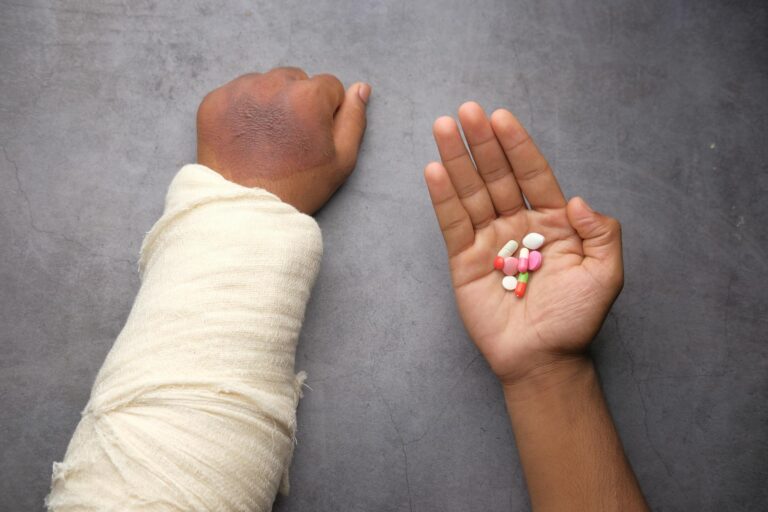
Acetaminophen, ibuprofen, and aspirin — three of the most commonly used drugs in the United States — are all linked to hearing loss when taken regularly. That means the bottle of Tylenol or Advil sitting in your medicine cabinet, the one you reach for twice a week for that nagging back pain or recurring headache, could be quietly damaging your ability to hear. A landmark Harvard study of nearly 27,000 men found that regular use of acetaminophen increased the risk of hearing loss by 22 percent, with younger men under 50 facing nearly double the risk.
For families dealing with dementia and cognitive decline, this finding deserves serious attention. Hearing loss is one of the largest modifiable risk factors for dementia, and millions of older adults take these painkillers on a near-daily basis for arthritis, chronic pain, or cardiovascular protection. The connection between something so ordinary and a consequence so significant has been quietly building in the research literature for over a decade. This article breaks down which over-the-counter pain relievers carry the most risk, how they damage your hearing at the cellular level, what the research says about men and women separately, whether the damage is reversible, and what practical steps you can take — especially if you or someone you care for already lives with some degree of hearing loss.
Table of Contents
- Which Over-the-Counter Drugs Cause Hearing Loss With Regular Use?
- What the Research Found in Men — And Why Age Matters
- What the Research Found in Women — Duration Makes It Worse
- How These Drugs Actually Damage Your Hearing
- When Hearing Loss Already Exists — The Risk of Progression
- Aspirin’s Unusual Position — Low Dose Appears Safe
- Where This Research Is Headed and What It Means for Brain Health
- Conclusion
- Frequently Asked Questions
Which Over-the-Counter Drugs Cause Hearing Loss With Regular Use?
There are more than 200 known ototoxic medications — drugs that can damage the structures of the inner ear — according to the American Speech-Language-Hearing Association. But the three that matter most to the general public are the ones nearly everyone has at home: aspirin, NSAIDs like ibuprofen and naproxen, and acetaminophen, sold under the brand name Tylenol. These aren’t obscure chemotherapy agents or powerful antibiotics. They’re the pills people take without a second thought, often without consulting a doctor at all. What makes this particularly concerning is scale. Because these are the most commonly used drugs in the country, even a modest increase in risk translates into an enormous number of affected people.
A study from the Nurses’ Health Study at Harvard estimated that roughly 16.2 percent of hearing loss in women could be attributed to ibuprofen or acetaminophen use alone, assuming the relationship is causal. That is not a small number. For context, if you gathered ten women with hearing loss in a room, the pain relievers in their bathroom cabinets may have contributed to the problem for one or two of them. It is worth noting, however, that not all doses and frequencies carry the same risk. Low-dose aspirin at 100 milligrams per day or less — the kind many people take for heart protection — has not been linked to hearing side effects in the research. The trouble begins with regular use, generally defined as two or more days per week, sustained over months or years. The occasional ibuprofen for a sprained ankle is a different story than taking it every other day for chronic joint pain.

What the Research Found in Men — And Why Age Matters
The most cited study on this topic was published in the American Journal of Medicine in 2010, conducted by researchers at Brigham and Women’s Hospital and Harvard. They followed 26,917 men aged 40 to 74 over a combined 369,079 person-years of follow-up, during which 3,488 cases of hearing loss were reported. The design was rigorous, the sample was large, and the results were consistent across all three drug categories. Men who used aspirin regularly — two or more days per week — had a 12 percent increased risk of hearing loss compared to those who rarely used it. For NSAIDs like ibuprofen, the risk climbed to 21 percent. Acetaminophen carried the highest relative risk at 22 percent. These numbers are hazard ratios, meaning they account for other variables like age, smoking, and noise exposure.
They represent a real, independent effect of the drugs themselves. The finding that should give the most pause, however, involves age. Among men under 50, the risks were dramatically higher. Aspirin use was associated with a 33 percent increased risk. NSAIDs jumped to 61 percent. And acetaminophen nearly doubled the risk of hearing loss — a 99 percent increase. The researchers did not fully explain why younger men were more vulnerable, but the pattern was clear and statistically significant. If you are in your 40s and reaching for ibuprofen several times a week, the data suggests your ears may be paying a price you will not notice for years.
What the Research Found in Women — Duration Makes It Worse
A separate but equally important study came out of the Nurses’ Health Study at Harvard in 2016, examining over 54,000 women aged 48 to 73. The results largely confirmed what the men’s study had shown, with one important addition: the longer women used these painkillers, the greater the risk became. Women who used acetaminophen two to three days per week had an 11 percent increased risk of hearing loss. At four to five days per week, the risk rose to approximately 21 percent. And women who had been using these medications for six or more years faced higher risks still.
This dose-response relationship — more use, more damage — is one of the hallmarks researchers look for when trying to distinguish a genuine causal effect from a statistical coincidence. The women’s study also produced the striking estimate that 16.2 percent of hearing loss cases among participants could be linked to ibuprofen or acetaminophen use. That figure assumes causality, which has not been proven through a randomized trial and likely never will be for ethical reasons. But the consistency across two large, well-designed studies involving both sexes gives the finding considerable weight. For women managing chronic conditions like fibromyalgia, osteoarthritis, or frequent migraines — conditions that often lead to daily or near-daily painkiller use — this is information worth discussing with a doctor.

How These Drugs Actually Damage Your Hearing
The mechanisms differ by drug, which is part of what makes this so insidious. NSAIDs like ibuprofen and naproxen harm hearing by reducing blood flow to the cochlea, the snail-shaped organ deep in the inner ear where sound waves are converted to electrical signals. The cochlea depends on a rich blood supply to keep its delicate sensory hair cells alive and functioning. When that blood flow is chronically reduced, those hair cells begin to deteriorate. Once they are gone, they do not grow back. Humans are born with about 15,000 hair cells per ear, and every one that dies is a permanent loss. Acetaminophen works through a different pathway.
It depletes glutathione, an antioxidant compound that serves as the cochlea’s primary defense against oxidative stress, including the kind caused by everyday noise exposure. Think of glutathione as a buffer that absorbs the damage from loud restaurants, traffic, and headphone use. When acetaminophen strips that buffer away, the cochlea is left exposed. A level of noise that your ears would normally handle just fine can now cause lasting damage. This may explain why acetaminophen carried the highest risk in the men’s study — it does not just harm the ear directly, it removes the ear’s ability to protect itself. Aspirin at high doses — six to eight grams per day, far above what most people take — directly causes tinnitus and hearing loss through a mechanism that affects the outer hair cells of the cochlea. The important distinction with aspirin is that these effects are usually reversible once the dose is reduced or stopped. That is not reliably the case with NSAIDs or acetaminophen, where long-term use without monitoring may produce permanent damage, according to the American Speech-Language-Hearing Association.
When Hearing Loss Already Exists — The Risk of Progression
For anyone already living with some degree of hearing loss — and that includes a substantial portion of adults over 65 — the stakes are even higher. Research reported by AARP found that NSAID use was associated with a 45 percent higher risk of progression of existing hearing loss. That means ibuprofen does not just contribute to hearing loss in the first place; it can accelerate decline that is already underway. This has direct implications for dementia care. Hearing loss is strongly associated with cognitive decline, social isolation, and faster progression of dementia symptoms.
An older adult who takes ibuprofen daily for arthritis pain and already wears hearing aids may be inadvertently making both their hearing and their cognitive situation worse. The cruel irony is that the pain they are treating is real and needs management, but the tool they are using may be compounding a separate and equally serious problem. The limitation here is that we do not have randomized controlled trial data isolating this effect, so the 45 percent figure comes from observational research. Nonetheless, it aligns with everything else we know about how NSAIDs affect cochlear blood supply. If you or someone in your family uses hearing aids and also takes ibuprofen or naproxen regularly, this is a conversation worth having with a physician — not to stop pain management entirely, but to explore whether alternatives exist.

Aspirin’s Unusual Position — Low Dose Appears Safe
Aspirin occupies a unique place in this discussion. Millions of Americans take low-dose aspirin daily, typically 81 milligrams, for cardiovascular protection. The good news from the research is that low-dose aspirin at 100 milligrams per day or less has not been linked to hearing side effects. The ototoxic effects of aspirin appear to be dose-dependent and, importantly, reversible.
This stands in contrast to ibuprofen and acetaminophen, where damage may accumulate silently over years and become permanent. That said, regular-strength aspirin taken at higher doses — the kind someone might use for chronic pain — does carry measurable risk, as the 12 percent increase in hearing loss from the Harvard men’s study showed. The distinction between a baby aspirin for your heart and two full-strength aspirin twice a day for back pain is clinically meaningful when it comes to your ears. If you have been advised by a cardiologist to take low-dose aspirin, this research should not cause you to stop. But if you are self-medicating with full-strength aspirin for pain on a regular basis, a different calculus applies.
Where This Research Is Headed and What It Means for Brain Health
The connection between ototoxic painkillers and hearing loss is likely to receive more attention in the coming years, particularly as the relationship between hearing loss and dementia becomes more widely understood. The 2020 Lancet Commission on dementia prevention identified hearing loss as the single largest modifiable risk factor for dementia, responsible for more attributable risk than smoking, depression, or physical inactivity. Any factor that worsens hearing loss — including chronic use of common painkillers — becomes relevant to the broader fight against cognitive decline. Researchers are beginning to explore whether monitoring hearing should become a standard part of care for patients on long-term analgesic therapy, much the way kidney function is monitored for chronic NSAID users.
For now, that is not standard practice, and most people who take these drugs regularly have never been told they might affect their hearing. That gap between what the research shows and what patients are told represents both a failure and an opportunity. The information exists. It just has not reached the people who need it most.
Conclusion
The evidence is now substantial and consistent: regular use of acetaminophen, ibuprofen, and high-dose aspirin increases the risk of hearing loss, with acetaminophen appearing to carry the highest relative risk — especially for people under 50. The mechanisms are understood, the studies are large and well-designed, and the dose-response relationship strengthens the case for a genuine causal link. For anyone already experiencing hearing loss, NSAIDs may accelerate the decline by as much as 45 percent.
None of this means you should suffer through pain without relief. It means that the decision to take these drugs regularly deserves the same thoughtfulness as any other medical choice. Talk to a doctor about alternatives, get your hearing tested as a baseline, and if you are caring for someone with dementia, pay attention to how often painkillers are being used and whether hearing seems to be changing. Protecting hearing is one of the most concrete things anyone can do to protect the brain, and it starts with knowing which everyday habits carry hidden costs.
Frequently Asked Questions
Can occasional use of ibuprofen or Tylenol cause hearing loss?
The research focused on regular use, defined as two or more days per week sustained over time. Occasional use — taking ibuprofen once for a headache or Tylenol a few times after dental work — has not been shown to carry meaningful risk. The concern is with chronic, habitual use over months or years.
Is the hearing loss from these drugs permanent?
It depends on the drug. Aspirin-related hearing loss is usually reversible when the dose is reduced or stopped. However, damage from long-term NSAID or acetaminophen use may become permanent if it continues without monitoring, according to the American Speech-Language-Hearing Association.
Does low-dose aspirin for heart health affect hearing?
No. Research has not found a link between low-dose aspirin at 100 milligrams per day or less and hearing side effects. The ototoxic effects of aspirin appear at much higher doses, typically six to eight grams per day. If your cardiologist has prescribed baby aspirin, this research should not change that decision.
Which painkiller is safest for hearing?
Among the three studied, low-dose aspirin carries the least hearing risk and its effects are reversible. Acetaminophen showed the highest relative risk in the Harvard men’s study, particularly for younger users. There is no perfectly “safe” option for regular use, which is why discussing alternatives and monitoring with a physician matters.
Can these drugs make existing hearing loss worse?
Yes. NSAID use was associated with a 45 percent higher risk of progression among people who already had hearing loss. This is particularly relevant for older adults who may be managing both chronic pain and age-related hearing decline simultaneously.
How does hearing loss from painkillers relate to dementia risk?
Hearing loss is the single largest modifiable risk factor for dementia, according to the 2020 Lancet Commission. Any factor that contributes to or accelerates hearing loss — including chronic painkiller use — is indirectly relevant to dementia prevention. Protecting hearing is one of the most actionable steps for supporting long-term brain health.