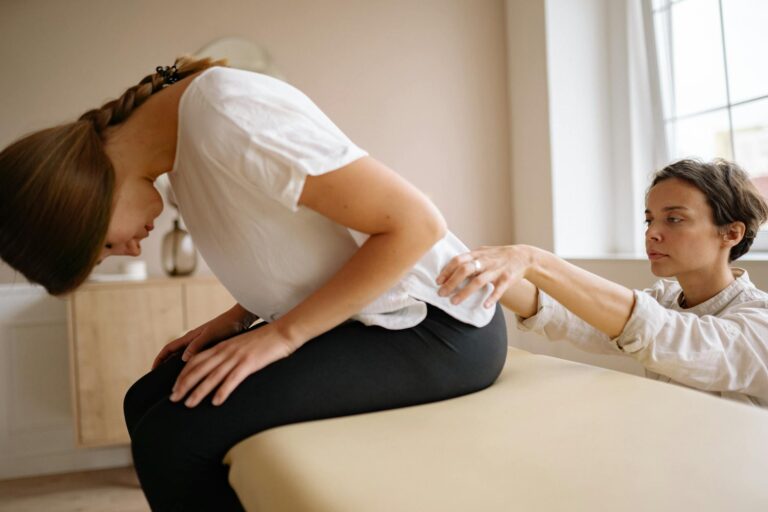
When doctors evaluate lumbar spine stress—the medical term for lower back pain and related conditions—they consistently identify ten primary causes that account for the vast majority of patient diagnoses. The most common culprit is muscle strain and ligament sprains, which alone responsible for approximately 97% of back pain complications in the general adult population. These mechanical issues are followed by structural problems like intervertebral disc degeneration, herniated discs, and age-related degenerative changes. For example, a 55-year-old office worker might develop lumbar spine stress from a combination of muscle strain during a poorly executed lifting movement, coupled with years of sedentary work and the natural disc degeneration that accelerates after age 50. Understanding these ten causes—and how they interact with individual risk factors—helps patients and their healthcare providers develop more effective treatment strategies rather than defaulting to generic pain management.
This article examines each of these diagnoses, the research behind them, and why certain causes are far more prevalent than others. The scale of lumbar spine stress globally is substantial: 619 million people currently live with low back pain worldwide, and the World Health Organization projects this number will rise to 843 million by 2050. In the United States alone, 39% of adults have experienced back pain in recent years. The condition is the leading cause of disability globally since 1990, yet 90% of cases are classified as “non-specific”—meaning doctors cannot pinpoint a single structural diagnosis without additional red flags. This reality underscores an important fact: most lumbar spine stress is mechanical and treatable, but requires understanding the underlying cause to address it effectively.
Table of Contents
- Why Muscle Strain and Ligament Sprains Dominate Back Pain Diagnoses
- Intervertebral Disc Degeneration and Its Progressive Nature
- Herniated and Prolapsed Discs and Their Variable Impact
- Age-Related Changes and the Acceleration of Lumbar Stress After 50
- Modifiable Risk Factors—Obesity, Smoking, and Inactivity
- Occupational Stress and Workplace-Related Lumbar Spine Conditions
- Psychological Stress, Depression, and the Mind-Body Connection in Lumbar Pain
- Degenerative Conditions—Osteoarthrosis and Spondylosis
- Conclusion
Why Muscle Strain and Ligament Sprains Dominate Back Pain Diagnoses
Muscle strain and ligament sprains represent the most frequently diagnosed cause of lumbar spine stress, accounting for nearly all back pain complications seen in primary care and orthopedic settings. These injuries are classified as mechanical, and they comprise approximately 90% of all back pain cases—a significantly higher prevalence than more dramatic-sounding conditions like herniated discs or degenerative joint disease. A muscle strain occurs when muscle fibers tear due to overuse, sudden movement, or improper lifting technique, while ligament sprains involve the connective tissue that stabilizes the spine. The key distinction is that these injuries are typically self-limiting; the body’s natural healing process resolves them over weeks to months without surgical intervention. The reason these diagnoses are so common is partly anatomical and partly circumstantial.
The lumbar spine bears most of the body’s weight during standing and sitting, and the muscles surrounding it are among the most frequently used in daily movement. A person might strain their lower back muscles reaching for something awkwardly, lifting a heavy object with poor form, or even sleeping in an uncomfortable position. Unlike disc herniation, which requires significant force or underlying degeneration, muscle strain can occur from relatively minor trauma. This accessibility—the fact that nearly anyone can strain their back—explains the 97% prevalence figure. However, the downside is that muscle strains can recur if the underlying weakness or movement pattern isn’t addressed, leading to chronic intermittent back pain that frustrates both patients and their doctors.
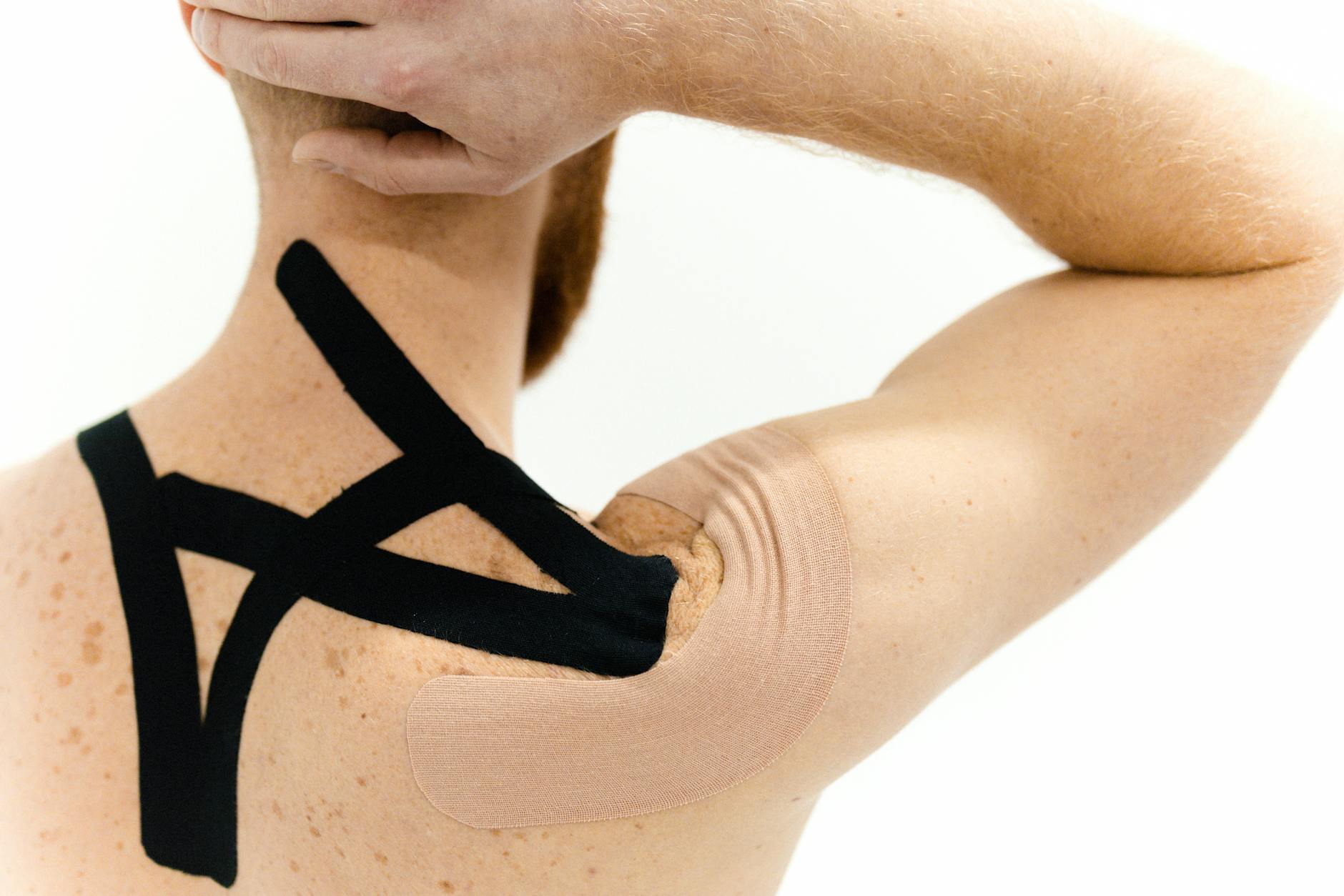
Intervertebral Disc Degeneration and Its Progressive Nature
Intervertebral disc degeneration represents one of the most common structural changes affecting the lumbar spine, and it occurs through a combination of biochemical, mechanical, and inflammatory processes. The discs between vertebrae contain a gel-like nucleus surrounded by a tough fibrous outer ring. Over time—especially in people over 50—this disc material breaks down through a process called extracellular matrix degradation, and inflammatory mediators increase within the disc space. This isn’t a sudden failure; it’s a gradual deterioration that can take place over decades. Research from Nature shows that disc degeneration involves complex interactions between mechanical stress, chemical breakdown, and inflammation, making it particularly difficult to reverse once significantly advanced.
The practical reality of disc degeneration is that it often produces no symptoms at all. Many imaging studies find degenerative discs in people with no back pain whatsoever, which means doctors must be careful not to over-diagnose or over-treat this condition. However, when degeneration progresses far enough, it can narrow the spaces where spinal nerves exit, leading to radiating pain down the leg—a condition called sciatica. Additionally, degenerated discs lose height and stability, which increases stress on surrounding muscles and ligaments. The challenge with disc degeneration is that while we can slow it through activity, weight management, and smoking cessation, we cannot currently reverse the damage once it has occurred. This means that early intervention to prevent or delay degeneration—through lifestyle measures—is more effective than trying to treat advanced cases.
Herniated and Prolapsed Discs and Their Variable Impact
Herniated discs occur when the outer ring of an intervertebral disc tears and allows the inner gel material to protrude into the spinal canal, potentially pressing on nerves. A prolapsed disc is similar, with the disc material bulging backward into the space where the spinal cord and nerve roots reside. Despite the dramatic nature of these diagnoses and the concerning images that MRI produces, it’s important to understand that herniated discs account for less than 5% of all back pain problems in the general population. Many herniated discs cause no pain at all—imaging studies frequently incidental find them in people without any symptoms. Others cause significant pain and neurological symptoms like numbness, weakness, or tingling that radiates into the buttocks and down the leg.
The variable impact of herniated discs depends on several factors: the size of the herniation, its exact location, the age of the patient, and the underlying degenerative state of the disc. A young person with a large herniation that doesn’t compress a nerve may have no symptoms, while an older person with a smaller disc bulge might experience significant nerve compression and pain. This unpredictability means that imaging findings alone shouldn’t drive treatment decisions. Most herniated discs improve over time with conservative treatment—physical therapy, activity modification, and sometimes anti-inflammatory medications—without requiring surgery. Only when herniation causes progressive neurological deficits or incapacitating pain should surgery be considered. The limitation here is that while some herniated discs resolve spontaneously as the body reabsorbs the protruding material, others remain stable but symptomatic, requiring long-term management strategies.

Age-Related Changes and the Acceleration of Lumbar Stress After 50
Age represents one of the most significant predictors of lumbar spine stress, with prevalence increasing dramatically across the lifespan. According to CDC data, back pain affects 28.4% of adults ages 18-29, but this rises to 45.6% in adults over 65—a 60% increase. The peak incidence appears to occur around ages 50-55, where multiple degenerative changes accelerate simultaneously: discs lose water content and height, ligaments stiffen, muscles become weaker if not actively maintained, and bone density decreases. This convergence of changes explains why many people experience their first significant back pain episode in their fifth or sixth decade. The mechanisms behind age-related lumbar stress are both structural and functional.
Structurally, cumulative wear-and-tear on the spine creates the conditions for osteoarthritis, disc degeneration, and reduced spinal stability. Functionally, aging brings reduced muscle mass (sarcopenia), decreased flexibility, and slower healing capacity. A 60-year-old who strains their back will take longer to recover than a 30-year-old with the same injury. The comparison is important: while young people typically experience acute muscle strains that resolve quickly, older adults are more likely to develop chronic intermittent pain due to underlying degenerative changes that make their spine more vulnerable. The silver lining is that age-related changes are not inevitable; research consistently shows that older adults who remain physically active and maintain muscle strength have significantly less lumbar spine stress than sedentary peers of the same age.
Modifiable Risk Factors—Obesity, Smoking, and Inactivity
Obesity, smoking, and physical inactivity collectively contribute to lumbar spine stress through multiple mechanisms and represent the modifiable risk factors with the greatest impact on prevention and treatment. Obesity increases stress on the lumbar spine because additional body weight places greater mechanical load on the discs and facet joints, particularly in the lower back. Smoking affects spinal health by reducing blood flow to the discs (impairing nutrition and waste removal), diminishing healing capacity, and potentially increasing inflammation throughout the body. Physical inactivity contributes through deconditioning of the core muscles that stabilize the spine, leading to excessive motion and stress on discs and ligaments. These three factors are particularly important because they’re within a patient’s control, unlike age or genetic predisposition.
A person who loses weight, quits smoking, and begins regular exercise—particularly activities that strengthen core stability and maintain flexibility—can significantly reduce their lumbar spine stress even if they have underlying degenerative changes. The tradeoff, however, is that lifestyle change requires sustained effort and motivation. A person might improve their back pain through three months of consistent exercise, only to regress if they become sedentary again. This pattern of improvement and regression is common in back pain management and highlights why doctors emphasize lifestyle factors as foundational interventions. The WHO guidelines on low back pain consistently recommend non-surgical management approaches including activity, exercise, and cognitive behavioral therapy before resorting to more intensive interventions.

Occupational Stress and Workplace-Related Lumbar Spine Conditions
Occupational factors significantly influence lumbar spine stress, with heavy lifting and repetitive movements representing the primary workplace contributors to back pain and structural damage. Jobs involving sustained awkward postures, vibration exposure, or frequent overhead reaching place considerable stress on the lower back. Construction workers, nurses, warehouse workers, and others in physically demanding roles face elevated risk, but office workers are not exempt—prolonged sitting with poor ergonomics creates its own form of occupational stress through sustained compression of the discs and passive stretching of ligaments. The important nuance is that not all occupational stress results from the job itself.
A warehouse worker with strong core muscles and good lifting technique may experience less back pain than an office worker with weak abdominal muscles and poor posture. This means that while job modification and ergonomic improvements are important, they’re most effective when combined with personal fitness and body mechanics training. A specific example: someone whose job requires lifting should not only ensure their employer provides proper lifting equipment and techniques training, but should also maintain core strength through targeted exercise. The limitation is that some occupations inherently impose more spinal stress than others, and even with perfect technique, cumulative microtrauma can eventually lead to degenerative changes. This reality underscores why occupational health and worker protections remain important public health considerations.
Psychological Stress, Depression, and the Mind-Body Connection in Lumbar Pain
Psychological stress and depression significantly influence the development and persistence of lumbar spine stress, a relationship that many patients find surprising until it’s explained. The WHO 2023 guidelines on chronic low back pain specifically identify psychological factors as critical both in disease development and in treatment outcomes. Depression and anxiety lower pain thresholds, meaning people experiencing these conditions perceive the same level of physical stimulus as more painful than those in better mental health. Additionally, stress triggers muscle tension and changes in movement patterns that can perpetuate or worsen mechanical back problems.
The clinical implication is profound: a person with significant mechanical lumbar spine stress may not improve with physical therapy alone if underlying depression or anxiety remains unaddressed. The WHO guidelines recommend cognitive behavioral therapy (CBT) as an evidence-based intervention for chronic low back pain, recognizing that psychological treatment can be as important as physical treatment. An example: a patient recovering from a disc herniation might do their physical therapy exercises perfectly, but if they’re also experiencing depression that reduces their motivation and increases catastrophizing about their pain, their recovery will be slower and more incomplete. The bidirectional relationship also works in reverse—chronic back pain can itself trigger depression and anxiety, creating a cycle that’s difficult to break without comprehensive treatment addressing both the physical and psychological dimensions.
Degenerative Conditions—Osteoarthrosis and Spondylosis
Osteoarthrosis and spondylosis represent degenerative changes of the spine that become increasingly common with age and represent specific structural diagnoses visible on imaging. Osteoarthrosis, or facet joint arthritis, involves the small joints between vertebrae, while spondylosis refers more broadly to degenerative changes and bone spurs (osteophytes) that develop as the body attempts to stabilize an increasingly mobile or damaged segment. These conditions often coexist with disc degeneration, creating a pattern of multilevel spinal damage that accumulates over decades. The importance of recognizing osteoarthrosis and spondylosis is that they require different management approaches than acute muscle strains.
Someone with facet joint arthritis may find that certain movements—particularly extension and rotation—provoke pain more than others, whereas someone with disc degeneration may have symptoms worse with flexion. Physical therapists can tailor exercises to avoid provocative movements while strengthening supporting muscles. Additionally, patients should understand that these degenerative diagnoses, while concerning-sounding, are often compatible with functional and pain-free living. Many people with significant osteoarthritis on imaging have no symptoms whatsoever. The key is managing the condition proactively through exercise, weight management, and activity modification rather than accepting the diagnosis as a progressive disability.
Conclusion
The ten causes of lumbar spine stress that doctors diagnose most frequently—muscle strain, disc degeneration, herniation, age-related changes, obesity, smoking, inactivity, occupational stress, psychological factors, and osteoarthrosis—represent a complex web of mechanical, structural, and systemic factors. Understanding that muscle strain and ligament injuries account for 97% of cases should be reassuring; most back pain is not due to dramatic structural failure, but rather to mechanical problems that the body can often resolve with appropriate management. The fact that 619 million people globally live with low back pain, with projections rising to 843 million by 2050, underscores that lumbar spine stress is a pandemic of modern living—driven partly by aging populations and partly by lifestyle factors like sedentary behavior, obesity, and smoking.
The pathway forward for individuals experiencing lumbar spine stress involves first establishing an accurate diagnosis (which is challenging given the high proportion of non-specific cases), then implementing a comprehensive approach targeting modifiable risk factors. This means maintaining physical activity and core strength, managing weight, avoiding smoking, addressing psychological factors like depression and anxiety, and ensuring proper ergonomics at work and home. For most people, this conservative approach—supported by current WHO guidelines—produces the best long-term outcomes without progression to more invasive interventions. Anyone experiencing persistent back pain should consult with healthcare providers who can identify the specific cause and recommend targeted treatment strategies rather than generic pain management alone.