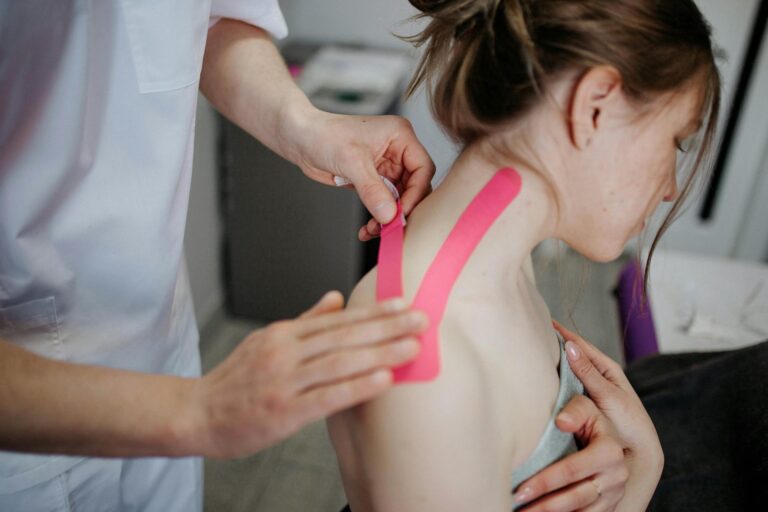
Recent meta-analyses examining acupuncture against conventional medication for chronic back pain have generally found that acupuncture performs comparably to, and in some cases modestly outperforms, standard pharmacological treatments for short-term pain relief — with significantly fewer side effects. For the millions of people living with persistent back pain, including older adults managing cognitive decline or dementia alongside musculoskeletal problems, this finding matters because it opens the door to a treatment option that avoids the sedation, confusion, and fall risk that many pain medications carry. Consider a 72-year-old with mild cognitive impairment who has been prescribed opioids or muscle relaxants for a herniated disc: the cognitive fog from those drugs can mimic or worsen dementia symptoms, making an alternative like acupuncture not just a preference but a clinical priority.
This article breaks down what the latest body of research suggests about acupuncture versus medication for chronic back pain, why the conversation is especially relevant for brain health, and where the evidence has real limits. We will look at which types of back pain respond best to acupuncture, what the risks and limitations are on both sides, how cognitive health intersects with pain management choices, and what practical steps someone might take when weighing these options. A note of transparency: meta-analytic data in this space evolves frequently, and some of the specific findings discussed here may have been updated since publication. Where uncertainty exists, we will say so plainly.
Table of Contents
- What Does the Meta-Analytic Evidence Actually Show About Acupuncture vs. Medication for Back Pain?
- Why Chronic Back Pain Treatment Choices Carry Extra Weight for Brain Health
- Which Types of Chronic Back Pain Respond Best to Acupuncture?
- Practical Steps for Choosing Between Acupuncture and Medication
- Limitations of the Evidence and What Can Go Wrong
- Insurance, Cost, and Access Barriers
- Where This Field Is Headed
- Conclusion
- Frequently Asked Questions
What Does the Meta-Analytic Evidence Actually Show About Acupuncture vs. Medication for Back Pain?
Meta-analyses pool results from multiple randomized controlled trials to reach broader conclusions, and several published in recent years have examined acupuncture head-to-head with pharmacological treatments for chronic low back pain. The general pattern across these analyses has been that acupuncture produces statistically significant reductions in pain intensity compared to no treatment and performs at least as well as NSAIDs, muscle relaxants, and in some comparisons, opioid-based regimens over periods of four to twelve weeks. Some analyses have reported a modest edge for acupuncture in function and disability scores, though the effect sizes tend to be small to moderate — meaningful to patients, but not dramatic in statistical terms. However, the quality of the underlying trials varies considerably.
Many studies originate from clinical settings where blinding is difficult — you cannot easily give someone a convincing placebo acupuncture session — and this introduces bias that reviewers consistently flag. Sham acupuncture controls, where needles are inserted at non-traditional points or at shallow depths, often produce effects that are closer to real acupuncture than to no treatment at all, which complicates interpretation. What the evidence supports with reasonable confidence is that acupuncture is a legitimate option in the treatment toolkit, not that it is categorically superior to medication. The distinction matters for anyone making real clinical decisions.

Why Chronic Back Pain Treatment Choices Carry Extra Weight for Brain Health
For people with dementia, mild cognitive impairment, or those at elevated risk for cognitive decline, the choice between acupuncture and medication is not purely about the back. Many first-line medications for chronic pain have direct cognitive consequences. Opioids cause sedation and confusion. Benzodiazepines, sometimes prescribed as muscle relaxants, are associated with increased dementia risk in epidemiological studies, though causation remains debated. Even over-the-counter NSAIDs, when used chronically, carry risks of gastrointestinal bleeding and kidney damage that complicate care in older adults already managing multiple prescriptions.
Acupuncture sidesteps these pharmacological burdens almost entirely. Its most commonly reported side effects — minor bruising, temporary soreness at needle sites, occasional lightheadedness — are localized and transient. For a caregiver managing a parent with Alzheimer’s disease who also has chronic lumbar pain, reducing the medication load by even one sedating drug can translate to better daytime alertness, fewer falls, and a clearer picture of how the dementia itself is progressing versus what is drug-induced fog. That said, acupuncture is not risk-free for this population. Patients with advanced dementia may not be able to communicate pain, hold still during sessions, or consent meaningfully — all practical barriers that clinicians and families need to weigh honestly.
Which Types of Chronic Back Pain Respond Best to Acupuncture?
Not all back pain is the same, and the meta-analytic literature does not treat it as such. Nonspecific chronic low back pain — the kind where imaging does not reveal a clear structural cause like a fracture, tumor, or severe stenosis — is the category where acupuncture has the strongest evidence base. This happens to be the most common form, accounting for an estimated 85 to 90 percent of chronic back pain cases. For someone whose MRI shows mild degenerative changes that do not fully explain their level of pain, acupuncture has reasonable evidence behind it.
The picture changes for radiculopathy, where a compressed nerve root sends shooting pain down the leg, or for pain following spinal surgery. In these cases, the evidence for acupuncture is thinner and less consistent. A person recovering from a lumbar fusion who tries acupuncture may find some relief from the muscular tension surrounding the surgical site, but should not expect it to address nerve-related symptoms in the same way a targeted nerve block or gabapentinoid medication might. The American College of Physicians has included acupuncture among recommended nonpharmacological therapies for chronic low back pain in its clinical guidelines, but this recommendation applies primarily to the nonspecific category. Knowing which kind of back pain you are dealing with is essential before choosing a treatment path.
Practical Steps for Choosing Between Acupuncture and Medication
The decision between these approaches does not have to be binary, and for most people, it should not be. Integrative treatment plans that combine acupuncture with judicious short-term medication use, physical therapy, and movement-based strategies tend to produce better outcomes than any single intervention alone. The practical question is usually not “acupuncture or medication” but rather “how much of each, and in what sequence.” A reasonable starting framework, particularly for older adults or those with cognitive health concerns, is to trial acupuncture first for nonspecific chronic low back pain, typically over six to twelve sessions spanning several weeks.
If meaningful improvement occurs — reduced pain scores, better sleep, improved ability to participate in daily activities — then the argument for avoiding or reducing medication becomes straightforward. If acupuncture alone is insufficient, layering in a short course of NSAIDs or acetaminophen as a bridge while continuing sessions is a common clinical approach. The tradeoff to understand clearly is that acupuncture requires more time, more appointments, and more out-of-pocket cost in many insurance environments, while medication offers faster onset but ongoing exposure to side effects. For someone whose primary concern is protecting cognitive function, the extra logistical effort of acupuncture may be well worth it.
Limitations of the Evidence and What Can Go Wrong
It would be irresponsible to discuss this topic without being direct about where the evidence falls short. The most significant limitation in acupuncture research is the difficulty of blinding, as mentioned earlier. When patients know they are receiving acupuncture — and they usually do — expectation effects can inflate the apparent benefit. This does not mean the benefit is imaginary, but it does mean the true pharmacological-style effect of needling specific points is harder to isolate than proponents sometimes suggest. There are also quality-of-practice concerns.
Acupuncture administered by a well-trained licensed practitioner in a clinical setting is a different experience from what is offered in some wellness spas or by practitioners with minimal training. Adverse events, while rare, are not zero: there have been documented cases of pneumothorax from needles inserted too deeply near the chest, and infections from improperly sterilized equipment. For patients on blood thinners — common in the older adult population — even routine needling carries a somewhat elevated bleeding risk. Additionally, the research base skews heavily toward short-term outcomes measured at four to twelve weeks. Long-term data on whether acupuncture produces sustained benefit for chronic back pain beyond six months is limited and inconsistent. Anyone beginning acupuncture should do so with realistic expectations about what it can and cannot deliver over time.

Insurance, Cost, and Access Barriers
One of the most common real-world obstacles to choosing acupuncture is cost. While coverage has expanded in recent years — Medicare, for instance, began covering acupuncture for chronic low back pain in 2020 in the United States, though with specific visit limits and provider requirements — many insurance plans still offer limited or no reimbursement. A typical session ranges historically from $75 to $150 out of pocket, and a standard initial course involves eight to twelve sessions.
By comparison, a month of generic naproxen costs a few dollars. For a family already bearing the financial weight of dementia caregiving, this cost differential can be decisive regardless of what the clinical evidence says. It is worth checking current coverage specifics with your insurer, as this landscape changes frequently.
Where This Field Is Headed
Research into acupuncture for pain management is evolving in several promising directions. Electroacupuncture, which adds mild electrical stimulation to the needles, is being studied with more rigorous trial designs and may offer more standardized dosing than traditional manual acupuncture. Neuroimaging studies are beginning to map how acupuncture modulates pain processing in the brain, which is directly relevant to understanding its potential interactions with neurodegenerative conditions.
There is also growing interest in whether acupuncture’s effects on inflammatory markers could have neuroprotective implications, though this remains speculative and early-stage. For the dementia care community specifically, the larger shift toward deprescribing — systematically reducing unnecessary medications in older adults — creates a natural opening for nonpharmacological pain treatments. As more health systems invest in integrative medicine programs, access to acupuncture within conventional clinical settings is likely to improve. The evidence is unlikely to ever show acupuncture as a miracle cure for chronic back pain, but its role as a safe, modestly effective complement to a broader pain management strategy appears increasingly secure.
Conclusion
The meta-analytic evidence to date supports acupuncture as a viable and generally safe alternative or complement to medication for chronic nonspecific low back pain. Its most compelling advantage is not necessarily superior pain relief but rather the absence of the cognitive side effects, dependency risks, and organ damage associated with long-term pharmacological use — a consideration that carries outsized importance for people managing brain health conditions alongside chronic pain.
The practical path forward for most people is not choosing one over the other in absolute terms but assembling a treatment approach that reflects their specific diagnosis, cognitive health status, financial situation, and access to qualified practitioners. Discussing acupuncture explicitly with a primary care provider or pain specialist is a reasonable first step, particularly for older adults or those caring for someone with dementia. The goal is not to find a single perfect intervention but to reduce pain while preserving as much cognitive clarity and quality of life as possible.
Frequently Asked Questions
Is acupuncture safe for someone with dementia?
Generally yes, though practical challenges exist. Patients with advanced dementia may have difficulty holding still, communicating discomfort during treatment, or providing informed consent. A caregiver or legal health proxy should be involved in the decision-making, and sessions should be conducted by a practitioner experienced with older or cognitively impaired patients.
How many acupuncture sessions are typically needed for chronic back pain?
Most clinical trials and practice guidelines suggest an initial course of eight to twelve sessions over six to eight weeks to assess response. Some patients notice improvement within three to four sessions, while others require the full course before meaningful changes occur. Maintenance sessions at longer intervals may be recommended if the initial course is effective.
Can acupuncture replace pain medication entirely?
For some people with mild to moderate nonspecific chronic low back pain, yes — acupuncture alone may provide sufficient relief. For others, particularly those with severe pain, radiculopathy, or post-surgical pain, it is more realistic to view acupuncture as one component of a multimodal plan that may still include some medication use.
Does Medicare cover acupuncture for back pain?
As of 2020, Medicare began covering acupuncture specifically for chronic low back pain under certain conditions, including visit limits and approved provider requirements. Coverage details may have changed since then, so verifying current benefits with Medicare or a supplemental insurer directly is advisable.
Are there any medications for back pain that are especially problematic for brain health?
Opioids, benzodiazepines, and anticholinergic muscle relaxants like cyclobenzaprine are among the most cognitively problematic options. They can cause sedation, confusion, increased fall risk, and in the case of benzodiazepines, have been epidemiologically linked to increased dementia risk with long-term use. These are often flagged on the Beers Criteria list of potentially inappropriate medications for older adults.