A class of drugs known as JAK inhibitors has emerged as the first FDA-approved treatment specifically for severe alopecia areata, and clinical trial data has shown that a majority of patients experienced meaningful hair regrowth within several months of starting therapy. Baricitinib, marketed as Olumiant, became the first such drug to receive FDA approval for alopecia areata in 2022, followed by ritlecitinib (Litfulo) in 2023, giving patients two oral options where previously none existed. For someone like a 45-year-old woman who lost nearly all her scalp hair over the course of a year, these medications have represented a genuine turning point — trial participants in her situation went from wearing wigs daily to seeing substantial regrowth that allowed them to stop covering their heads entirely.
This development matters beyond dermatology circles, and it holds particular relevance for readers following brain health and neurological research. Alopecia areata is an autoimmune condition, and the inflammatory pathways it shares with neuroinflammation — a key driver of cognitive decline and dementia — make these treatment advances worth watching closely. The JAK inhibitor mechanism that calms the immune system’s attack on hair follicles operates on some of the same signaling pathways researchers are now investigating in Alzheimer’s disease and other neurodegenerative conditions. This article covers how these drugs work, what the clinical results actually show, the important limitations patients should understand, and why the autoimmune connection between hair loss and brain health deserves more attention than it currently receives.
Table of Contents
- How Does the New Drug for Alopecia Areata Regrow Hair in Most Patients?
- What Are the Risks and Limitations of JAK Inhibitors for Hair Loss?
- The Autoimmune Connection Between Alopecia Areata and Brain Health
- Comparing Treatment Options for Alopecia Areata Today
- What Happens When Treatment Is Stopped — and Who Should Be Cautious
- Emotional and Psychological Dimensions of Hair Loss in Aging and Dementia
- Where Research Goes From Here
- Conclusion
- Frequently Asked Questions
How Does the New Drug for Alopecia Areata Regrow Hair in Most Patients?
JAK inhibitors work by blocking Janus kinase enzymes, which act as chemical messengers inside immune cells. In alopecia areata, the immune system mistakenly sends T cells to attack hair follicles, treating them as foreign invaders. By inhibiting the JAK-STAT signaling pathway, these drugs essentially tell the immune system to stand down, removing the assault on follicles and allowing them to resume their normal growth cycle. The mechanism is not a cure — it manages the condition rather than eliminating it — but the effect on hair regrowth has been striking in clinical settings. In pivotal trials for baricitinib, roughly 35 to 40 percent of patients with severe alopecia areata achieved at least 80 percent scalp hair coverage after 36 weeks of treatment, compared to roughly 5 percent of those on placebo.
Ritlecitinib showed comparable efficacy in its own trial program, with a meaningful proportion of patients reaching significant regrowth thresholds. To put this in perspective, before these approvals, dermatologists were limited to off-label treatments like corticosteroid injections, topical immunotherapy, or systemic immunosuppressants — none of which were specifically studied or approved for alopecia areata, and none of which had this level of clinical evidence behind them. The difference between injecting steroids into a patchy scalp every few weeks and taking a daily pill that addresses the underlying immune dysfunction is substantial for patient quality of life. It is worth noting that response rates vary considerably depending on disease severity and duration. Patients who had alopecia areata for a shorter period tended to respond better than those who had been living with total hair loss for many years. This makes early intervention an important consideration, though even long-standing cases showed improvement in a subset of patients.

What Are the Risks and Limitations of JAK Inhibitors for Hair Loss?
JAK inhibitors are not without serious considerations, and any patient evaluating these treatments needs to weigh the benefits against well-documented risks. The FDA approved these drugs with a boxed warning — the most serious category of safety alert — noting increased risks of major cardiovascular events, blood clots, cancer, and serious infections. These warnings stem partly from safety data on JAK inhibitors used in rheumatoid arthritis, particularly a large post-marketing study of tofacitinib (Xeljanz) that found elevated rates of heart attack, stroke, and malignancy in older patients with cardiovascular risk factors. Whether those same risks apply equally to the younger, generally healthier alopecia areata population remains an open question, but regulators decided the warnings were warranted. However, if a patient has pre-existing cardiovascular disease, a history of blood clots, or is a current or former smoker over age 50, the risk-benefit calculation shifts significantly.
Dermatologists generally conduct thorough screening before prescribing, including blood work to check cholesterol, blood counts, and liver function. Patients typically need ongoing monitoring with periodic lab tests throughout treatment. The other major limitation is that hair regrowth is not permanent if the drug is stopped — most patients who discontinue treatment see their hair loss return within months, meaning this is potentially a lifelong therapy commitment for those who respond. Common side effects during trials included upper respiratory infections, headaches, acne, elevated cholesterol, and urinary tract infections. Most of these were mild to moderate, but they add up over years of continuous use. For a condition that is medically benign — alopecia areata does not cause physical pain or organ damage — asking patients to accept even a small increase in serious health risks is a genuine ethical and clinical tension that physicians and patients must navigate together.
The Autoimmune Connection Between Alopecia Areata and Brain Health
The reason alopecia areata treatment breakthroughs deserve attention on a brain health platform goes beyond surface-level interest. Autoimmune conditions tend to cluster, and research has suggested that people with one autoimmune disorder face elevated risk for others, including conditions that affect the nervous system. Several epidemiological studies have found associations between autoimmune diseases and increased dementia risk, with chronic systemic inflammation being the likely connective thread. The same overactive immune signaling that destroys hair follicles in alopecia areata can, through different but related pathways, contribute to neuroinflammation that damages neurons over time. JAK-STAT signaling, the very pathway these new hair loss drugs target, has become a subject of active research in neurodegenerative disease.
Preclinical studies have examined whether JAK inhibitors might reduce neuroinflammation in models of Alzheimer’s disease, Parkinson’s disease, and multiple sclerosis. For instance, researchers have investigated whether blocking specific JAK pathways could reduce the production of pro-inflammatory cytokines in the brain’s microglia — the immune cells that, when chronically activated, are believed to accelerate cognitive decline. This research is still in early stages, and no JAK inhibitor is approved or recommended for any neurological indication, but the biological overlap is real and worth tracking. For caregivers and family members dealing with dementia, there is also a practical dimension. A loved one with dementia who also develops alopecia areata faces compounded distress — the visible hair loss can worsen confusion, agitation, and loss of identity that already accompany cognitive decline. Understanding that effective treatments now exist for the hair loss component can meaningfully improve quality of life and dignity for these patients, even when the dementia itself remains difficult to treat.

Comparing Treatment Options for Alopecia Areata Today
Patients and their physicians now face a decision landscape that, while still limited, is more varied than it was just a few years ago. The two FDA-approved JAK inhibitors — baricitinib and ritlecitinib — differ in their specificity. Baricitinib inhibits JAK1 and JAK2, while ritlecitinib targets JAK3 and the TEC family of kinases. In theory, ritlecitinib’s more selective mechanism could translate to a different side effect profile, potentially sparing some of the cardiovascular risks associated with broader JAK inhibition. However, head-to-head trials comparing the two drugs directly have not been published as of recent reports, so any comparison of efficacy and safety between them relies on cross-trial analysis, which is inherently imperfect. Beyond JAK inhibitors, older approaches remain in use and may be appropriate for milder cases. Corticosteroid injections directly into patchy areas of the scalp can stimulate regrowth in localized disease and have decades of clinical experience behind them.
Topical immunotherapy with agents like diphencyprone (DPCP) deliberately causes a mild allergic reaction on the scalp to redirect the immune system’s attention, and it works for some patients but requires regular clinic visits and can cause uncomfortable skin reactions. Systemic options like methotrexate or cyclosporine suppress the immune system more broadly and carry their own serious side effect profiles. The tradeoff is clear: JAK inhibitors offer the best evidence and most targeted mechanism, but they are also the most expensive option and require the most careful monitoring. Cost is a significant barrier that cannot be overlooked. JAK inhibitors for alopecia areata can carry list prices in the range of tens of thousands of dollars per year, and insurance coverage has been inconsistent. Some insurers classify alopecia areata as a cosmetic condition and deny coverage entirely, forcing patients into lengthy appeals processes. Manufacturer assistance programs exist but do not cover everyone. For many patients, especially older adults on fixed incomes or those managing the financial strain of dementia caregiving, the out-of-pocket cost may place these drugs out of reach regardless of their clinical promise.
What Happens When Treatment Is Stopped — and Who Should Be Cautious
One of the most important things patients need to understand before starting a JAK inhibitor for alopecia areata is what happens when they stop taking it. Clinical data has consistently shown that hair loss returns in the majority of patients after discontinuation, often within three to six months. This is not a treatment failure — it reflects the nature of alopecia areata as a chronic autoimmune condition that is being managed, not cured. But it means patients should go in with realistic expectations: if you respond well and want to keep your hair, you will likely need to stay on the medication indefinitely. This creates a particular concern for older adults and people with multiple comorbidities. The long-term safety profile of JAK inhibitors over decades of continuous use is not yet fully established, because the drugs have only been widely available for a few years.
The cardiovascular and malignancy warnings carry more weight for patients over 65 or those already managing conditions like hypertension, diabetes, or a history of cancer. A dermatologist prescribing a JAK inhibitor to a 70-year-old with alopecia areata and mild cognitive impairment faces a different calculation than one treating a 30-year-old with no other health issues. There is also the question of drug interactions and polypharmacy, which is especially relevant for the dementia care community. Patients with Alzheimer’s or other forms of dementia often take multiple medications — cholinesterase inhibitors, memantine, antidepressants, antipsychotics, blood pressure medications — and adding a JAK inhibitor to that mix requires careful pharmacological review. Baricitinib, for example, is cleared by the kidneys, and renal function declines with age. Dose adjustments may be necessary, and close coordination between dermatology and the patient’s primary care or neurology team is essential.
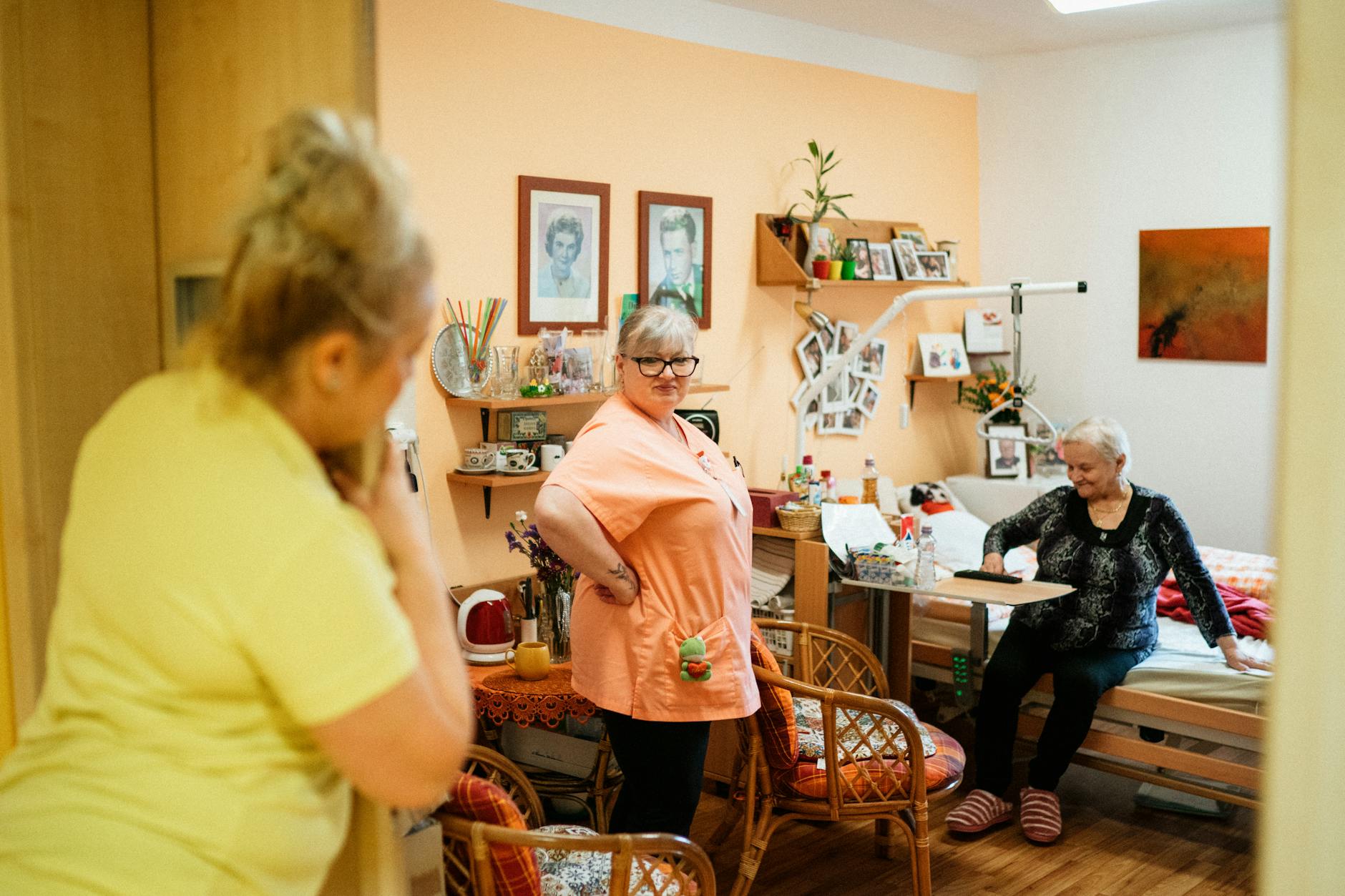
Emotional and Psychological Dimensions of Hair Loss in Aging and Dementia
The psychological impact of alopecia areata is well documented but often underestimated by those who have not experienced it. Studies have found rates of anxiety and depression among alopecia areata patients that rival those seen in other chronic diseases with significant physical symptoms. For older adults, hair loss intersects with existing anxieties about aging, attractiveness, and identity.
For a person in the early stages of dementia, who may already feel a frightening erosion of self, losing their hair on top of losing their memory can be devastating. One caregiver described her mother with moderate Alzheimer’s becoming inconsolable for weeks after her hair fell out, unable to understand why it was happening but deeply aware that something important had been taken from her. Having effective treatment options means that this dimension of suffering is no longer something families simply have to accept. Even if the decision is ultimately made not to pursue a JAK inhibitor due to safety concerns or cost, knowing that the option exists — and having a conversation about it with a physician — can itself be a form of care and respect for the patient’s dignity.
Where Research Goes From Here
The approval of JAK inhibitors for alopecia areata has opened a broader research frontier. Multiple pharmaceutical companies are investigating next-generation JAK inhibitors with even greater selectivity, aiming to preserve the hair regrowth benefits while minimizing systemic side effects. Topical JAK inhibitor formulations are also under development, which could potentially deliver the drug directly to the scalp and reduce exposure to the rest of the body — a meaningful advance if it proves effective, particularly for patients where systemic therapy carries too much risk.
Beyond alopecia, the success of targeting the JAK-STAT pathway in an autoimmune condition has energized research into whether similar approaches could help in neuroinflammatory diseases. While it would be irresponsible to suggest that a hair loss drug will treat Alzheimer’s disease, the underlying science of immune modulation is increasingly converging across medical specialties. For families navigating both autoimmune conditions and cognitive decline, staying informed about these developments is not just academically interesting — it may eventually influence treatment decisions that were not available even a year ago. As with all emerging therapies, the best approach is to maintain a relationship with knowledgeable physicians, ask questions, and resist the urge to either dismiss new treatments out of hand or embrace them without understanding the full picture.
Conclusion
The arrival of FDA-approved JAK inhibitors for alopecia areata represents a genuine medical advance — the first targeted, evidence-backed oral treatments for a condition that affects millions of people and has been inadequately served by medicine for decades. For the majority of patients who respond, these drugs can restore not just hair but a sense of normalcy and identity that hair loss quietly steals. The clinical data, while not perfect, is more robust than anything that came before it, and the pipeline of future treatments suggests the field will only improve from here. For those in the dementia care community, these developments carry added significance.
The autoimmune and neuroinflammatory connections between conditions like alopecia areata and cognitive decline make advances in one field potentially relevant to the other. On a more immediate level, having effective hair loss treatments available for elderly patients — including those with dementia — is a matter of preserving dignity and quality of life during an already difficult journey. As always, decisions about treatment should be made in close consultation with a medical team that understands the full picture of a patient’s health, and no one should start or stop a medication based solely on what they read online. But knowing what options exist is the first step toward making informed choices.
Frequently Asked Questions
Is alopecia areata the same as regular age-related hair thinning?
No. Alopecia areata is an autoimmune condition in which the immune system attacks hair follicles, typically causing distinct patches of complete hair loss or, in severe cases, total scalp or body hair loss. Age-related thinning, known as androgenetic alopecia, is driven by hormones and genetics and follows a gradual, diffuse pattern. The treatments discussed in this article — JAK inhibitors — are approved specifically for alopecia areata and are not indicated for common pattern baldness.
Can someone with dementia safely take a JAK inhibitor for hair loss?
There is no blanket answer. It depends on the individual’s overall health, other medications, kidney and liver function, and cardiovascular risk factors. The decision requires coordination between the prescribing dermatologist and the patient’s primary care physician or neurologist. Caregivers should advocate for a thorough risk-benefit discussion rather than assuming the treatment is either too dangerous or automatically appropriate.
How long does it take to see hair regrowth with these drugs?
In clinical trials, meaningful regrowth was typically observed between 12 and 36 weeks of treatment, though some patients took longer to respond. Not everyone responds, and the degree of regrowth varies. Patients with shorter disease duration and less extensive hair loss tended to respond faster and more completely.
Will insurance cover JAK inhibitors for alopecia areata?
Coverage varies widely. Some insurers cover these medications for alopecia areata, while others classify the condition as cosmetic and deny claims. Patients often need to go through prior authorization processes and may need to demonstrate that other treatments have failed first. Manufacturer patient assistance programs may help offset costs for those who qualify.
Does alopecia areata increase the risk of developing dementia?
Research into the connection between autoimmune conditions and dementia risk is ongoing. Some epidemiological studies have found modest associations between having autoimmune diseases and elevated dementia risk, potentially mediated by chronic inflammation. However, alopecia areata specifically has not been established as a direct risk factor for dementia, and more research is needed to understand these relationships.