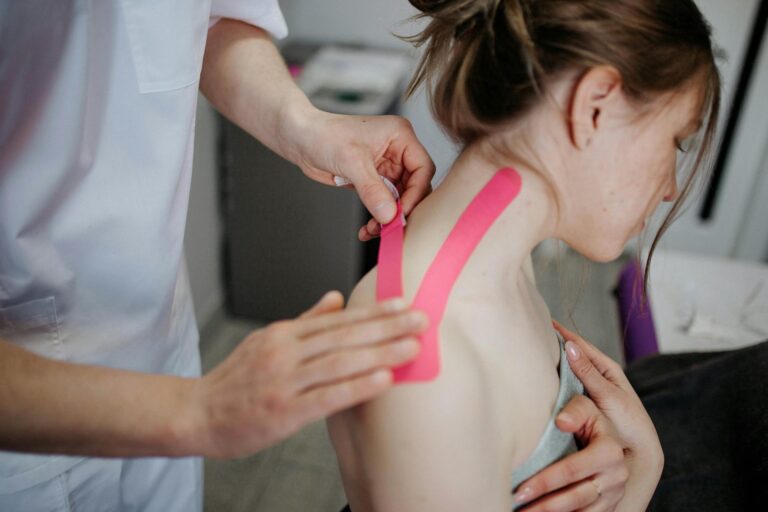
People wait too long to use their epinephrine auto-injector because they fail to recognize anaphylaxis, fear the needle, hope antihistamines will be enough, or simply don’t have the device on hand. That hesitation can be fatal. Delayed or absent epinephrine is the single most consistent risk factor for death from anaphylaxis across food, drug, and venom triggers, and fatal reactions can progress from first symptoms to respiratory or cardiac arrest within five to thirty minutes. Yet pre-hospital epinephrine use remains strikingly low — only 7.17% of adults and 20.98% of children experiencing anaphylaxis receive epinephrine before reaching the hospital. Consider a teenager at a school cafeteria who eats something containing a trace amount of tree nut. Within minutes, her lips swell and her throat tightens.
A teacher hands her Benadryl. Ten minutes pass. By the time someone locates her auto-injector in her locker, she’s in full anaphylaxis and a paramedic has to administer the shot en route to the emergency room. This scenario plays out with alarming regularity — roughly every ten seconds, a food allergy reaction sends someone to an American ER, totaling approximately 3.4 million food-allergy emergency visits per year. Anaphylaxis affects an estimated 1 in 50 Americans, with some experts placing the figure closer to 1 in 20. This article examines the specific reasons people delay using epinephrine, the medical consequences of that delay, the role cost and access play in the crisis, and what a newly approved needle-free alternative could change for the millions of people living with severe allergy risk.
Table of Contents
- Why Do So Many People Wait Too Long to Use an Epinephrine Auto-Injector?
- The Medical Consequences of Delaying Epinephrine — What the Research Shows
- How Cost and Access Barriers Keep Auto-Injectors Out of Reach
- Antihistamines vs. Epinephrine — Understanding the Critical Difference
- Caregivers, Schools, and the Challenge of Delegated Emergency Response
- Neffy — A Needle-Free Option That May Change the Equation
- What Needs to Change — Policy, Training, and the Road Ahead
- Conclusion
- Frequently Asked Questions
Why Do So Many People Wait Too Long to Use an Epinephrine Auto-Injector?
The reasons break down into a handful of recurring barriers, and they overlap in ways that compound the problem. The most commonly cited is a failure to recognize that anaphylaxis is actually happening. Symptoms can look different from one episode to the next, even when the same allergen is involved — one reaction might present as hives and stomach cramps, the next as throat swelling with no skin symptoms at all. That variability creates doubt, and doubt creates delay. According to the American College of Allergy, Asthma and Immunology and the Allergy and Asthma Network, this inconsistency is a leading contributor to under-treatment. Fear of the needle is another well-documented barrier, particularly among adolescents and their caregivers. Studies in the medical literature have repeatedly flagged needle phobia as a major reason people hesitate, even when they intellectually understand that anaphylaxis is life-threatening.
Compounding this is the “wait and see” mentality — the instinct to try an antihistamine like Benadryl first, monitor symptoms, and escalate only if things get worse. But antihistamines take thirty or more minutes to begin working and cannot reverse anaphylaxis. They address hives and itching; they do nothing for airway constriction or cardiovascular collapse. Harvard Health has been blunt on this point: epinephrine is the only effective treatment for anaphylaxis. Then there’s the basic problem of not having the device available. Less than half of at-risk patients carry their epinephrine auto-injector at all times, with carriage rates measured as low as 57% in published studies. Forty percent of patients report never carrying one because they believe they can simply avoid their allergen — a strategy that works until it doesn’t. A single mislabeled ingredient, a contaminated cutting board, or an insect sting in the backyard can override the best avoidance plan.

The Medical Consequences of Delaying Epinephrine — What the Research Shows
The data here is unambiguous. Most patients who use an auto-injector delay self-administration by more than ten minutes from the onset of symptoms. In that window, anaphylaxis can escalate from uncomfortable to life-threatening. An estimated 186 to 225 Americans die from anaphylaxis each year, a rate of 0.63 to 0.76 per million person-years. The case fatality rate among those who make it to a hospital or emergency department is approximately 0.3%. These numbers are low in absolute terms, but nearly every study examining fatal cases identifies the same thread: epinephrine was either not given or given too late.
Pre-hospital administration of epinephrine is associated with fewer hospital admissions, less intravenous fluid use in the emergency department, and lower odds of an uncontrolled reaction spiraling into something worse. Put simply, using the auto-injector early doesn’t just reduce mortality risk — it reduces the severity of the entire episode. A patient who self-injects within the first few minutes of symptom onset may avoid intubation, ICU admission, or a second biphasic reaction hours later. However, there’s an important limitation to acknowledge: epinephrine is not a cure, and it doesn’t eliminate the need for emergency medical care. Even after a successful injection, patients should call 911 and be monitored for at least four hours, because anaphylaxis can return after the drug wears off. The auto-injector buys time — critical, life-saving time — but it is the beginning of treatment, not the end of it. Patients who use their device and then skip the ER because they feel better are taking a serious gamble.
How Cost and Access Barriers Keep Auto-Injectors Out of Reach
For some patients, the delay isn’t psychological — it’s financial. A two-pack of brand-name EpiPens costs roughly $680 to $815 without insurance. Generic alternatives range from $100 to $500, depending on the pharmacy and the specific product. These are devices with expiration dates, which means families need to replace them regularly, often maintaining multiple sets for school, home, and travel. A 2023 survey found that 25% of patients who did not fill their epinephrine prescriptions cited cost as the reason, and 36% reported being unable to obtain the device due to co-pay burdens or prior authorization requirements from their insurer. This creates a grim arithmetic. A family with two allergic children might need four to six auto-injectors at any given time — two per child, with extras stashed at school or with grandparents.
Even at generic prices, that can exceed a thousand dollars a year out of pocket, assuming insurance cooperates. For families already stretched by other medical expenses, the auto-injector becomes a luxury rather than a necessity, which is a dangerous inversion of priorities for a device designed to prevent death. The access problem extends beyond cost. Some patients receive inconsistent advice from healthcare providers about when and how to use the device. Training at the point of prescription is often cursory — a quick demonstration with a trainer pen and a handout. When 35% to 43% of auto-injector uses involve erroneous technique, it’s clear that the training model is failing. A device that’s too expensive to buy, too confusing to use correctly, and carried inconsistently is a device that will not be used in time.

Antihistamines vs. Epinephrine — Understanding the Critical Difference
The most dangerous misconception in allergy management is the belief that Benadryl can substitute for epinephrine in an emergency. It cannot. Diphenhydramine (Benadryl) is an antihistamine. It blocks histamine receptors, which can reduce itching, hives, and mild swelling. It does nothing to reverse the bronchospasm that closes airways, the vasodilation that causes blood pressure to plummet, or the laryngeal edema that makes breathing impossible. Antihistamines manage discomfort. Epinephrine reverses a life-threatening cascade. The tradeoff patients weigh — often unconsciously — is between the certainty of a painful injection and the uncertainty of whether this particular reaction will become anaphylaxis.
Many people have had mild allergic reactions that resolved on their own or with an antihistamine, which trains them to believe the next one will follow the same pattern. But anaphylaxis does not follow patterns reliably. A person who had mild hives from a peanut exposure at age eight can experience full cardiovascular collapse from a similar exposure at age fifteen. Past reactions are not a reliable predictor of future severity, and experts at the ACAAI stress that epinephrine should be used at the first sign of a severe reaction, not after antihistamines have failed to work. The practical guideline most allergists now recommend is straightforward: if there is any doubt about whether a reaction is anaphylaxis, use the epinephrine. The risks of unnecessary epinephrine — elevated heart rate, jitteriness, temporary nausea — are minor and self-limiting. The risks of withholding it during true anaphylaxis are catastrophic and irreversible. When in doubt, inject.
Caregivers, Schools, and the Challenge of Delegated Emergency Response
The problem multiplies when the person experiencing anaphylaxis is a child, an elderly adult, or someone with cognitive impairment — populations where the decision to use epinephrine often falls to a caregiver, teacher, or bystander rather than the patient. For readers of this site who care for someone with dementia, the intersection of severe allergies and cognitive decline presents a particularly difficult scenario. A person with dementia may not be able to articulate what they ate, recognize that their symptoms are worsening, or locate and operate their auto-injector without help. Schools face similar challenges. Despite stock epinephrine laws in many states, administration often depends on a nurse or trained staff member being physically present.
A substitute teacher who has never seen an auto-injector, a cafeteria aide who freezes under pressure, a babysitter who doesn’t know where the device is stored — these are real-world failure points. The device is only useful if the right person knows where it is, recognizes when it’s needed, and can operate it correctly under stress. This is where training gaps become most dangerous. When studies show that more than a third of auto-injector uses involve technique errors — wrong site, insufficient force, premature removal — it’s clear that possession alone is not enough. Caregivers need hands-on practice with trainer devices, clear written anaphylaxis action plans, and the confidence to act without waiting for a doctor’s phone confirmation. Hesitation by a caregiver carries the same risk as hesitation by the patient.
Neffy — A Needle-Free Option That May Change the Equation
In August 2024, the FDA approved neffy, a 2 mg epinephrine nasal spray manufactured by ARS Pharmaceuticals, for adults and children weighing at least 30 kilograms (66 pounds). It was the first needle-free epinephrine treatment approved in over 35 years. In March 2025, the FDA expanded the approval to include a 1 mg dose for children ages four and older weighing 15 to 30 kilograms (33 to 66 pounds). Neffy directly addresses the needle-fear barrier.
A nasal spray requires no injection technique, no removal of safety caps in a specific sequence, and no sustained pressure against the thigh. Yale Medicine has noted that even untrained individuals — babysitters, teachers, restaurant staff — can effectively administer the nasal spray. For families managing food allergies, and especially for caregivers of people with dementia or other conditions that make cooperation during an injection difficult, this is a meaningful advance. The limitation worth noting is that neffy’s absorption profile differs slightly from intramuscular injection, and its long-term real-world effectiveness data is still being collected. It is not a replacement for carrying and knowing how to use a traditional auto-injector if one is available, but it lowers the barrier to action in situations where an auto-injector would otherwise go unused.
What Needs to Change — Policy, Training, and the Road Ahead
The underlying problem is not that epinephrine doesn’t work — it works extremely well when used promptly. The problem is a system-wide failure to ensure that at-risk individuals can access, carry, recognize the need for, and correctly deploy the drug in an emergency. Policy changes around cost — including insurance mandates for coverage without prior authorization and expanded access to generics — would address one of the most concrete barriers. School-based stock epinephrine programs, already showing results in states that have implemented them, need to be universal rather than optional.
Beyond policy, the cultural shift matters. Allergy organizations, emergency physicians, and allergists have spent years trying to change the default assumption from “try Benadryl first” to “use epinephrine first.” That message is getting through, but slowly. The approval of neffy and the potential for additional needle-free options in the pipeline may accelerate this shift by removing the most visceral obstacle — the fear of stabbing oneself or a child with a needle. If the barrier to use is low enough, more people will act in time. And in anaphylaxis, acting in time is the only thing that reliably separates a bad day from a funeral.
Conclusion
The gap between having an epinephrine auto-injector prescribed and actually using it in time is filled with fear, cost, confusion, poor training, and a deeply human tendency to hope that things will get better on their own. The research is consistent: delayed or absent epinephrine is the primary modifiable risk factor for death from anaphylaxis. With only 7% of adults receiving epinephrine before reaching the hospital, the current system is failing at the most basic level of emergency preparedness. For anyone managing severe allergies — or caring for someone who does, including individuals with dementia or other cognitive challenges — the action steps are specific: carry the device at all times, practice with a trainer until the steps are automatic, use epinephrine at the first sign of a severe reaction rather than reaching for an antihistamine, and call 911 immediately afterward.
Ask your allergist about neffy if needle fear has been a barrier. Replace expired devices on schedule even when the cost stings. And talk to every caregiver, teacher, and family member who might need to act on your behalf. The auto-injector only saves lives if someone is willing to use it.
Frequently Asked Questions
Can Benadryl stop anaphylaxis if I take it fast enough?
No. Antihistamines like Benadryl take 30 or more minutes to begin working and cannot reverse the airway constriction, blood pressure drop, or cardiovascular collapse that define anaphylaxis. Only epinephrine can do that. Benadryl can be given as a secondary treatment after epinephrine, but it should never be used as a substitute or first-line response.
What happens if I use my auto-injector and it turns out I didn’t actually need it?
The side effects of unnecessary epinephrine — a rapid heartbeat, shakiness, temporary anxiety, and sometimes nausea — are mild and resolve on their own. There is no serious medical downside to using it when it wasn’t strictly needed. The risk of not using it during true anaphylaxis is far greater than the risk of using it unnecessarily.
How quickly does anaphylaxis become fatal?
Fatal anaphylaxis can progress from initial symptoms to respiratory or cardiac arrest within 5 to 30 minutes, depending on the trigger and the individual. Food-triggered anaphylaxis tends to progress somewhat more slowly than drug or venom reactions, but this is not a reliable rule. Any delay in treatment increases the risk.
Is the neffy nasal spray as effective as an auto-injector?
Neffy was approved by the FDA based on clinical data showing adequate epinephrine absorption through the nasal route. Its absorption profile differs slightly from intramuscular injection, and real-world effectiveness data is still being collected. It is a genuine option for people who cannot or will not use a needle-based device, but patients should discuss the choice with their allergist.
Why is my epinephrine auto-injector so expensive?
Brand-name EpiPens cost approximately $680 to $815 for a two-pack without insurance, driven by limited market competition and the classification of auto-injectors as combination drug-device products, which face higher regulatory hurdles. Generics range from $100 to $500. Programs from manufacturers, GoodRx coupons, and state-level legislation mandating insurance coverage have helped, but cost remains a barrier for roughly one in four patients.
Should I still go to the ER after using epinephrine if I feel better?
Yes, always. Anaphylaxis can return in a biphasic reaction hours after the initial episode, even after successful epinephrine treatment. Emergency guidelines recommend at least four hours of medical observation following any anaphylactic event, regardless of how well the patient responds to the initial dose.