When a herniated disc presses on the sciatic nerve, the result is typically a sharp, electric shock-like pain that radiates from the lower back and buttocks down one leg, sometimes all the way to the foot. This happens because the soft inner material of the disc—called the nucleus—breaks through the outer layer and compresses the nerve root, but the damage isn’t purely mechanical. The disc material also releases chemical irritants that trigger nerve inflammation, intensifying the pain and other symptoms. For someone experiencing this, sitting for long periods or standing up might feel unbearable; a simple task like tying shoes can trigger intense discomfort.
This article explains the mechanics of what happens when a disc herniates, why symptoms vary so widely, what treatment options exist, and why most people who develop sciatica do eventually recover—even though the underlying herniated disc might never completely disappear. Sciatica from herniated discs is remarkably common. About 1 to 5 percent of people develop sciatica in any given year, and somewhere between 10 and 40 percent of the population will experience it at some point in their lives. However, there’s an important twist: many people have herniated discs without ever knowing it. Studies show that 20 to 36 percent of people with no pain or symptoms have a herniated disc visible on imaging, and this is especially true in older adults—about 40 out of 100 people over 50 have herniated discs despite feeling perfectly fine.
Table of Contents
- How Does a Herniated Disc Compress the Sciatic Nerve?
- What Symptoms Develop When the Nerve is Compressed?
- Who Is Most Likely to Experience Nerve Compression from a Herniated Disc?
- How Do Doctors Treat Nerve Compression from Herniated Discs?
- What Are the Risks of Long-Term Nerve Compression?
- How Long Does Recovery Typically Take?
- Herniated Discs Versus Sciatica: Why Some People Have One Without the Other
- Conclusion
How Does a Herniated Disc Compress the Sciatic Nerve?
The spine is made up of bones called vertebrae, separated by discs that act as shock absorbers and spacers. Each disc has a tough outer layer called the annulus fibrosus and a softer, gel-like center called the nucleus pulposus. When a disc herniates, the nucleus pushes through tears or weak points in the annulus and can bulge into the spinal canal where the sciatic nerve passes through. The sciatic nerve is the longest nerve in the human body, and when even a small disc fragment presses against it, the effect can be dramatic. The compression itself—the physical squeezing—is only part of the problem.
The disc material also releases chemical irritants and inflammatory substances that inflame the nerve, which is why pain from sciatica can be severe even when imaging shows only modest disc displacement. Think of it like stepping on a hose: you might block water flow with direct pressure, but chemicals seeping from the hose’s material cause additional damage. The reason herniated discs are such a common cause of sciatica is partly related to age and wear. The discs lose water content and flexibility over time, making them more prone to tears. Herniated discs cause approximately 90 percent of sciatica cases, making this the leading mechanical cause of sciatic pain. However, it’s worth noting that a herniated disc in the cervical spine (neck) or thoracic spine (mid-back) won’t compress the sciatic nerve; the relevant herniations are always in the lumbar spine (lower back), where the sciatic nerve roots form.

What Symptoms Develop When the Nerve is Compressed?
When the sciatic nerve is actively compressed and inflamed, the symptoms are distinctive and often unmistakable. The classic presentation includes sharp, burning pain that radiates from the buttocks down the back or side of one leg, sometimes extending into the foot. Many people describe it as an electric shock or shooting pain. Alongside pain, tingling and numbness often develop in the leg and foot, and weakness in the leg, foot, or ankle muscles can make walking, climbing stairs, or pressing the foot down difficult. The pain typically worsens with activities that increase pressure in the disc space, particularly standing for long periods, walking, sitting (especially bending forward), or straightening the affected leg. Someone with sciatica might find they can’t sit through a meal comfortably or take a walk around the block without the pain becoming intolerable.
However, it’s crucial to understand that compression severity varies widely, and so do symptoms. Some people experience only mild tingling; others are nearly disabled by the pain. The intensity of symptoms doesn’t always correlate with the size of the herniation visible on imaging. A person with a large disc bulge might have minimal symptoms, while someone with a smaller herniation might be in significant pain. This is partly because the chemical inflammation component varies, and partly because nerve sensitivity is individual. Additionally, if the herniation is mild and doesn’t actually touch the nerve, there may be no pain at all—the disc might simply bulge into the canal without making contact.
Who Is Most Likely to Experience Nerve Compression from a Herniated Disc?
Sciatica from herniated discs peaks in people in their 40s, though it can occur at younger or older ages. The condition shows no gender predominance, affecting men and women equally. Risk factors include heavy lifting or bending, sedentary work, smoking (which reduces disc nutrition), and obesity (which increases load on the spine). However, one of the most counterintuitive findings is that having a herniated disc and having symptoms are very different things.
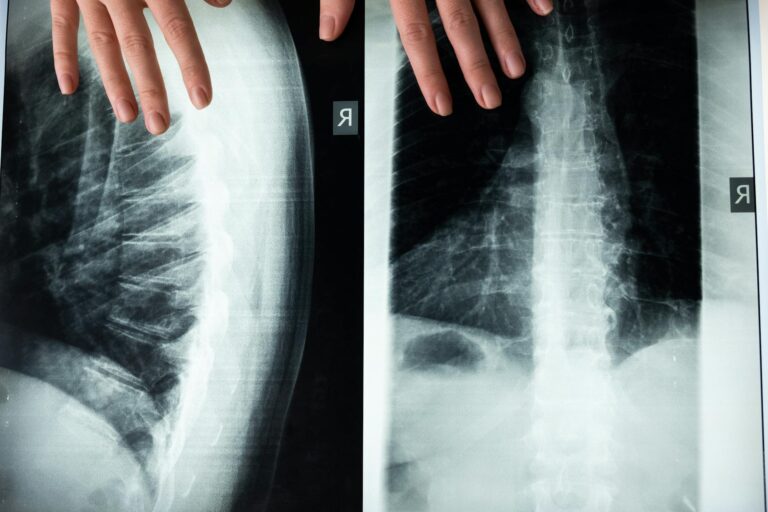
A person in their 20s might have a herniated disc visible on an MRI and feel completely normal; another person the same age might have sciatica symptoms from a smaller disc bulge. For people in their 40s, when peak incidence occurs, around 30 out of 100 have herniated discs on imaging without symptoms. This dramatic disconnect means that the presence of a herniated disc on an MRI doesn’t automatically mean it’s causing your pain—a doctor has to correlate the imaging findings with the person’s actual symptoms and physical examination. Someone who gets an MRI for back pain and is told they have a herniated disc might actually have pain from tight muscles, arthritis, or something unrelated to the disc herniation.

How Do Doctors Treat Nerve Compression from Herniated Discs?
Treatment for sciatica from a herniated disc almost always starts conservatively, meaning without surgery. The goals are to reduce nerve inflammation, manage pain, and restore mobility. Anti-inflammatory medications like ibuprofen or naproxen, combined with muscle relaxers, can reduce pain and spasm. Physical therapy is often recommended to strengthen the core muscles that support the spine and to improve flexibility, reducing pressure on the disc and nerve. Many people benefit from epidural steroid injections, where a corticosteroid is injected into the space around the nerve to reduce inflammation; these are typically given as a series over 4 to 6 weeks. Most importantly, 80 to 90 percent of people recover naturally without any specific treatment beyond activity modification and pain management, with the majority improving within 3 months or less.
Surgery, typically a microdiscectomy (removal of the herniated disc material), is reserved for people with severe, unrelenting symptoms that don’t improve after several weeks or months of conservative treatment. When surgery is performed for refractory symptoms, it provides 80 to 90 percent immediate relief of leg pain in the short term. However, this high success rate in the immediate period doesn’t mean the underlying problem is permanently solved. About 10 percent of people experience a recurrence of herniation after their symptoms have resolved, sometimes months or even years later. So while surgery can be very effective for severe acute pain, it’s not a permanent fix and isn’t undertaken lightly. The decision between continuing conservative treatment and having surgery ultimately depends on how much the symptoms interfere with daily life and how long someone is willing to wait for natural recovery.
What Are the Risks of Long-Term Nerve Compression?
Although most people recover well from sciatica, there are real risks if nerve compression is severe or prolonged. Approximately 1 in 100 people experience permanent nerve damage from disc herniation. This can result in lasting numbness, weakness, or altered sensation in the leg or foot. Additionally, chronic compression can lead to the development of bone spurs (osteophytes) as the spine tries to stabilize itself in response to the disc herniation, which can then cause their own compression problems.
In rare but serious cases—typically when herniation is severe and central (affecting the center of the spinal canal)—cauda equina syndrome can develop, causing bowel and bladder dysfunction, severe bilateral leg pain, and even paralysis. This is a medical emergency requiring immediate surgery. The risk of permanent damage underscores why severe or worsening symptoms warrant prompt medical evaluation rather than indefinite waiting. Warning signs that should prompt urgent evaluation include progressive leg weakness that’s getting worse, loss of control over bladder or bowel, or numbness in the saddle area (inner thighs and buttocks). For the vast majority of people with straightforward sciatica, conservative treatment works well, but severity matters in determining how aggressively to pursue treatment.

How Long Does Recovery Typically Take?
The timeline for recovery from sciatica is one of the most encouraging aspects of this condition. Studies consistently show that 80 to 90 percent of people recover naturally without specific treatment, and most of those who improve do so within 3 months or less. This means that if someone develops sciatica on a Monday, there’s a good chance that by late spring or early summer, they’ll be back to normal.
Some people recover in weeks; others take the full 3 months. A smaller group takes longer—perhaps 6 months to a year—but still eventually improves without surgery. The body has a remarkable capacity to resorb the herniated disc material and for inflammation to settle over time, even as the structural herniation itself might never completely disappear on imaging.
Herniated Discs Versus Sciatica: Why Some People Have One Without the Other
A key distinction that often confuses patients is the difference between having a herniated disc and having sciatica symptoms. A herniated disc is a structural issue—the nucleus has broken through the outer layer of the disc. Sciatica is a symptom—pain from a compressed nerve. Crucially, you can have a herniated disc without sciatica, and in fact, this is very common. Between 20 and 36 percent of people without any back or leg pain have a herniated disc visible on imaging.
In younger people (20-30 years old), about 30 out of 100 have a herniated disc with no symptoms. This disconnect exists because not all herniations are positioned where they can press on a nerve, or the compression, if present, isn’t severe enough to cause symptoms. The chemical irritant component also varies—some disc herniations trigger more inflammation than others. Understanding this distinction helps explain why two people with very similar-looking MRIs can have completely different experiences: one is pain-free, the other is struggling. It also explains why successful treatment sometimes involves reducing inflammation and allowing the nerve to settle, rather than necessarily making the herniated disc itself go away.
Conclusion
When a herniated disc presses on the sciatic nerve, the result is pain and nerve symptoms caused by both mechanical compression and chemical irritation from the disc material. The symptoms—radiating pain, tingling, numbness, and weakness—are distinctive, but severity varies widely based on the size and position of the herniation, individual nerve sensitivity, and the degree of inflammation. The good news is that 80 to 90 percent of people recover naturally within 3 months, often without surgery, through conservative treatment including medication, physical therapy, and epidural steroid injections. The important caveat is that about 1 in 100 people experience permanent nerve damage, and severe cases can develop serious complications like cauda equina syndrome requiring emergency intervention.
If you develop sudden sharp leg pain radiating from the buttocks, tingling, or leg weakness, see a healthcare provider for evaluation. Most people with sciatica will recover completely, but the first step is confirming the diagnosis and ruling out rare emergencies. Many people also benefit from knowing that having a herniated disc visible on an MRI doesn’t automatically mean it’s the source of their pain—clinical correlation with symptoms is essential. For most cases, patience combined with active conservative treatment—staying mobile, doing appropriate exercises, and managing inflammation—is the pathway to recovery.