Physical therapy is the gold standard treatment for herniated and degenerative discs, with 70–90% of patients experiencing meaningful recovery using conservative physical therapy alone. The routine typically combines pain management techniques (ice, heat, and manual therapy), flexibility exercises to improve movement, core strengthening to stabilize the spine, and posture correction to reduce ongoing disc pressure. A person with a herniated disc in the lower back, for example, would begin with gentle stretches and ice therapy to manage inflammation, progress to targeted core exercises within a few days or weeks, and eventually work toward regaining full functional capacity—all without surgery in the vast majority of cases. This article explores the specific physical therapy techniques used for disc recovery, why they work, how long improvement typically takes, and what factors determine success.
Table of Contents
- What Physical Therapy Exercises Target Herniated Discs?
- How Long Does Disc Recovery Take with Physical Therapy?
- The McKenzie Method and Spinal Extension Exercises
- Building Your Personalized Disc Recovery Program
- When Physical Therapy May Not Be Enough
- The Role of Manual Therapy in Disc Recovery
- Long-term Spine Health After Disc Injury
- Conclusion
What Physical Therapy Exercises Target Herniated Discs?
The standard physical therapy routine for disc recovery focuses on five core components designed to reduce pain, restore movement, and prevent re-injury. Pain management is the first priority, using ice and heat modalities along with manual therapy—such as joint mobilization and soft tissue massage—to reduce muscle spasms and decrease pressure on the affected nerve. Once pain subsides enough to tolerate movement, flexibility and stretching exercises help restore normal spinal motion.
A patient might perform gentle hamstring stretches, knee-to-chest movements, or cat-cow spinal flexion exercises, all designed to improve range of motion without aggravating the injury. Core strengthening forms the backbone of long-term recovery, targeting the deep abdominal muscles and multifidus (deep spinal stabilizers) that hold the spine upright and protect the discs during daily activities. Unlike superficial abdominal crunches, these exercises activate muscles you feel as much as stability gains—imagine bracing your core as if preparing to be punched, which activates the transversus abdominis and internal obliques that truly stabilize the lumbar spine.
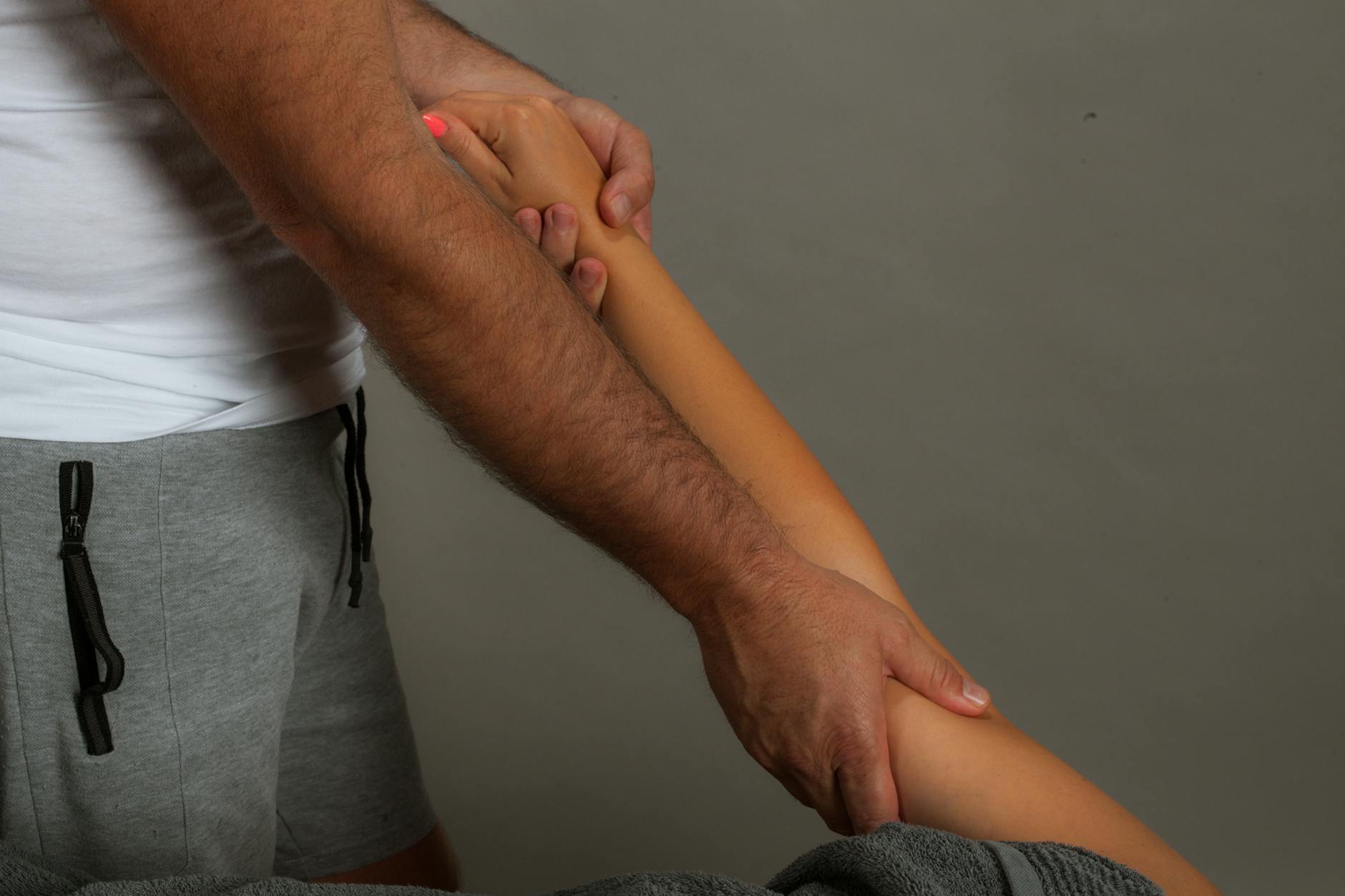
How Long Does Disc Recovery Take with Physical Therapy?
Recovery from a herniated disc follows a predictable timeline when physical therapy is pursued consistently. most patients begin noticing meaningful improvements in pain levels and functional status within 2–6 weeks of starting therapy, which reinforces compliance and helps patients believe recovery is possible. By 3–6 months of consistent therapy, many achieve substantial functional recovery—returning to work, exercise, and daily activities without restrictions.
However, this is not the end of the recovery process: the biological remodeling of the disc itself takes 12–18 months to complete fully. This means that while you feel better and move normally after 3–6 months, the actual cellular healing inside the disc continues for another year or more. A person who stops all exercises after 6 months and resumes old posture habits can experience a setback, because the disc has not fully healed at that point. Approximately 75% of patients with a herniated disc recover spontaneously within 6 months using conservative care—a statistic that surprises many people who fear they’ll need surgery, but it underscores just how effective the body’s own healing mechanisms are when supported by targeted therapy.
The McKenzie Method and Spinal Extension Exercises
The McKenzie Method of Mechanical Diagnosis and Therapy (MDT) is the most commonly prescribed physical therapy protocol for disc herniations and represents the gold standard for chronic low back pain—clinical evidence shows superior results compared to other rehabilitation approaches. The method is based on spinal extension exercises designed to restore the normal inward curve of the lower spine (lumbar lordosis) and, critically, to move pain from the leg back toward the spine’s midline, a phenomenon called “centralization.” When a therapist teaches spinal extension movements—such as prone press-ups or standing extension bends—they watch for this centralization sign: if pain shifts from the calf or foot back toward the low back itself, it’s a positive indicator that the disc is responding well and recovery is likely.
A patient with pain radiating down the leg might perform gentle extension exercises that seem counterintuitive at first, but as they continue and feel the pain migrate closer to the spine, they gain confidence that therapy is working. One important caveat: the McKenzie Method shows superior results for *chronic* low back pain but not for acute low back pain in the first days or weeks—for new injuries, other forms of carefully graded rehabilitation are equally effective. This is why an acute disc herniation might start with flexion-based stretches and pain control before progressing to extension work as inflammation subsides.

Building Your Personalized Disc Recovery Program
A successful physical therapy program for disc recovery requires three critical success factors: consistent attendance at scheduled therapy sessions, diligent performance of home exercises between sessions, and deliberate lifestyle modifications that reduce disc stress. Clinical evidence shows that patients who attend therapy regularly and perform prescribed exercises at home progress significantly faster than those who attend sporadically or skip home work. Your physical therapist will typically prescribe 2–3 sessions per week for 4–8 weeks, with each session including hands-on manual therapy, guided exercise instruction, and progression planning.
Between sessions, you’re expected to perform the same exercises at home—usually 10–15 minutes daily—which actually exceeds the volume of formal therapy. Lifestyle modifications might include adjusting your work posture, taking frequent standing breaks if you have a desk job, using proper lifting techniques, sleeping on your side rather than your back (which reduces disc pressure), and avoiding activities that reproduce your pain until you’re stronger. The comparison is worth noting: a person who attends three therapy sessions per week but sits slouched at a desk for 8 hours daily and avoids home exercises will progress far more slowly than someone who attends twice weekly but maintains perfect posture, performs daily exercises, and modifies problematic activities.
When Physical Therapy May Not Be Enough
While 90% of herniated disc patients recover through conservative treatment alone, approximately 10% do require surgical intervention. Physical therapy should be considered adequate if you’re showing steady progress—decreasing pain, increasing range of motion, improving functional capacity—within the first 6–12 weeks. Warning signs that surgery might become necessary include: progressive neurological symptoms such as increasing weakness, loss of bowel or bladder control (cauda equina syndrome, a medical emergency), or pain that worsens despite 6–12 weeks of consistent physical therapy.
Another scenario where surgery becomes relevant is if your herniation is so large that the disc material is compressing the nerve root severely, causing significant weakness in the leg that prevents normal function even with therapy. However, severity of imaging findings alone does not predict who needs surgery; some people with massive herniations on MRI do fine with physical therapy, while others with small bulges suffer persistent symptoms. This is why your therapist and physician assess *your symptoms and function* rather than relying solely on imaging. If you’ve committed to therapy for 12 weeks with minimal improvement, or if functional limitations are so severe you cannot work or maintain activities of daily living, it’s reasonable to discuss surgical consultation with your physician—but this pathway represents a minority of cases.

The Role of Manual Therapy in Disc Recovery
Manual therapy—performed by a licensed physical therapist—plays a supportive role in disc recovery by addressing muscle tightness and joint restrictions that accompany disc injuries. When a disc herniates, surrounding muscles reflexively tighten to protect the spine, creating stiffness and further limiting movement. A therapist uses joint mobilization techniques (gentle oscillating movements of the spine and pelvis) and soft tissue massage to relieve this guarding, making it easier for you to tolerate exercise.
In one example, a patient with a disc herniation at L4–L5 might have tightness in the piriformis muscle deep in the buttock, which irritates the sciatic nerve and amplifies leg pain even though the primary problem is the disc. Manual release of that tight muscle, combined with stretching and trigger-point work, reduces the secondary irritation and allows other therapeutic exercises to be more effective. Manual therapy is never sufficient on its own—you must combine it with your own active exercises and lifestyle changes—but it serves as a bridge that makes active rehabilitation more tolerable and effective during the acute phase.
Long-term Spine Health After Disc Injury
Once you’ve recovered from an acute disc herniation with physical therapy, your ongoing challenge is preventing re-injury and maintaining the strength gains you’ve earned. Eight out of ten clinical guidelines reviewed recommend physical therapy as the foundation for disc herniation recovery, and these same guidelines emphasize that continued core maintenance—even after you’re symptom-free—reduces the recurrence risk significantly.
Many people return to activity after 3–6 months of good improvement and gradually let their exercise routine lapse, believing they’re “fixed.” However, your disc still has 6–12 additional months of biological remodeling ahead, and the deeper stabilizer muscles can atrophy quickly without continued stimulation. A sustainable long-term approach involves performing a simplified version of your therapeutic exercises 2–3 times per week indefinitely—not the intensive program you did during acute recovery, but enough to maintain core endurance and spinal stability. This forward-looking perspective transforms recovery from a temporary treatment phase into a lifestyle adjustment that protects your spine for decades.
Conclusion
The physical therapy routine for disc recovery is a evidence-based, multi-modal approach combining pain management, flexibility work, core strengthening, manual therapy, and posture correction. Recovery typically progresses rapidly—within 2–6 weeks you notice meaningful improvement, and within 3–6 months most people regain full functional capacity—but the underlying biological healing continues for 12–18 months. Seventy to 90% of herniated disc patients recover fully through physical therapy alone, avoiding surgery and the risks it carries, provided they remain consistent with their exercises, attend therapy regularly, and modify activities that stress the injured disc. The key to success is viewing physical therapy not as a temporary fix but as the beginning of long-term spine health.
Your therapist will teach you specific techniques—possibly including the evidence-backed McKenzie Method if extension movements produce centralization—and send you home with exercises to perform daily. The work you do at home matters as much as, or more than, the work done in the clinic. If you commit fully to this approach and show progress over 6–12 weeks, you’re very likely on the path to durable recovery. If progress stalls or neurological symptoms worsen, then consultation with your physician about surgical options becomes reasonable—but for the vast majority of disc herniation patients, persistent conservative care with physical therapy delivers full recovery without ever needing an operating room.





