Rest alone does not heal disc injuries because the discs in your spine cannot repair themselves through immobility—they actually depend on movement and loading to maintain their blood supply and nutrient delivery. When you remain completely sedentary after a disc injury, the damaged tissue starves of the oxygen and nutrients it needs to regenerate, and the surrounding muscles that stabilize your spine begin to atrophy, leaving you weaker and more vulnerable to re-injury. For example, someone with a herniated lumbar disc who spends two weeks lying flat may find their pain decreases temporarily due to reduced pressure on the nerve, but without gradual movement and targeted rehabilitation, the underlying disc damage worsens and the supporting structures deteriorate. This article explores why motion and rehabilitation are essential components of disc healing, what the research actually shows about recovery timelines, and how to progress from acute pain management to genuine tissue repair.
Table of Contents
- How Do Spinal Discs Actually Heal Without a Blood Supply?
- The Inflammation Problem—Why Too Much Rest Backfires
- Muscle Atrophy and Spinal Instability—The Secondary Problem
- Progressive Loading and Rehabilitation—What Actually Promotes Healing
- The Risk of Chronic Pain and Maladaptive Movement Patterns
- How Posture, Ergonomics, and Lifestyle Factors Support Disc Healing
- Recovery Timeline and Managing Expectations
- Conclusion
- Frequently Asked Questions
How Do Spinal Discs Actually Heal Without a Blood Supply?
Spinal discs are avascular structures—they have no direct blood vessels once you reach adulthood. Instead, they receive oxygen and nutrients through a diffusion process called imbibition, where fluids move into the disc when you move and compress it, and nutrients are drawn in like water being absorbed into a sponge. Complete bed rest interrupts this process because the disc receives minimal loading and fluid movement, essentially cutting off its supply line. Research published in the journal Spine shows that discs in immobilized segments undergo accelerated degeneration and lose structural integrity faster than discs subjected to appropriate movement and loading.
When a disc herniates or bulges, the injury to the annulus (the tough outer layer) and nucleus (the gel-like center) does have some potential for repair, but only if conditions support it. The body’s inflammatory response in the first few weeks is actually a necessary part of healing—it brings immune cells and growth factors to the area. However, prolonged inflammation combined with immobility shifts the balance away from repair and toward fibrosis and degeneration. Gentle, progressive loading helps resolve inflammation and promotes the reabsorption of disc material that has extruded into the spinal canal.

The Inflammation Problem—Why Too Much Rest Backfires
Acute inflammation after a disc injury is helpful and necessary, but it should resolve over weeks to months, not persist indefinitely. When people rest completely, they often experience pain relief initially because they’re not aggravating the injured area, but this creates a false sense of healing. The inflammatory cytokines and swelling around the nerve root remain elevated because the mechanical conditions that would normally promote their clearance—gentle loading, muscular stabilization, and fluid exchange—never occur.
Studies tracking disc herniations with MRI over time reveal a critical finding: discs in completely immobilized or sedentary patients show slower reabsorption of extruded material and higher rates of persistent inflammation compared to patients who engage in supervised movement. However, the key caveat is that movement must be graduated and appropriate to the stage of injury—too much aggressive activity too soon can re-traumatize the healing tissue and restart the inflammatory cascade. The goal is to find the threshold between “move enough to promote healing” and “don’t move so much that you re-injure yourself.”.
Muscle Atrophy and Spinal Instability—The Secondary Problem
Even if your disc were somehow healing in isolation during bed rest—which it isn’t—your supporting muscles would be deteriorating. The erector spinae, multifidus, and core muscles that normally stabilize your spine atrophy rapidly during immobility, with measurable loss of muscle mass occurring within two to three weeks. This atrophy is particularly pronounced in the deep stabilizer muscles that most directly protect the spine, and these are the hardest to recover.
Once you do return to activity, your spine is now supported by weaker muscles, which means the healing disc faces greater shear forces and mechanical stress than it did before the injury. A patient who rested for six weeks and then suddenly returned to normal activities is essentially re-injuring a partially healed disc with an unstable, deconditioned supporting structure. Physical therapy and progressive rehabilitation specifically target rebuilding these muscles in a controlled manner, restoring the mechanical support the disc needs to tolerate normal activities. Without this muscular rebuilding, many people experience recurrent disc injuries within months of their initial injury.
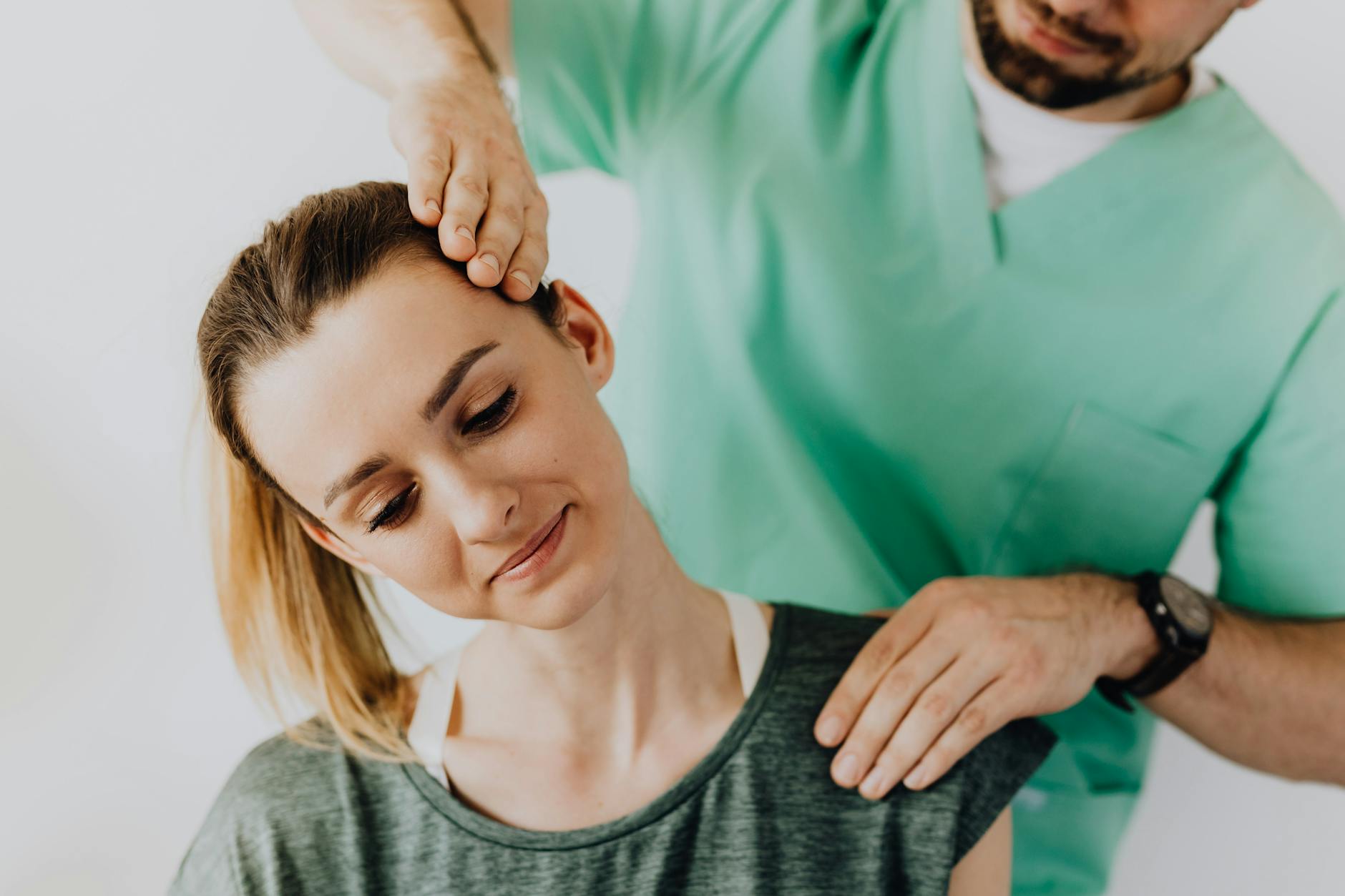
Progressive Loading and Rehabilitation—What Actually Promotes Healing
The evidence-based approach to disc injury recovery involves a phased rehabilitation program that progresses from pain management and gentle mobility in the acute phase to gradual strengthening and functional training as healing progresses. In the first one to two weeks after acute injury, relative rest (not absolute bed rest) is appropriate—this means avoiding activities that sharply worsen pain while maintaining gentle movement like walking and basic stretches that keep the disc mobile. By week two to three, if pain is manageable, most people benefit from beginning controlled exercises that activate the stabilizing muscles without excessive spinal loading.
These might include bird-dog exercises, dead bugs, gentle isometric core holds, and controlled walking. As weeks progress and pain improves, resistance is gradually added through exercises like quadruped limb raises, bridges, and eventually functional movements like squats and lunges done with proper form. This progression isn’t arbitrary—it follows the tissue healing timeline and gives muscles time to regain strength while the disc is simultaneously being nourished through movement and loaded in ways that promote repair rather than further damage.
The Risk of Chronic Pain and Maladaptive Movement Patterns
One of the most underappreciated consequences of extended bed rest is the development of central sensitization and maladaptive movement patterns. Chronic pain can involve changes in how your nervous system processes pain signals, and prolonged inactivity combined with fear of movement can lock in these patterns. People who rest for weeks often develop a strong fear-avoidance relationship with movement—they believe their spine is fragile, so they guard against any activity that might stress it, which perpetuates weakness and fear.
A critical limitation of the “rest heals” model is that it ignores the psychological and neurological dimensions of recovery. Rehabilitation programs that include graded exposure to movement, education about how discs actually heal, and progressive confidence-building through successful activity tolerance have much better long-term outcomes than rest-based approaches. However, this doesn’t mean you should ignore pain signals entirely—sharp, acute pain is a warning that you’ve exceeded your current capacity. The distinction is between protective pain that guides you toward appropriate activity levels and chronic pain that keeps you locked in avoidance patterns.

How Posture, Ergonomics, and Lifestyle Factors Support Disc Healing
While rehabilitation is essential, the environment you move in matters too. Poor ergonomics, prolonged sitting, and repetitive heavy lifting that contributed to the disc injury in the first place will continue to stress the healing tissue if they aren’t addressed. Someone whose disc herniated because they spent eight hours a day hunched over a desk will not fully recover just by doing exercises three times a week—the other 165 hours of the week spent in poor posture will continue to stress the disc.
Effective recovery requires integrating postural awareness and ergonomic modifications into daily life. This might mean adjusting your chair height, taking regular standing breaks, using proper lifting mechanics when handling heavy objects, or modifying your sleep position to reduce nighttime stress on the disc. These changes don’t directly heal the disc, but they reduce the ongoing irritation that prevents healing and support the gains made through rehabilitation.
Recovery Timeline and Managing Expectations
Most uncomplicated disc injuries take three to six months for the acute inflammation to fully resolve and the disc tissue to stabilize, assuming appropriate rehabilitation is followed. Complete pain resolution often takes longer—sometimes nine to twelve months for full functional recovery. The timeline varies significantly based on the severity of the initial injury, your age, the specific location of the disc, and your compliance with rehabilitation.
Understanding this timeline is important because it sets realistic expectations and prevents the common trap of returning to full activity too quickly once pain improves. Pain improvement and tissue healing don’t always align; you might feel significantly better at eight weeks while the disc is still vulnerable to re-injury. This is why rehabilitation progression is tied to specific movement milestones and functional capacity rather than just pain levels. As you return to higher-intensity activities, the underlying disc stability and muscular support must be adequate to prevent re-injury.
Conclusion
Rest alone does not heal disc injuries because the spine’s discs depend on movement and appropriate loading for nutrient delivery and repair, because supporting muscles will atrophy during immobility, and because prolonged inactivity can entrench chronic pain patterns. The scientific evidence consistently shows that graded, progressive rehabilitation produces better long-term outcomes than extended bed rest. While initial relative rest is appropriate for acute pain management, moving too quickly from rest to unrestricted activity is equally problematic because it re-injures a partially healed disc with weakened muscular support.
The path to genuine disc healing involves understanding that recovery requires active participation—progressive exercises, postural awareness, and appropriate pacing over weeks and months. If you’re dealing with a disc injury, work with a healthcare provider or physical therapist to develop a rehabilitation plan suited to your specific injury stage and severity. The goal is not to return to pain-free activity as quickly as possible, but to rebuild the structural and muscular support that allows your spine to tolerate normal demands over the long term.
Frequently Asked Questions
Can I do any exercise with a disc injury, or should I avoid movement completely?
Movement is necessary for healing, but it must be graduated to your injury stage. In the acute phase (first 1-2 weeks), light walking and gentle stretching are appropriate. As pain improves, controlled exercises targeting stabilization muscles are gradually introduced. Avoid high-impact activities, heavy loading, and movements that sharply increase your pain—but gentle, pain-controlled movement is beneficial from the early stages of recovery.
How long before I can return to my normal activities after a disc injury?
Most people see significant pain improvement within 4-6 weeks, but structural healing takes longer. Returning to normal activities typically requires 3-6 months of consistent rehabilitation. The specific timeline depends on injury severity and how well you follow rehabilitation. Returning too early risks re-injury; returning too late risks perpetuating weakness and fear-avoidance patterns.
Does bed rest ever help with disc injuries, or is it always counterproductive?
Brief relative rest in the first 1-2 weeks can help manage acute pain, but prolonged bed rest is counterproductive for healing. Complete immobility for more than a week or two typically worsens outcomes by accelerating muscle atrophy and slowing the healing process. The focus should shift quickly from rest to graded movement and rehabilitation.
Why do I feel better when I rest, but then pain returns when I try to move?
Rest reduces pain by decreasing mechanical stress on the injured tissue, but it doesn’t heal the underlying injury. When you return to activity, your muscles are weaker, the supporting structures have atrophied, and the disc is still vulnerable. This is why rehabilitation that rebuilds strength and stability is essential—it allows you to tolerate activity without pain returning.
Can imaging (MRI or X-ray) tell me when my disc is healed?
Structural changes on imaging heal much more slowly than functional recovery. You may feel capable of normal activity long before imaging shows complete resolution of the disc bulge or herniation. The disc material may take months to fully reabsorb, but functional healing—the point at which your spine can tolerate normal demands—often comes sooner. Focus on functional milestones (returning to specific activities without pain) rather than waiting for imaging to look “normal.”
Should I wear a brace or support belt during recovery?
Braces can provide pain relief and reduce anxiety in the acute phase, but prolonged bracing can weaken stabilizing muscles further and delay recovery. Short-term bracing (1-2 weeks) may be helpful during the most painful period, but your goal should be transitioning to rehabilitation that builds natural support through muscle strengthening. Check with your physical therapist about when to reduce or discontinue bracing.





