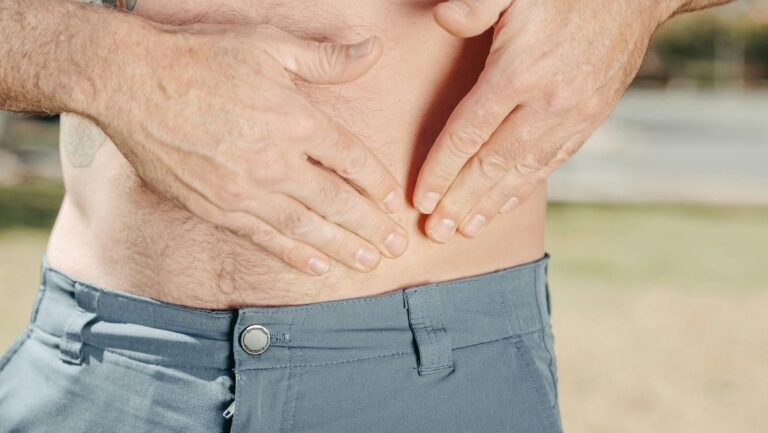
Back pain ranks as the single leading cause of disability worldwide, and the five most common reasons people develop it are muscle strain, degenerative disc disease, excess body weight, occupational hazards, and osteoarthritis or spinal stenosis. If you or someone you care for is dealing with persistent back pain, understanding which of these causes is at play matters enormously — because the right treatment depends entirely on the right diagnosis. Consider a 72-year-old woman with moderate dementia whose family notices she has become more agitated and resistant to standing. The underlying issue turns out to be spinal stenosis, but because she cannot clearly articulate her pain, months pass before anyone identifies the problem.
Globally, 619 million people were affected by low back pain in 2020, and that number is projected to climb to 843 million by 2050, according to the Global Burden of Disease Study published in The Lancet Rheumatology. In the United States alone, 39 percent of adults reported experiencing back pain in the past three months, per CDC data, and the country spends an estimated $100 billion annually on back pain-related costs. These figures are staggering, but what makes them especially relevant for aging adults and dementia caregivers is that back pain often goes underreported and undertreated in older populations. This article breaks down each of the five major causes, examines why they matter for brain health and cognitive care, and explores emerging research suggesting that chronic back pain may actually originate in the brain itself.
Table of Contents
- What Are the Five Leading Causes of Back Pain and Why Do They Matter?
- Muscle Strain and Ligament Injury — The Most Common Culprit
- Degenerative Disc Disease and Its Connection to Aging
- How Obesity and Excess Weight Contribute to Chronic Back Pain
- Occupational Hazards and Ergonomic Risks That Damage the Spine
- Osteoarthritis and Spinal Stenosis in Older Adults
- What Emerging Brain Research Means for Chronic Back Pain
- Conclusion
- Frequently Asked Questions
What Are the Five Leading Causes of Back Pain and Why Do They Matter?
The five causes — muscle strain, degenerative disc disease, obesity, occupational factors, and osteoarthritis or spinal stenosis — cover the vast majority of back pain cases. Roughly 90 percent of all back pain is classified as non-specific mechanical pain, meaning it stems from muscles, ligaments, or joints rather than from a serious underlying disease like cancer or infection. This is reassuring in one sense, but it also means that diagnosis can be frustratingly vague. A doctor may tell you that your back hurts because of a muscle strain without being able to pinpoint the exact tissue involved.
For older adults and people living with dementia, the picture gets more complicated. Degenerative disc disease, osteoarthritis, and spinal stenosis become increasingly prevalent with age, while the ability to communicate pain clearly may decline. A person with Alzheimer’s disease might express back pain through behavioral changes — refusing to walk, increased agitation, or disrupted sleep — rather than saying “my back hurts.” Caregivers who understand the common causes of back pain are better equipped to recognize these signals and seek appropriate medical evaluation. The difference between a muscle strain that resolves in a few weeks and spinal stenosis that requires ongoing management is significant, and mistaking one for the other can lead to months of unnecessary suffering.
Muscle Strain and Ligament Injury — The Most Common Culprit
Muscle strain and ligament injury account for the largest share of back pain cases, particularly among younger and middle-aged adults. These injuries typically result from lifting something heavy with poor form, twisting awkwardly, or sudden movements that overload the soft tissues of the back. The good news is that most of these injuries resolve within six weeks. The less reassuring news, based on research cited by ScienceDaily in 2024, is that roughly one-third of back pain cases become persistent and may last for years. A common misconception is that bed rest is the best remedy for an acute muscle strain.
In reality, prolonged inactivity tends to make things worse by weakening the muscles that support the spine. Gentle movement, over-the-counter anti-inflammatory medication, and gradual return to normal activities are generally more effective. However, if pain persists beyond six to eight weeks, or if it is accompanied by numbness, tingling, or weakness in the legs, that is a signal that something beyond a simple strain may be involved. For caregivers of older adults, it is worth noting that a fall — even a seemingly minor one — can cause muscle and ligament injuries that the person may not report. Unexplained changes in mobility or posture should prompt a conversation with a healthcare provider.
Degenerative Disc Disease and Its Connection to Aging
Degenerative disc disease is not really a “disease” in the traditional sense but rather a natural process in which the intervertebral discs — the rubbery cushions between the vertebrae — gradually lose hydration and structural integrity over time. According to research published in Nature’s Bone Research journal in 2025, approximately 40 percent of chronic low back pain cases are attributed to intervertebral disc degeneration. This makes it one of the most significant causes of persistent back pain in older adults. What makes degenerative disc disease particularly relevant for dementia caregivers is its slow, progressive nature. A person may have moderate disc degeneration visible on an MRI but experience no pain at all, while someone else with milder changes on imaging may be in considerable discomfort. The correlation between what scans show and what patients feel is notoriously unreliable.
This creates a challenge when caring for someone who cannot easily describe their symptoms. A practical example: an 80-year-old man with vascular dementia begins resisting transfers from bed to wheelchair. His caregiver assumes it is a behavioral symptom of dementia, but a physical examination reveals significant disc degeneration at L4-L5 that has been causing increasing pain. Once treated with gentle physical therapy and appropriate pain management, his resistance to transfers largely resolves. It is also worth noting that degenerative disc disease does not inevitably lead to debilitating pain. Many people live with significant disc degeneration and remain active and comfortable. The key is maintaining core strength, staying physically active within one’s abilities, and addressing pain early rather than allowing it to become entrenched.

How Obesity and Excess Weight Contribute to Chronic Back Pain
Carrying excess body weight places additional mechanical load on the spine and its supporting structures, but the relationship between obesity and back pain goes beyond simple physics. Excess adipose tissue, particularly visceral fat, triggers a systemic inflammatory response that can sensitize pain pathways and accelerate the degeneration of spinal structures. According to the Global Burden of Disease Study published in The Lancet Rheumatology, obesity is one of three modifiable risk factors — alongside smoking and ergonomic factors — that together explain 38.8 percent of years lived with disability due to back pain globally. The tradeoff that many older adults face is between the benefits of weight loss and the practical challenges of achieving it. Exercise is one of the most effective interventions for both back pain and weight management, but back pain itself can make exercise difficult or intimidating. Walking, swimming, and water-based exercises tend to be the most accessible options for people dealing with both excess weight and back pain, as they reduce the load on the spine while still providing cardiovascular and musculoskeletal benefits.
For individuals with dementia, structured physical activity programs — even simple seated exercises — can help manage both weight and pain while also providing cognitive stimulation. However, it is important to note that weight loss alone is not a guaranteed solution for back pain. A person who loses 30 pounds may still have significant disc degeneration or spinal stenosis. Weight management is best understood as one component of a broader approach rather than a standalone fix. Addressing smoking, improving workplace or daily ergonomics, and maintaining regular physical activity are equally important. The encouraging finding from the Institute for Health Metrics and Evaluation is that addressing these three modifiable risk factors together could reduce the global burden of low back pain by approximately 39 percent.
Occupational Hazards and Ergonomic Risks That Damage the Spine
Physically demanding jobs and sedentary work in non-neutral postures are significant contributors to back pain across all age groups. Research from the Global Burden of Disease Study has shown that bent postures at work are linked to new-onset low back pain in nurses, while prolonged sitting in call center employees is associated with chronic low back pain. The common thread is sustained or repetitive stress on spinal structures without adequate recovery time. For caregivers — both professional and family — this cause of back pain is especially relevant because caregiving itself is physically demanding work. Lifting, transferring, and repositioning a person with limited mobility places enormous strain on the back, particularly when done without proper body mechanics or assistive equipment.
A family caregiver who spends years helping a spouse with dementia get in and out of bed, on and off the toilet, and in and out of chairs is at substantial risk for developing chronic back pain. The limitation that many caregivers face is that they know they should use proper lifting techniques and mechanical aids, but in the moment — when someone is falling, or resisting, or the equipment is in another room — they default to whatever gets the job done. Investing in a simple transfer belt, a bed rail, or a sliding board can make a meaningful difference. Caregivers should also be aware that once back pain becomes chronic, it tends to become self-reinforcing: pain leads to guarded movement, which leads to muscle weakness, which leads to more pain. Breaking this cycle early is far easier than addressing it after years of compensatory patterns have taken hold.

Osteoarthritis and Spinal Stenosis in Older Adults
Osteoarthritis affects the facet joints of the spine and causes chronic inflammation, stiffness, and pain. The condition impacts roughly 33 million American adults, according to the National Council on Aging. Spinal stenosis — the narrowing of the spinal canal that puts pressure on the spinal cord and nerve roots — is especially prevalent among older adults and is one of the leading causes of chronic back pain in people over 65. These two conditions frequently coexist and can produce symptoms that mimic or exacerbate cognitive and behavioral changes in people with dementia.
Pain from spinal stenosis, for example, often worsens with standing and walking and improves with sitting or bending forward. A person with dementia who suddenly refuses to walk or who insists on leaning forward in their chair may be instinctively adopting a posture that relieves nerve compression. Recognizing this pattern can help caregivers and clinicians distinguish between a behavioral symptom of dementia and an orthopedic problem that has a specific, treatable cause. Treatment options range from physical therapy and anti-inflammatory medications to epidural steroid injections and, in severe cases, surgical decompression.
What Emerging Brain Research Means for Chronic Back Pain
One of the most compelling developments in back pain research comes from a University of Colorado Anschutz study that found many cases of chronic back pain are driven by changes in the brain rather than ongoing tissue damage. In these cases, the pain system essentially gets “stuck” — it keeps firing long after the original injury has healed. The brain continues to interpret normal signals from the back as painful, creating a self-sustaining loop that has little to do with the current state of the spine. This finding is particularly meaningful for a brain health audience because it highlights the bidirectional relationship between pain and cognition.
Chronic pain consumes attentional resources, disrupts sleep, contributes to depression, and may accelerate cognitive decline. Conversely, cognitive impairment can alter pain perception and make it harder for individuals to engage in the psychological and behavioral strategies — such as graded exposure and cognitive reframing — that are increasingly used to treat centralized pain. As researchers continue to untangle these connections, the hope is that interventions targeting the brain’s pain-processing pathways could offer relief for people whose back pain has resisted conventional orthopedic treatments. For now, the practical takeaway is that persistent back pain is not always a sign that something is structurally wrong with the spine, and treating it may require addressing the nervous system as much as the musculoskeletal system.
Conclusion
The five major causes of back pain — muscle strain, degenerative disc disease, obesity, occupational hazards, and osteoarthritis or spinal stenosis — are not mutually exclusive. Most older adults dealing with chronic back pain are contending with some combination of these factors, and effective treatment requires identifying which ones are most relevant in each individual case. For people living with dementia and their caregivers, the challenge is compounded by communication barriers, but understanding the common patterns of each condition can help bridge that gap.
Back pain does not have to be accepted as an inevitable part of aging or dismissed as a minor complaint. With low back pain standing as the number one cause of disability worldwide and projected to affect 843 million people by 2050, the scale of this problem demands attention. Whether through maintaining a healthy weight, using proper body mechanics during caregiving, staying physically active, or seeking timely medical evaluation for persistent symptoms, there are concrete steps that can reduce both the severity and the duration of back pain. The emerging research on the brain’s role in chronic pain adds another dimension of hope — and another reason to take back pain seriously rather than simply enduring it.
Frequently Asked Questions
How long does back pain typically last?
Most cases of acute back pain resolve within six weeks. However, research shows that approximately one-third of cases become persistent and may last for years. If pain has not improved after six to eight weeks, or if it is accompanied by leg weakness or numbness, medical evaluation is important.
Can back pain be a sign of something more serious than a muscle strain?
Yes. While 90 percent of back pain is mechanical and non-serious, pain accompanied by fever, unexplained weight loss, loss of bladder or bowel control, or progressive leg weakness warrants immediate medical attention. These can be signs of infection, tumor, or cauda equina syndrome.
How can I tell if a person with dementia is experiencing back pain?
Watch for behavioral cues such as resisting movement, increased agitation, guarding a particular body part, changes in posture, reluctance to sit or stand, facial grimacing, and disrupted sleep. Standardized pain observation tools like the PAINAD scale can help caregivers and clinicians assess pain in people who cannot self-report.
Does losing weight actually help with back pain?
It can, but it is not a guaranteed solution. Excess weight contributes to back pain through both mechanical stress and systemic inflammation. Weight loss reduces those factors but will not reverse structural problems like disc degeneration or spinal stenosis. It is most effective as part of a comprehensive approach that includes exercise and ergonomic adjustments.
Is exercise safe when you have back pain?
In most cases, gentle movement and exercise are not only safe but beneficial. Prolonged bed rest tends to worsen back pain by weakening supporting muscles. Walking, swimming, and physical therapy exercises designed to strengthen the core are generally well tolerated. However, any new exercise program should be discussed with a healthcare provider, especially for older adults or those with multiple health conditions.