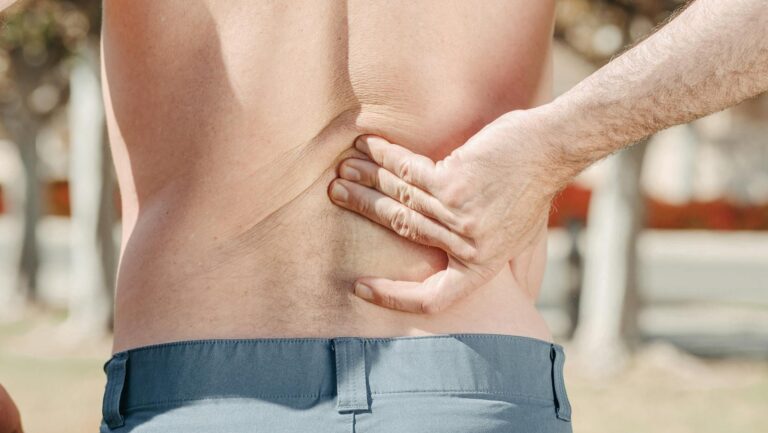
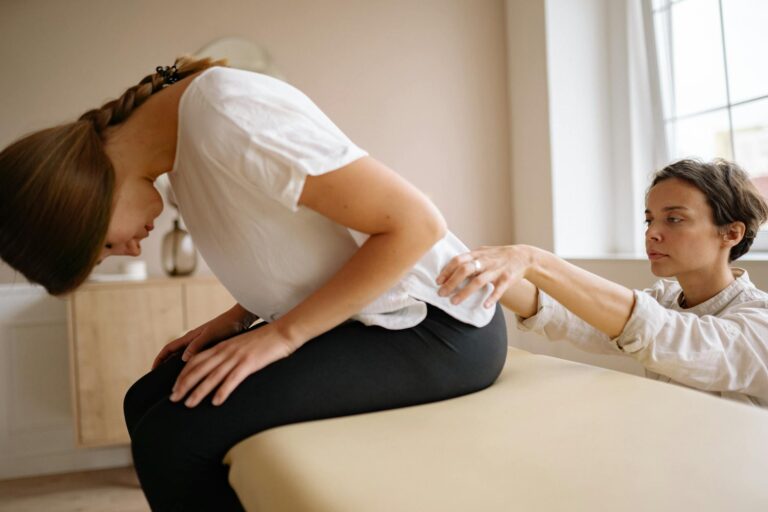
Doctors identify nine primary causes of chronic lower back pain, each requiring different approaches to treatment and management. The most common causes are mechanical in nature—lumbar strain and sprain account for 70% of mechanical low back pain cases, while age-related degenerative changes, herniated disks, compression fractures, and spinal stenosis round out the structural issues. Beyond the spine itself, occupational factors, lifestyle choices like smoking and obesity, psychosocial elements such as depression and anxiety, and socioeconomic circumstances all significantly influence whether acute back pain becomes chronic. Consider a 55-year-old office worker with poor posture who smokes and struggles with sleep quality due to anxiety—their chronic back pain likely stems from a combination of occupational ergonomics, lifestyle, and mental health factors, not just a single structural problem.
This article explores all nine categories that doctors routinely see in their patients with chronic lumbar pain, helping you understand which factors may be contributing to your own symptoms or those of a loved one. Understanding these causes matters because chronic lower back pain now affects an estimated 619 million people globally, with projections reaching 843 million by 2050. More concerning, low back pain has been the leading cause of years lived with disability since 1990. Between 4% and 25% of patients who experience acute low back pain go on to develop chronic pain, meaning identifying modifiable causes early can prevent progression. This article breaks down the mechanical, occupational, lifestyle, and psychological factors doctors identify when diagnosing chronic lumbar pain.
Table of Contents
- Lumbar Strain and Sprain—The Most Frequent Diagnosis
- Degenerative Disc Disease and Age-Related Structural Changes
- Herniated Discs and Spinal Compression
- Compression Fractures and Osteoporotic Changes
- Spinal Stenosis and Narrowing of the Spinal Canal
- Occupational and Ergonomic Risk Factors
- Lifestyle Factors—Smoking and Obesity
- Psychosocial Factors and Mental Health
- Socioeconomic Factors and Demographic Influences
- Conclusion
Lumbar Strain and Sprain—The Most Frequent Diagnosis
lumbar strain and sprain represent the single largest category of mechanical low back pain, accounting for approximately 70% of all cases. A strain occurs when muscles or tendons that support the lower back are stretched or torn, while a sprain involves injury to the ligaments that connect the vertebrae. These injuries can result from sudden movements, improper lifting, falls, or overuse. The key distinction between acute and chronic strain is duration—most muscle strains resolve within weeks, but some people develop chronic inflammation, scar tissue formation, or persistent muscle guarding that perpetuates pain.
What makes lumbar strain particularly relevant to chronic pain development is the cycle it creates. When muscles are injured, they tighten in response to pain, limiting movement and causing weakness. Over time, weak muscles cannot adequately support the spine, leading to poor posture and compensatory movement patterns. A patient who experiences a strain from lifting something improperly might develop chronic pain not from the initial injury itself but from months of avoiding activity, deconditioned muscles, and altered movement mechanics. For individuals with cognitive concerns—including those managing early dementia—chronic pain from strain can further complicate mobility and increase fall risk, creating a compounding health problem.
Degenerative Disc Disease and Age-Related Structural Changes
Intervertebral disc degeneration represents approximately 40% of chronic lower back pain overall, making it nearly as prevalent as acute strain when considering the full population with chronic symptoms. The discs between vertebrae are composed of a tough outer layer (annulus fibrosus) and a gel-like center (nucleus pulposus). As people age, these discs lose water content, become less flexible, and develop tears or bulges. Additionally, the facet joints—small joints at the back of the spine that guide movement—develop osteoarthritis and bone spurs.
Age strongly predicts which structural changes patients develop. Younger individuals with low back pain typically experience muscular strain or disc herniation, whereas older adults more commonly have degenerative disc disease, facet arthropathy, osteoporotic compression fractures, and spinal stenosis. However, not everyone with degenerative changes experiences pain—imaging studies show many asymptomatic people have significant disc degeneration and arthritis. This means doctors cannot simply look at an X-ray or MRI and declare that degeneration “is” the cause; symptoms must correlate with imaging findings, and other factors must be ruled out.
Herniated Discs and Spinal Compression
Herniated intervertebral discs account for approximately 4% of mechanical low back pain cases, yet they deserve detailed attention because they represent one of the most recognizable causes patients know by name. When the outer layer of a disc ruptures or weakens, the inner gel pushes through, potentially pressing on nerve roots or the spinal cord itself. This compression can cause pain radiating into the legs (sciatica), weakness, numbness, or loss of bladder and bowel control in severe cases.
The critical warning here is that small disc herniations often cause no symptoms and require no treatment, whereas others cause significant pain with minimal anatomical changes. A large disc bulge might produce only mild discomfort, while a small disc herniation in an unfortunate location might cause severe radiculopathy. This unpredictability is why imaging alone does not determine treatment—clinical symptoms and physical examination findings must guide decision-making. For older patients, particularly those with cognitive decline, monitoring for changes in leg weakness or loss of bowel/bladder control is essential, as these can indicate serious nerve compression requiring urgent intervention.

Compression Fractures and Osteoporotic Changes
Osteoporotic compression fractures account for about 4% of mechanical low back pain cases and become increasingly common with age, especially in postmenopausal women. These fractures occur when weakened vertebral bodies collapse under normal loading, sometimes with minimal or no trauma. A person might develop a compression fracture simply from a cough, sneeze, or minor fall. Unlike traumatic fractures that cause acute severe pain, some compression fractures develop gradually with slowly worsening chronic pain, stooped posture, and loss of height.
Multiple compression fractures create a particularly challenging situation—each fracture reduces spinal stability and changes the mechanical distribution of load across remaining vertebrae. Someone with three or four compression fractures may have chronic pain that persists despite adequate pain management because the underlying structural instability remains. Patients with dementia or cognitive decline need special attention here because they cannot always communicate early warning signs of new fractures, and confusion can increase fall risk. Prevention through adequate calcium, vitamin D, exercise, and fall prevention becomes especially important in this population.
Spinal Stenosis and Narrowing of the Spinal Canal
Spinal stenosis, narrowing of the spinal canal, accounts for approximately 3% of mechanical low back pain cases but becomes increasingly prevalent with age. The narrowing can result from disc bulges, bone spurs, thickened ligaments, or collapsed vertebrae pressing on the spinal cord or nerve roots. Patients with stenosis often report claudication—pain or numbness that worsens with walking and improves with sitting or lying down, a pattern that differs from vascular claudication and helps doctors identify the source.
A critical limitation of treating stenosis is that conservative measures provide relief for many patients, yet some progress to require surgery. Identifying which patients will respond to physical therapy, anti-inflammatory medications, and epidural injections versus those who need surgical decompression requires careful clinical monitoring over time. For elderly patients or those with cognitive concerns, managing stenosis can be complicated by other comorbidities and the need for careful anesthesia planning if surgery becomes necessary.

Occupational and Ergonomic Risk Factors
Occupational ergonomic factors account for nearly 25% of years lived with disability from low back pain, according to the Global Burden of Disease Study 2021. This includes prolonged sitting at desks with poor posture, repetitive bending and lifting, manual labor jobs, and vibration exposure from vehicles or machinery. Office workers often assume their jobs are “safe,” yet sedentary work with poor ergonomics is a major contributor to chronic pain development.
A warehouse worker might develop chronic pain from years of heavy lifting, while an accountant develops it from years of poor desk posture and physical deconditioning. Low physical activity levels and physical deconditioning independently predict chronic pain development and perpetuation. Paradoxically, appropriate exercise is one of the most effective treatments for chronic low back pain, yet pain itself discourages activity, creating a vicious cycle. The challenge lies in distinguishing between pain that warrants movement restriction and pain that benefits from carefully prescribed physical activity—this is where physical therapy and medical guidance become essential.
Lifestyle Factors—Smoking and Obesity
Smoking accounts for 12.5% of attributable disability years from low back pain, making it one of the most modifiable risk factors with documented impact. Smoking reduces blood flow to spinal tissues, slows healing, promotes inflammation, and increases pain sensitivity. Patients who smoke are more likely to develop chronic pain from initial injuries and less likely to improve with treatment.
Additionally, smokers undergoing spine surgery have higher complication rates and slower fusion rates when bone healing is required. Elevated body mass index contributes 11.5% of attributable disability years, primarily through increased mechanical loading on the spine and associated inflammation. Obesity also correlates with depression, sleep disturbance, and poor health behaviors, compounding the risk for chronic pain development. Someone who is both obese and smokes faces a substantially elevated risk of chronic pain, and cessation of smoking combined with weight reduction represents one of the most effective lifestyle interventions for pain reduction.
Psychosocial Factors and Mental Health
Depression, anxiety, and poor sleep quality significantly increase both the chronicity of low back pain and its severity. These are not merely psychological responses to pain; rather, they alter pain signaling pathways in the brain and reduce pain tolerance. Patients with depression are more likely to catastrophize about their pain, develop maladaptive pain coping behaviors, and transition from acute to chronic pain.
This connection is especially relevant for individuals with cognitive concerns, as depression frequently accompanies early cognitive decline and can amplify perceived pain intensity. Alcohol use disorders are also associated with chronic pain progression, partly through inflammatory pathways and partly through impaired pain regulation. Maladaptive coping strategies—such as avoidance of activity, catastrophizing, or isolation—perpetuate pain and reduce quality of life. Crucially, for individuals managing dementia or early cognitive decline, untreated pain can accelerate cognitive deterioration and increase behavioral symptoms, making pain management a critical component of overall cognitive health.
Socioeconomic Factors and Demographic Influences
Systematic reviews have identified that low education level, low income, and unfavorable family status predict a chronic course of low back pain. Socioeconomic barriers affect access to physical therapy, specialist care, ergonomic workplace modifications, and time for exercise. Someone working multiple jobs with limited income has less access to preventive care and treatment options, increasing their risk of progressing to chronic pain.
Social isolation and poor family support also predict worse pain outcomes, highlighting the importance of psychosocial intervention in treatment plans. Age itself influences cause distribution—younger patients develop pain more frequently from muscular strain or disc herniation, while older adults experience more degenerative changes, stenosis, and compression fractures. Understanding these age-related patterns helps doctors prioritize investigations and treatments appropriate to the patient’s age and likely anatomical substrate.
Conclusion
Chronic lumbar pain develops from a complex interaction of mechanical, occupational, lifestyle, psychosocial, and socioeconomic factors. Most patients have multiple contributing causes rather than a single identifiable problem. With 619 million people globally affected and projections reaching 843 million by 2050, understanding these nine categories—lumbar strain, degenerative disc disease, herniated discs, compression fractures, spinal stenosis, occupational factors, smoking, obesity, and psychosocial influences—empowers both patients and healthcare providers to address modifiable risk factors and develop comprehensive treatment plans.
The critical opportunity lies in early identification of risk factors before acute pain transitions to chronic pain (a fate affecting 4-25% of acute cases). For individuals managing cognitive concerns or dementia, chronic pain represents a particular risk because it impairs mobility, increases fall risk, can accelerate cognitive decline, and complicates behavioral management. Addressing pain through a multidisciplinary approach—combining appropriate imaging, physical therapy, lifestyle modification, mental health support, and occupational ergonomics—offers the best chance of preventing chronic pain development or improving outcomes for those already affected.