Chronic back pain affects roughly one in four adults globally, and doctors most frequently diagnose it as stemming from one of twelve main causes: muscle strain, osteoarthritis, degenerative disc disease, disc herniation, lumbar spondylosis, spinal stenosis, facet arthropathy, osteoporotic compression fractures, ligament injuries, inflammatory conditions, postural dysfunction, and psychosocial factors. The vast majority of these diagnoses fall into predictable patterns—a 45-year-old with an office job presenting with shooting leg pain often has a disc herniation, while a 70-year-old complaining of pain that worsens with walking may have spinal stenosis. Understanding which condition a doctor suspects requires knowing how these causes present differently and which risk factors make them more likely.
Here’s an important caveat: despite these twelve commonly diagnosed causes, only about 10% of doctor visits for back pain result in a definitive diagnosis. Roughly 85-90% of low back pain is classified as “non-specific,” meaning no precise underlying cause can be identified through standard imaging or physical examination. This can be frustrating for patients seeking clear answers, but it also explains why back pain management often focuses on treatment strategies rather than targeting a specific structural problem. This article walks through each of the twelve causes doctors do successfully diagnose, what makes them different, who tends to develop them, and what the evidence tells us about their prevalence.
Table of Contents
- What Does Your Doctor Mean by “Muscle or Tendon Strain”?
- Degenerative Disc Disease, Osteoarthritis, and Wear-and-Tear Conditions
- Disc Herniation and Nerve Compression Disorders
- Spinal Stenosis and Facet Arthropathy in Older Adults
- Compression Fractures and When Bone Health Matters
- Inflammatory, Psychological, and Systemic Factors
- The Diagnostic Challenge and When Imaging Matters
- Conclusion
What Does Your Doctor Mean by “Muscle or Tendon Strain”?
Muscle and tendon strain is the most common acute cause of back pain and remains a frequent chronic diagnosis, especially in people with physically demanding jobs or sedentary lifestyles that weaken supporting muscles. When you lift incorrectly, overexert yourself, or make a sudden twisting motion, the muscle fibers or tendons in your back can partially tear or become overstretched, causing inflammation and localized pain. This type of injury typically worsens with movement and improves with rest over days to weeks.
The key distinction is that muscle strain itself is almost never the cause of chronic back pain lasting months or years—if someone has been in pain for more than three months from an initial strain, something else is usually driving the ongoing pain. However, a history of muscle strain can predispose you to recurrent episodes. A warehouse worker who tweaked his back five years ago may have developed weakness or scar tissue that makes him prone to re-injury with each heavy lift. This is different from a structural problem like a herniated disc, which causes pain through nerve compression rather than tissue inflammation.

Degenerative Disc Disease, Osteoarthritis, and Wear-and-Tear Conditions
Degenerative disc disease and osteoarthritis are the most common chronic causes, arising from the natural wear and tear of the spine over decades. Your spinal discs are shock-absorbing structures filled with gel; as you age, these discs lose water content and elasticity, a process that accelerates in people who smoke, are overweight, have physically demanding jobs, or experience high psychological stress. Osteoarthritis involves the breakdown of cartilage in the facet joints of the spine, creating inflammation and restricted movement. Lumbar spondylosis encompasses both disc degeneration and bone spur formation, primarily affecting adults over 40.
These three conditions often occur together. A 55-year-old might have degenerative discs in the lower spine, osteoarthritis in multiple facet joints, and early spondylotic changes, all contributing to chronic dull or achy pain that tends to worsen with prolonged sitting or certain activities. The important caveat: many people show significant disc degeneration or arthritis on imaging yet experience little or no pain, while others with minimal imaging findings report severe symptoms. This mismatch means that imaging abnormalities alone cannot predict your pain level or prognosis. Treatment focuses on strengthening muscles, maintaining mobility, and managing inflammation rather than “fixing” the degeneration itself.
Disc Herniation and Nerve Compression Disorders
A disc herniation occurs when the gel-filled center of a spinal disc pushes through the tough outer layer, potentially pressing on a nearby nerve root. This most frequently affects the L4-S1 segments in the lower back and produces distinctive symptoms: radiating pain, tingling, numbness, or weakness that travels down one leg (sciatica). Unlike the dull, localized pain of arthritis, nerve compression pain is often sharp, burning, or electric-shock-like. A patient might describe it as pain in the buttock that shoots all the way to the foot, with weakness that makes it hard to lift the foot or point the toes.
The good news is that disc herniations often improve on their own within weeks to months as inflammation settles and the body reabsorbs the disc material. Physical therapy, anti-inflammatory medications, and activity modification help most people recover without surgery. However, if a herniation compresses the nerve severely enough to cause progressive muscle weakness or loss of bowel or bladder control—called cauda equina syndrome—emergency surgery is needed. This is rare but serious, which is why any new numbness in the groin area or loss of bladder control warrants immediate medical evaluation.
Spinal Stenosis and Facet Arthropathy in Older Adults
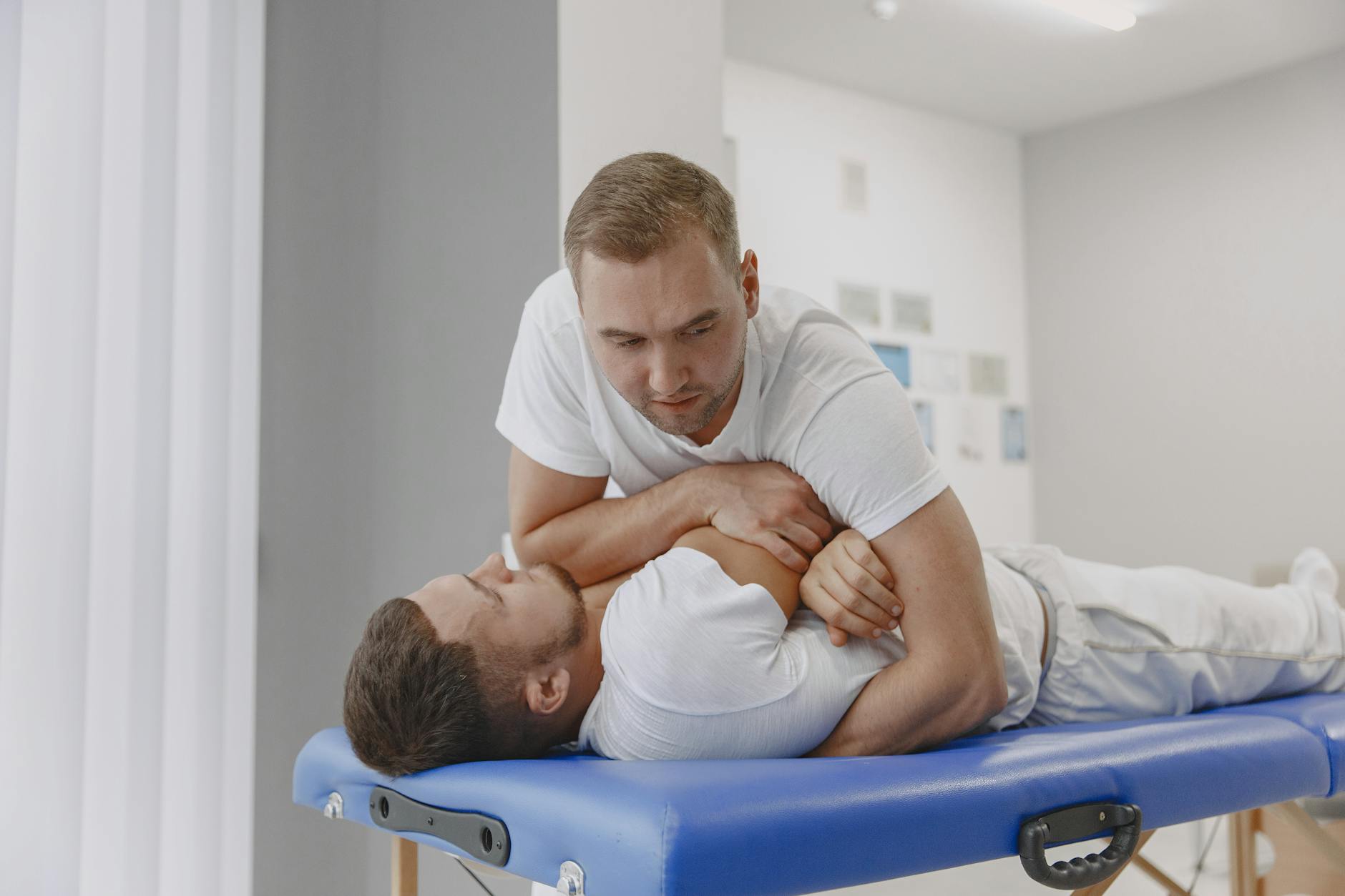
Spinal stenosis is the narrowing of the spinal canal, restricting the space available for the spinal cord and nerves. It becomes more common with age as discs bulge, bones thicken, and ligaments harden. Facet arthropathy refers to arthritis of the facet joints, the small joints on the back of each vertebra that guide spinal movement. Both conditions are highly prevalent in people over 65 and often coexist. A classic presentation is a patient who can walk short distances on level ground but experiences severe leg pain, cramping, or numbness after walking further—symptoms that improve dramatically when sitting down or bending forward.
This pattern, called claudication, distinguishes stenosis from other causes. The tradeoff in managing spinal stenosis is that while lying down or sitting typically relieves symptoms, you also need regular movement and exercise to prevent deconditioning and muscle weakness. Too much rest actually worsens the underlying problem. Physical therapy emphasizing core strength, flexibility, and aerobic conditioning helps many patients maintain function for years. Older adults with severe stenosis sometimes experience improvement with epidural steroid injections or, in select cases, surgical decompression if conservative care fails and functional impairment is significant.
Compression Fractures and When Bone Health Matters
Osteoporotic compression fractures occur when weakened bones in the spine collapse, reducing vertebral height and causing acute to chronic pain. These fractures are much more common in older adults, particularly post-menopausal women, but can occur in anyone with significant bone loss from conditions like osteoporosis, multiple myeloma, or long-term corticosteroid use. A minor fall or even a heavy cough can fracture a weakened vertebra. The pain is often severe initially, typically in the mid-to-lower back, and may improve over weeks but leave residual chronic pain and progressive loss of height.
A critical warning: if you’re over 50, have risk factors for osteoporosis (family history, low body weight, smoking, steroid use, early menopause), and develop new onset back pain, mention this to your doctor. Bone density screening (DEXA scan) and calcium-vitamin D supplementation can prevent fractures. Some patients with acute compression fractures benefit from kyphoplasty, a procedure that injects cement into the collapsed vertebra to restore height and stabilize the fracture. However, this procedure is not appropriate for everyone, and the evidence for long-term benefit beyond pain relief is mixed.
Inflammatory, Psychological, and Systemic Factors
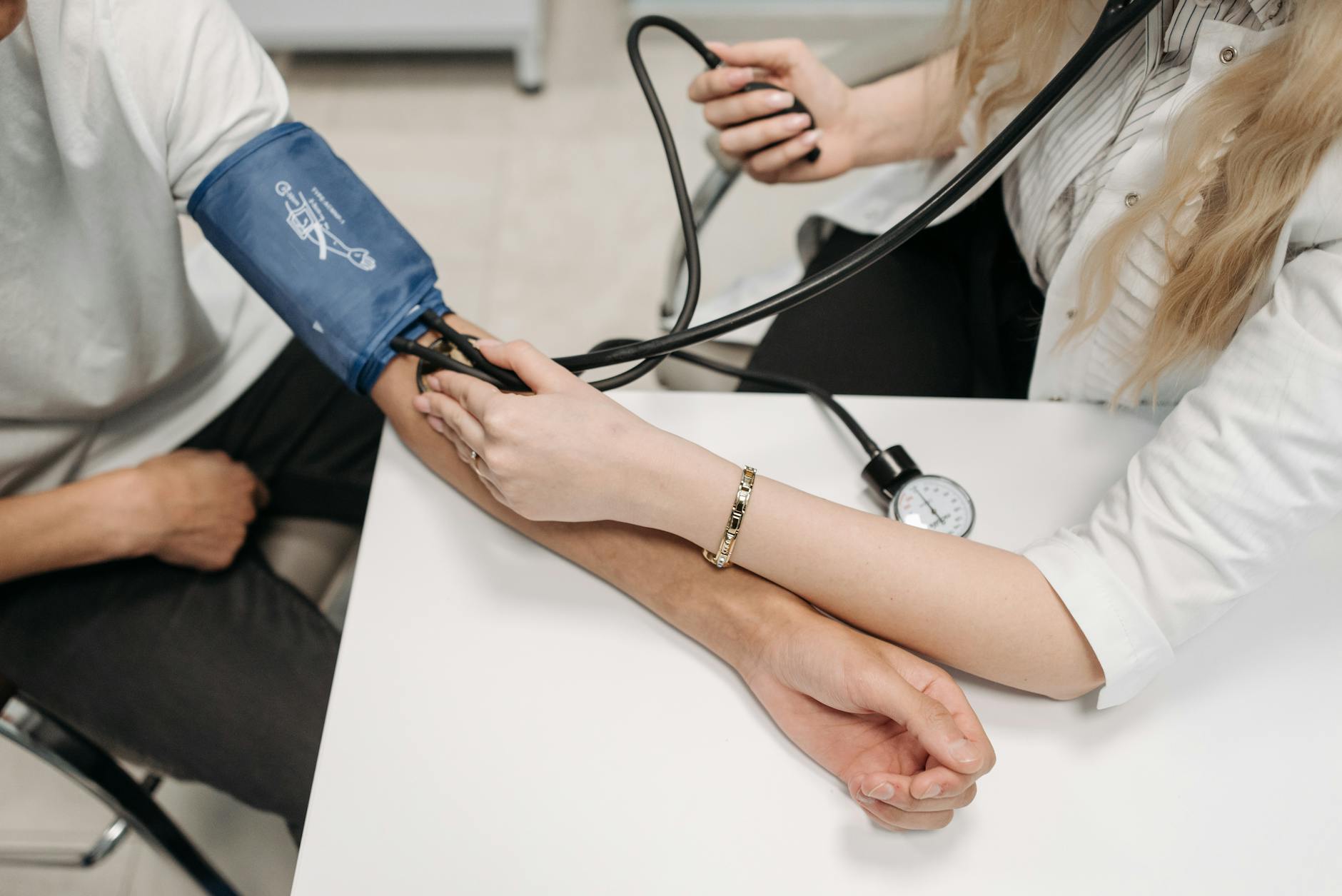
Beyond structural causes, doctors increasingly recognize that chronic back pain involves inflammatory pathways, neurological sensitization, and psychological factors including depression, anxiety, stress, and trauma history. Inflammatory conditions like ankylosing spondylitis can cause back pain, though these are less common than degenerative conditions. Psychological stress and poor coping mechanisms don’t “cause” back pain to exist from nothing, but they significantly amplify pain perception and delay recovery—a patient under high stress at work often reports worsening pain during stressful periods, even if imaging shows stable structural changes.
The evidence shows that addressing psychological factors—through cognitive-behavioral therapy, mindfulness, or stress reduction—can be as effective as physical interventions for some patients with chronic pain. This isn’t to say the pain is “all in your head,” but rather that pain is a complex experience involving brain, spine, and life circumstances. A person with the same disc herniation as someone else might recover quickly or develop chronic pain depending on fear-avoidance beliefs, work stress, sleep quality, and social support.
The Diagnostic Challenge and When Imaging Matters
One of the most important facts about chronic back pain is that only 10% of doctor visits result in a definitive diagnosis. This frustrates many patients, but it also reflects reality: back pain is a symptom with multiple potential causes, many of which don’t show up clearly on imaging. Some patients undergo repeated MRI scans searching for a diagnosis, only to find normal or minor degenerative changes that don’t explain their pain level.
Unnecessary imaging delays care, increases costs, and sometimes raises anxiety by highlighting incidental findings that don’t matter. Modern best practice suggests that imaging—MRI, CT, or X-rays—should be reserved for specific situations: when red flag symptoms suggest serious pathology (fever, unexplained weight loss, bowel/bladder symptoms, progressive neurological weakness), when symptoms have persisted beyond 6-12 weeks despite conservative treatment, or when specific structural findings would change management. For most acute back pain, a thorough physical examination and history are more valuable than immediate imaging. This approach saves money, reduces unnecessary radiation, and gets patients started on effective treatments like physical therapy and activity modification sooner.
Conclusion
Chronic back pain is one of the most common health complaints globally, affecting roughly 619 million people and projected to reach 843 million by 2050. Doctors frequently diagnose twelve main causes—from muscle strain and osteoarthritis to disc herniation and spinal stenosis—each with distinct presentations and prognostic patterns. Age, occupation, smoking, weight, and psychological stress all influence which condition develops and how severely it manifests.
Understanding your specific diagnosis helps you and your doctor tailor treatment, but it’s equally important to recognize that many people experience chronic back pain without a definitive structural diagnosis, and that this doesn’t mean the pain is less real or less treatable. If you’re experiencing new back pain lasting more than a few weeks, start with your primary care provider, who can perform a focused history and examination to identify red flag symptoms and clarify whether imaging is needed. Most back pain improves with conservative care: staying active, maintaining good posture, strengthening core muscles, managing stress, and treating any underlying conditions like osteoporosis or obesity. Even when a specific diagnosis is identified, these strategies remain the foundation of long-term management and prevention of recurrent episodes.





