The best relaxation techniques for dementia patients include music therapy, progressive muscle relaxation, gentle exercise, deep breathing, and multisensory stimulation, though the evidence behind each varies considerably. A 2025 systematic review published in The British Journal of Psychiatry confirmed Level 1 evidence supporting group cognitive stimulation therapy for improving quality of life in dementia, and Level 2 evidence supporting 42 non-pharmacological interventions including those based on exercise, music therapy, reminiscence, and occupational therapy. That broad endorsement matters because it tells caregivers these approaches are not just anecdotal — they have genuine clinical backing.
Consider a person in mid-stage Alzheimer’s who becomes agitated every afternoon around sundown. A caregiver who puts on a familiar Frank Sinatra album, dims overhead lights, and guides the person through slow hand squeezes may be drawing on three separate evidence-based techniques at once — music therapy, sensory environment modification, and gentle touch. None of these requires a prescription, specialized equipment, or clinical training, yet each has at least some research support for reducing behavioral and psychological symptoms of dementia. This article walks through the strongest relaxation techniques available, examines what the research actually shows (including where the evidence falls short), and offers practical guidance for tailoring these interventions to individual needs and disease stages.
Table of Contents
- Which Relaxation Techniques Work Best for Dementia Patients According to Research?
- How Deep Breathing and Gentle Exercise Reduce Agitation in Dementia Care
- Multisensory Stimulation and Touch Therapy for Dementia Relaxation
- Building a Daily Relaxation Routine That Actually Works
- Why Some Popular Techniques Have Weaker Evidence Than You Might Expect
- Adapting Techniques Across Dementia Stages
- Where Dementia Relaxation Research Is Heading
- Conclusion
- Frequently Asked Questions
Which Relaxation Techniques Work Best for Dementia Patients According to Research?
Music therapy stands out as one of the most studied and consistently supported relaxation interventions. A meta-analysis of 12 studies found music interventions had a medium overall effect size on reducing agitation in dementia patients, suggesting what the researchers called “robust clinical relevance” (Frontiers in Psychology, 2017). A separate exploratory randomized controlled trial found that agitation decreased during music therapy sessions compared to standard care, where agitation actually increased, with a statistically significant difference and a moderate effect size of 0.50. Perhaps most compelling for families is the fact that musical memories are retained even in later stages of dementia when other types of memory have deteriorated, which means a person who can no longer recognize a spouse may still light up at a song from their wedding. However, the picture is not uniformly positive even for music therapy. A 2024 systematic review examining 35 RCTs comprising 4,043 patients found that while music-based interventions effectively improved behavioral and psychological symptoms, anxiety, and depression, they did not reach statistical significance for agitation specifically.
That distinction matters. If a caregiver’s primary goal is reducing a specific behavior like repetitive vocalizing or physical restlessness, music alone may not be sufficient, and combining it with other techniques often produces better results. Progressive muscle relaxation also has meaningful evidence behind it. A study examining PMR performed 15 minutes daily for 90 days showed improvements in interest, volition, and social relationships in dementia patients at both 30-day and 90-day follow-ups. Researchers noted that PMR can change stress thresholds and reduce behavioral and psychological symptoms of dementia overall. The key limitation here is that PMR requires the person to follow verbal instructions — tensing and releasing specific muscle groups — which becomes increasingly difficult in later disease stages.
How Deep Breathing and Gentle Exercise Reduce Agitation in Dementia Care
Deep breathing exercises represent the most accessible calming technique available because they require no equipment, no training, and minimal cognitive capacity. Deep, rhythmic breathing activates the parasympathetic nervous system, suppressing the fight-or-flight response while lowering heart rate and blood pressure. For a person with dementia who is becoming visibly distressed — clenching fists, pacing, raising their voice — a caregiver who sits beside them, breathes audibly and slowly, and gently encourages them to match the rhythm can sometimes de-escalate the moment within minutes. The limitation is that deep breathing works best as an early intervention, before agitation peaks. Once a person with dementia reaches full distress, their ability to process and follow breathing cues drops sharply.
Caregivers who recognize early warning signs — slight restlessness, changes in facial expression, repetitive movements — and introduce breathing exercises at that point tend to see far better results than those who wait until the person is already in crisis. Exercise offers benefits that extend well beyond in-the-moment relaxation. An RCT found that strength, balance, and flexibility exercises were statistically significantly more effective than both a walking group and a social conversation control in reducing dementia symptoms. A 2025 review published in Frontiers in Aging Neuroscience explains the biological mechanisms: exercise therapy alleviates Alzheimer’s symptoms by enhancing mitochondrial function, reducing neuroinflammation, increasing neurotrophic factor levels, and elevating irisin levels. Meanwhile, an NIH-funded study is currently comparing traditional tai chi to a cognitively enriched form that adds mental puzzles, investigating whether combining physical and cognitive challenges can slow mild cognitive impairment more effectively than movement alone.
Multisensory Stimulation and Touch Therapy for Dementia Relaxation
Snoezelen rooms — dedicated multisensory environments that use a combination of light effects, calming sounds, scents, and tactile stimulation to engage multiple senses simultaneously — have become increasingly common in memory care facilities. The concept originated in the Netherlands in the 1970s and is built on the idea that sensory engagement can bypass the cognitive deficits of dementia and reach a person on a more instinctive level. A person who cannot follow a conversation may still respond to the warmth of fiber-optic lights shifting color, the scent of lavender, and the texture of a weighted blanket. Short-term benefits from Snoezelen environments have been reported in the literature, including reduced agitation and improved mood during and immediately after sessions. However, durable long-term effects were not consistently demonstrated across studies.
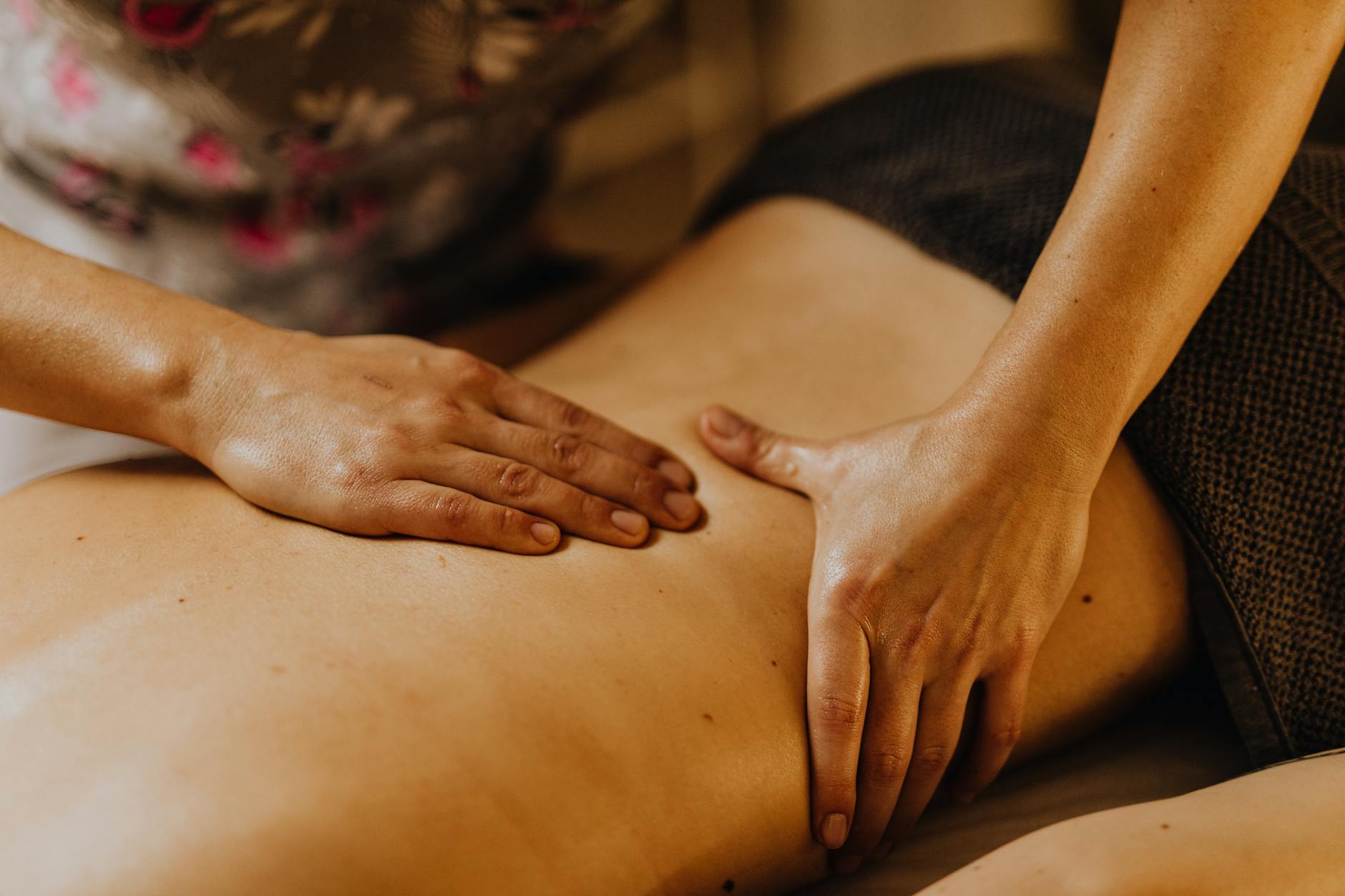
This is an important caveat for families evaluating memory care facilities that advertise Snoezelen rooms — the rooms can be genuinely helpful as part of a daily routine, but they are not a standalone treatment that produces lasting behavioral changes after a single session or even a short series. Touch therapy, particularly hand massage, has a smaller but encouraging evidence base. Two small RCTs found that hand massage combined with calming music significantly reduced agitation compared to no treatment. The combination is key — touch alone and music alone each have effects, but pairing them appears to amplify the benefit. For home caregivers, this is one of the most practical interventions available. It requires nothing more than lotion, a quiet room, and a playlist of music the person enjoyed in earlier decades.

Building a Daily Relaxation Routine That Actually Works
The single most effective relaxation strategy for dementia patients is not any one technique but rather a structured, predictable daily environment. Structured routines and predictable environments reduce anxiety on their own. Simplifying tasks, reducing visual and auditory clutter, and communicating calmly with sufficient response time all lower the baseline stress level from which agitation emerges. A person whose day follows a consistent pattern — morning hygiene, breakfast, a short walk, music time, lunch, rest, an activity, dinner — experiences far less confusion-driven anxiety than someone whose schedule varies unpredictably. The tradeoff is between structure and flexibility. Too rigid a schedule creates its own problems when disruptions inevitably occur — a doctor’s appointment, a visiting relative, a change in weather that prevents an outdoor walk.
The most effective approach builds a loose framework with consistent anchor points (mealtimes, bedtime routine) while allowing the spaces between to adapt. When disruptions happen, returning to the routine as quickly as possible minimizes the cascading anxiety that can result from one unexpected change. Personalization matters enormously. A 2024 review in The Gerontologist emphasized that interventions should be personalized to the individual’s preferences, history, and stage of disease for best results. A retired jazz musician may find classical piano music irritating rather than soothing. A former gardener may respond better to the smell of soil and herbs than to lavender essential oil. The more a caregiver knows about the person’s life before dementia — their career, hobbies, cultural background, favorite sensory experiences — the more effective any relaxation technique will be.
Why Some Popular Techniques Have Weaker Evidence Than You Might Expect
Mindfulness-based interventions, despite their enormous popularity in general wellness culture, have surprisingly weak evidence in dementia care specifically. A meta-analysis of 8 RCTs involving 276 patients found no significant effects for mindfulness-based interventions on any measured outcomes compared to control conditions. The evidence remains limited, and the likely explanation is straightforward: mindfulness meditation requires sustained attention, meta-awareness, and the ability to redirect wandering thoughts — cognitive capacities that are progressively compromised by dementia. This does not mean mindfulness is useless for caregivers themselves, where the evidence is much stronger, but recommending it directly to dementia patients based on current data would be premature.
Aromatherapy occupies a similar middle ground. Scents like lavender, vanilla, and peppermint can create calming environments, and many caregivers report positive anecdotal results. However, robust clinical evidence is still developing, and the effects are difficult to isolate from the broader sensory environment in which aromatherapy is typically used. A lavender-scented room that is also quiet, dimly lit, and staffed by a calm caregiver may produce relaxation that has more to do with the overall environment than the scent itself. Aromatherapy is best understood as one component of a multisensory approach rather than a standalone treatment.

Adapting Techniques Across Dementia Stages
In early-stage dementia, when a person retains significant cognitive function, progressive muscle relaxation, guided deep breathing, tai chi, and even simplified mindfulness exercises are all viable options. A person at this stage can follow multi-step instructions and may benefit from learning techniques they can eventually use independently. This is the stage where building habits around relaxation has the highest return, because those habits — the association between a particular chair and breathing exercises, or between afternoon and a favorite album — can persist through muscle memory and routine even as cognitive decline progresses.
In moderate to advanced stages, caregiver-led and sensory-based techniques become more appropriate. Music therapy retains its effectiveness because musical memory is preserved late into the disease. Hand massage with music, Snoezelen-style sensory stimulation, and simple rhythmic movement like gentle rocking or swaying to music all work without requiring the person to process verbal instructions. The caregiver’s own demeanor becomes the most powerful tool at this stage — a calm voice, unhurried movements, and warm touch communicate safety more effectively than any structured protocol.
Where Dementia Relaxation Research Is Heading
The research landscape is shifting toward combination therapies and personalized intervention protocols rather than testing single techniques in isolation. The NIH-funded study comparing traditional tai chi to cognitively enriched tai chi reflects this trend — the question is no longer just whether movement helps, but whether layering cognitive engagement onto physical activity produces compounding benefits. Similarly, the 2025 Frontiers review identifying specific biological mechanisms behind exercise benefits — mitochondrial function, neuroinflammation reduction, neurotrophic factor elevation — points toward a future where exercise prescriptions for dementia patients may be calibrated based on biomarkers rather than general guidelines.
For families and caregivers, the practical takeaway from current research trends is cautiously optimistic. The evidence base for non-pharmacological relaxation techniques continues to grow, and the consistent finding across reviews is that these approaches carry minimal risk and meaningful potential benefit. As personalized medicine advances, expect to see more tailored recommendations based on individual disease profiles, genetic factors, and personal histories rather than one-size-fits-all protocols.
Conclusion
The strongest evidence supports music therapy, progressive muscle relaxation, structured exercise, and multisensory stimulation as relaxation techniques for dementia patients, with deep breathing and touch therapy as practical supplementary approaches. A 2025 systematic review confirmed Level 1 and Level 2 evidence for dozens of non-pharmacological interventions, giving caregivers legitimate confidence that these strategies are clinically grounded. The most important principle across all techniques is personalization — matching interventions to the individual’s life history, current disease stage, and sensory preferences.
No single technique will work for every person or every situation. The most effective caregivers build a toolkit of multiple approaches, learn to read early signs of agitation, and intervene with the right technique at the right moment. Starting with familiar music and a calm, predictable daily structure provides a solid foundation, and layering in additional techniques like PMR, gentle exercise, or hand massage allows for adjustment as needs change over time.
Frequently Asked Questions
Can dementia patients do relaxation exercises on their own?
In early stages, yes — particularly deep breathing and progressive muscle relaxation, especially if these were practiced before significant cognitive decline. In moderate to advanced stages, most relaxation techniques need to be caregiver-led, relying on sensory cues, physical touch, and environmental design rather than verbal instructions.
How long should a relaxation session last for someone with dementia?
Most studies used sessions of 15 to 30 minutes. The PMR study showing positive results used 15-minute daily sessions over 90 days. Shorter, more frequent sessions tend to work better than longer ones, particularly in later disease stages where attention spans are limited.
Is music therapy effective in late-stage dementia?
Yes, and this is one of its most significant advantages. Musical memories are retained even when other types of memory have deteriorated, making music therapy one of the few interventions that remains effective across all stages of dementia progression.
Does mindfulness meditation help dementia patients?
Current evidence does not support it. A meta-analysis of 8 RCTs found no significant effects for mindfulness-based interventions compared to control conditions. The cognitive demands of mindfulness — sustained attention, self-monitoring, thought redirection — are progressively impaired by dementia, which likely explains the poor results.
Are Snoezelen rooms worth seeking out in a memory care facility?
They can be a valuable component of care but should not be a deciding factor on their own. Research shows short-term benefits during and immediately after sessions, but durable long-term effects have not been consistently demonstrated. A facility’s overall approach to routine, personalization, and staff training matters more than any single amenity.
What is the simplest relaxation technique a family caregiver can start with today?
Playing familiar music from the person’s young adult years (typically ages 18 to 25) in a calm environment. It requires no training, no equipment beyond a speaker, and has some of the strongest research support of any non-pharmacological intervention for dementia.




