response to particular actions rather than constantly. People often discover these triggers through painful trial and error: they reach down to pick something up, feel a sharp jab in their lower back or leg, and learn to avoid that movement going forward. This predictability can actually be helpful for understanding the condition, though it also limits daily activities significantly.

How Nerve Compression Creates Numbness, Tingling, and Burning Sensations
When a disc bulge presses directly on a nerve root, it doesn’t just cause pain—it disrupts normal nerve signaling, leading to numbness and tingling sensations in the arms, hands, legs, or feet, depending on which nerve is compressed. These paresthesias, as doctors call them, might feel like pins and needles, a “falling asleep” sensation, or even complete loss of feeling in certain areas. The difference between pain and numbness is important: pain means the nerve is irritated but functioning; numbness suggests the nerve signal itself is being blocked or significantly impaired.
Burning or electric-type sensations are another distinct symptom resulting from irritated nerves, and patients frequently describe them as sharp, shooting sensations rather than dull aches. Someone might feel a sudden electric shock down their leg when they move a certain way, or experience constant burning along the back of the calf. These sensations are particularly distressing because they can be unpredictable and often feel alarming, even though they’re typically not dangerous in themselves. However, numbness and tingling that affects the genital area or inability to control bladder or bowel function requires immediate emergency care, as this indicates cauda equina syndrome, a rare but serious condition requiring urgent surgery.
Muscle Weakness and Instability That Disrupts Balance and Movement
Muscle weakness in the legs or feet often accompanies nerve compression from a lumbar disc bulge, making it harder to walk, climb stairs, or lift objects. This weakness develops because the compressed nerve supplies those muscles with signals to contract; when the signal is compromised, the muscles don’t receive full instructions and weaken accordingly. A person might notice their leg feels “heavy” or that they can’t lift their foot as high when walking, potentially causing them to shuffle or stumble.
Instability while standing or walking represents a related but distinct symptom—the feeling that your legs won’t support you properly or that you might lose your balance without warning. This instability differs from simple weakness because it involves loss of proprioception (your sense of where your body is in space) and compromised muscle coordination. Climbing stairs becomes risky because the affected leg might not be reliable midway up, and standing still on one leg becomes nearly impossible. The fear of falling often leads people to move more cautiously, which can actually weaken muscles further through disuse over time.

How Difficulty Walking and Standing Progresses with Activity
Difficulty walking or standing for prolonged periods is a symptom that typically worsens gradually as the day progresses or activity increases. Someone might be able to walk to their car in the morning but struggle to remain on their feet by afternoon, or they might stand at the kitchen counter cooking and find they need to sit down halfway through. This is distinct from acute pain episodes because it’s tied to fatigue and cumulative stress on the affected structures rather than sudden sharp injury.
The relationship between activity duration and symptom severity is important to understand: most people with lumbar disc bulges can do things, but only for limited periods before discomfort forces them to rest. A person might walk for 15 minutes before pain forces them to sit, or stand at the sink for 10 minutes before their legs feel weak. Some people find that certain positions—like lying down or sitting with the back reclined—actually reduce symptoms by taking pressure off the nerve, while other positions make them worse. This variation between individuals means that one person’s coping strategy (like using a standing desk) might be harmful for someone else with a similar-sounding condition.
When Symptoms Signal Cauda Equina Syndrome or Other Complications
While most lumbar disc bulges resolve without emergency intervention, cauda equina syndrome is a rare but serious condition that requires immediate surgical attention. Symptoms include loss of bladder or bowel control, severe weakness in both legs, numbness in the saddle area (inner thighs, genitals, anal region), and sometimes complete paralysis of the legs. If someone experiences these symptoms, they should seek emergency care immediately, as delay can result in permanent nerve damage and loss of these functions. Fortunately, this complication affects only a small percentage of people with disc bulges, but knowing this warning sign is critically important.
Beyond cauda equina syndrome, some people develop progressive weakness or worsening numbness that suggests the nerve damage is advancing rather than improving. This might indicate that conservative treatments aren’t working and that more aggressive intervention is needed. However, it’s crucial to distinguish between expected fluctuations in symptoms (which are completely normal) and truly progressive deterioration. Most people experience good days and bad days, or improvement that isn’t perfectly linear; this pattern is different from steady worsening over weeks.

Understanding Why MRI Findings Don’t Always Match Symptoms
One of the most confusing aspects of lumbar disc bulges is that 10 to 81% of people with no pain symptoms at all show disc bulges or other abnormalities on MRI scans. This means you can have a disc bulge visible on imaging and feel completely fine, or have minimal symptoms despite a large bulge, while someone else might have severe symptoms from a small bulge. The correlation between what radiologists see on imaging and what patients experience is surprisingly weak, which explains why two people with seemingly identical MRI results can have vastly different symptoms and recovery trajectories.
This disconnect happens because the nerve’s sensitivity, inflammation levels, the bulge’s exact position relative to the nerve, and individual pain perception all influence whether a bulge actually causes symptoms. Age and activity level matter too: disc changes accumulate naturally over time, and at age 80, disc abnormalities are so common they’re almost the norm. Understanding this helps people avoid catastrophizing based on imaging alone or feeling hopeless about their recovery chances.
Recovery Timeline and Long-Term Prognosis
Research shows that 85 to 90% of people with acute herniated disc symptoms experience meaningful relief within 6 to 12 weeks without surgical treatment, meaning that natural recovery is the most common outcome. This recovery typically involves gradual reduction in pain and progressive improvement in function, though the timeline varies significantly between individuals. Some people improve dramatically in 2 to 3 weeks, while others need the full 12 weeks or occasionally longer.
For those whose symptoms persist beyond the typical recovery window, further intervention may be needed, but many of these individuals still improve with continued conservative care. The prognosis depends on factors like age, the severity of nerve compression, the specific location of the bulge, and whether the person has a history of previous back injuries. Moving forward from a lumbar disc bulge involves understanding that recovery is possible, that imaging findings shouldn’t override the reality of how you feel, and that gradual return to activity is usually the safest path.
Conclusion
The 11 symptoms of lumbar disc bulges that affect daily movement—from lower back pain and sciatica to numbness, tingling, burning sensations, muscle weakness, instability, difficulty walking or standing, and movement-specific pain triggers—develop because the bulging disc material compresses nearby nerve roots. However, having a disc bulge visible on imaging doesn’t guarantee you’ll experience symptoms, and most people who do develop symptoms recover naturally within 6 to 12 weeks without surgery.
The most important steps forward involve tracking your specific symptoms and triggers, seeking immediate care only if you experience cauda equina syndrome warning signs, and working with healthcare providers to develop a recovery plan suited to your individual circumstances rather than worrying about what an MRI shows. If you’re experiencing symptoms consistent with a lumbar disc bulge, keeping a symptom diary that notes when pain occurs, what activities triggered it, and how long it lasted can provide valuable information for your healthcare provider. This data helps distinguish between normal fluctuations and concerning progression, guides treatment decisions, and tracks your recovery over time.