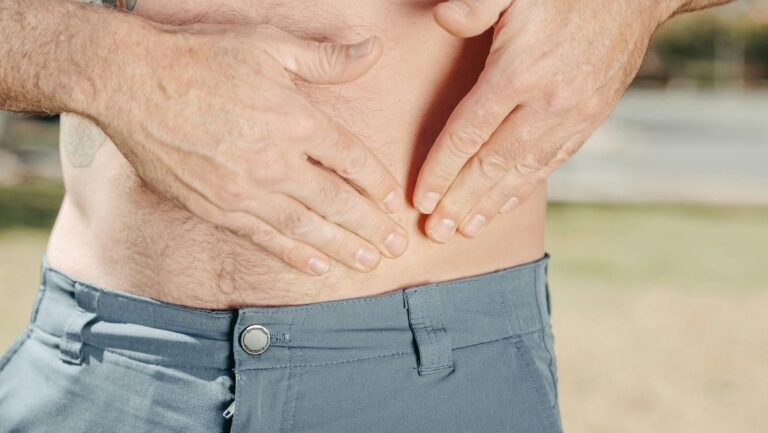
Pelvic stability exercises can meaningfully reduce fall risk, improve walking confidence, and support independence in older adults living with dementia. The seven exercises covered here — pelvic tilts, bridges, clamshells, seated marches, standing hip abductions, bird dogs, and wall sits — target the deep stabilizing muscles of the hips, lower back, and pelvic floor that tend to weaken with age and inactivity. For someone like a 78-year-old woman recovering from a hip replacement who also has mild cognitive impairment, a daily routine of gentle pelvic tilts and bridges can be the difference between needing a walker indefinitely and regaining enough stability to move around the kitchen unassisted.
These exercises matter more than most people realize for the dementia population specifically. Gait disturbances and balance problems appear early in many forms of dementia, often before a formal diagnosis. Research published in the Journal of Alzheimer’s Disease has shown that targeted lower-body strengthening can slow the rate of functional decline in people with mild to moderate cognitive impairment. This article walks through each of the seven exercises in detail, explains how to modify them for different ability levels, addresses safety concerns unique to dementia care, and covers how caregivers can provide effective cueing and support during exercise sessions.
Table of Contents
- Why Does Pelvic Stability Matter for People With Dementia?
- The Seven Exercises Explained Step by Step
- How to Modify Each Exercise for Different Ability Levels
- Building a Realistic Daily Routine Around These Exercises
- Safety Concerns and When to Stop
- The Role of Caregivers in Cueing and Motivation
- What the Research Says About Long-Term Outcomes
- Conclusion
- Frequently Asked Questions
Why Does Pelvic Stability Matter for People With Dementia?
The pelvis is the structural keystone of the body. It connects the spine to the legs and serves as the anchor point for dozens of muscles involved in standing, walking, turning, and sitting down. When the muscles surrounding the pelvis weaken — the gluteus medius, deep hip rotators, transverse abdominis, and pelvic floor — the entire chain of movement becomes less reliable. A person might start shuffling, leaning to one side, or gripping furniture to stay upright. In dementia, this physical instability compounds the cognitive challenges already affecting motor planning and spatial awareness. Falls are the leading cause of injury-related hospitalization in older adults with dementia, and pelvic instability is one of the most modifiable risk factors.
A 2021 study in the British Journal of Sports Medicine found that people with Alzheimer’s disease who participated in structured balance and strengthening programs experienced 30 percent fewer falls over a 12-month period compared to a control group. The comparison is stark: medications for fall prevention in dementia have shown far less consistent results than exercise. Unlike pharmacological interventions, pelvic stability work carries virtually no risk of adverse drug interactions or cognitive side effects. The neurological benefits deserve attention as well. Exercise that challenges balance and coordination activates brain regions involved in executive function and spatial processing — areas often affected early in dementia. This does not mean exercise reverses dementia, but it can help maintain the neural pathways that support safe movement for longer.

The Seven Exercises Explained Step by Step
The first three exercises are performed lying down, making them accessible even for people with significant balance impairment. pelvic tilts involve lying on the back with knees bent, gently pressing the lower back into the floor by engaging the abdominal muscles, holding for five seconds, and releasing. This small movement activates the transverse abdominis and teaches the brain to control the neutral pelvis position. Bridges build on the same starting position — the person presses through the heels to lift the hips off the ground, forming a straight line from shoulders to knees. This targets the gluteus maximus and hamstrings. Clamshells are performed lying on the side with knees bent at 45 degrees, opening the top knee like a hinge while keeping the feet together, which isolates the gluteus medius. The remaining four exercises involve more upright positions and greater challenge.
Seated marches — lifting one knee at a time while sitting upright in a sturdy chair — train hip flexor strength and core stability simultaneously. Standing hip abductions involve lifting one leg out to the side while holding onto a counter or chair back. Bird dogs, performed on hands and knees, require extending the opposite arm and leg, which demands significant core coordination. Wall sits, where the person leans against a wall with knees bent as if sitting in an invisible chair, build sustained endurance in the quadriceps and glutes. However, if the person has moderate to advanced dementia, bird dogs and wall sits may be too complex or physically demanding to perform safely without hands-on assistance. In that case, it is better to double the time spent on the first five exercises rather than pushing through movements that create frustration or fall risk. A physical therapist can assess which exercises are appropriate for each individual’s cognitive and physical stage.
How to Modify Each Exercise for Different Ability Levels
Modification is not about making exercises easier in a way that removes the benefit — it is about matching the challenge to the person’s current ability so the muscles actually get worked. For bridges, a person who cannot lift the hips fully off the ground can start by simply pressing the hips upward an inch or two. That partial movement still activates the glutes. Over weeks, the range of motion often improves. Adding a small pillow or ball between the knees during bridges also recruits the inner thigh muscles and gives the person a tactile cue to squeeze against, which can be helpful when verbal instructions are hard to follow. For standing exercises, the width and stability of the support surface matter enormously.
A kitchen counter is generally safer than a single chair because it provides a longer surface to grip if the person sways. One occupational therapist described working with a client who had vascular dementia and kept forgetting to hold on during standing hip abductions. The solution was placing a bright piece of tape on the counter as a visual anchor — the client’s attention was drawn to the tape, and the hand followed. Small environmental cues like this often work better than repeated verbal reminders in dementia care. Seated marches can be progressed by adding a light ankle weight — even one pound makes a noticeable difference — or by slowing the movement down so each lift takes three full seconds. Slower repetitions increase the time the muscles spend under tension, which builds strength more effectively than fast, momentum-driven movements.

Building a Realistic Daily Routine Around These Exercises
The biggest mistake caregivers make with exercise programs is treating them like a formal gym session. For someone with dementia, a 30-minute structured workout is often overwhelming. A more effective approach is embedding two or three exercises into existing daily routines. Pelvic tilts and bridges can happen in bed before getting up in the morning — three sets of eight repetitions takes about four minutes. Seated marches fit naturally into the period after breakfast while the person is still at the table. Standing hip abductions can be paired with time at the kitchen counter, such as while waiting for tea to brew.
This distributed approach has a practical tradeoff: it requires the caregiver to remember multiple cue points throughout the day rather than blocking off one chunk of time. Some families find that a simple checklist on the refrigerator helps — not for the person with dementia, but for whoever is providing care that day. The alternative, a single dedicated exercise session, works better when a professional is leading it, such as during a home health visit or adult day program. Neither approach is inherently superior, but the distributed model tends to produce better long-term adherence in home settings because it does not depend on the person’s willingness to start a formal activity. Consistency matters more than volume. Three exercises done every day for six months will produce more functional improvement than all seven exercises done sporadically for the same period. Start with the two or three exercises the person tolerates best and build from there.
Safety Concerns and When to Stop
The most important safety rule is simple: if an exercise causes sharp pain, stop immediately. Muscle soreness the following day is normal and expected when starting a new routine, but pain during the movement itself — particularly in the lower back, hip joint, or knees — signals that something is wrong. This could mean the form is incorrect, the exercise is too advanced, or there is an underlying orthopedic issue that needs medical evaluation. For people with dementia, there is an additional safety layer that is easy to overlook: the person may not reliably report pain. Facial grimacing, guarding a body part, sudden resistance to an exercise they previously tolerated, or increased agitation during or after exercise can all indicate discomfort.
Caregivers need to watch for these nonverbal signals closely, especially as dementia progresses and verbal communication becomes less reliable. Certain medical conditions require exercise modification or medical clearance before starting. Osteoporosis increases the risk of fracture during loaded exercises like wall sits. Severe spinal stenosis can make extension-based movements like bird dogs painful. Uncontrolled blood pressure may warrant avoiding positions where the head drops below the heart. A conversation with the person’s physician or a physical therapist is not optional — it is a necessary first step, particularly for anyone who has not been physically active recently.
The Role of Caregivers in Cueing and Motivation
Verbal cueing for exercise looks different in dementia care than in a typical physical therapy session. Long, multi-step instructions overwhelm working memory. Instead of saying “Lie on your back, bend your knees, put your feet flat on the floor, and press your lower back down,” break it into single actions with pauses between each one. “Lie on your back.” Wait.
“Bend your knees.” Wait. “Now press your back down into the bed.” Demonstration is even more effective — mirror neurons respond to seeing a movement performed, and many people with dementia can imitate a movement they cannot follow verbally. One adult daughter caring for her father with Lewy body dementia described how she started doing the exercises alongside him each morning. He could not remember the routine on his own, but when she began her bridges next to him in bed, he would join in without being asked. The social component turned exercise from a task imposed on him into a shared activity, which reduced his resistance considerably.
What the Research Says About Long-Term Outcomes
The evidence base for exercise in dementia care has grown substantially over the past decade. A 2023 Cochrane review concluded that multicomponent exercise programs — those combining strength, balance, and flexibility work — can maintain physical function and reduce fall rates in people with mild to moderate dementia. Pelvic stability exercises hit all three components when programmed thoughtfully. The review also noted that benefits diminish within weeks of stopping exercise, which reinforces the need for sustainable, ongoing routines rather than short-term programs.
Looking ahead, there is growing interest in combining physical exercise with cognitive tasks — known as dual-task training — to amplify the benefits of both. Counting repetitions aloud, naming objects in the room during seated marches, or following rhythm-based movement cues are all ways to layer cognitive engagement onto pelvic stability work. Early studies suggest this combined approach may slow functional decline more than exercise alone, though the research is still emerging. What is already clear is that doing nothing carries the highest cost. Every week of inactivity accelerates the cycle of weakness, falls, hospitalization, and further cognitive decline.
Conclusion
Pelvic stability is not a luxury goal for people living with dementia — it is foundational to maintaining the ability to stand, walk, and use the bathroom independently. The seven exercises described here require no equipment, can be scaled to nearly any ability level, and address the specific muscle groups most responsible for balance and gait. The key principles are consistency over intensity, environmental and verbal cueing tailored to the person’s cognitive level, and ongoing attention to safety signals that the person may not be able to articulate.
Starting is the most important step, and starting small is perfectly fine. Two exercises done reliably each morning will build a foundation that additional exercises can be added to over time. Involve the person’s healthcare team in selecting the right starting point, and revisit the program as abilities change. Pelvic stability work is one of the few interventions in dementia care that is low-cost, low-risk, and supported by strong evidence — and it is available to nearly everyone willing to commit a few minutes a day.
Frequently Asked Questions
Can someone with advanced dementia still do pelvic stability exercises?
Yes, though the exercises will need significant modification. Pelvic tilts and bridges in bed, with hands-on guidance from a caregiver, can still activate the target muscles even when the person cannot follow verbal instructions. A physical therapist experienced in dementia care can design an appropriate program.
How quickly will these exercises reduce fall risk?
Most studies show measurable improvements in balance and lower-body strength within six to eight weeks of consistent practice, with three to five sessions per week. Fall reduction takes longer to demonstrate statistically, typically three to six months, because falls are relatively infrequent events that require longer observation periods.
Should these exercises replace walking as a form of physical activity?
No. Walking and pelvic stability exercises serve different but complementary purposes. Walking is a cardiovascular and functional activity, while pelvic exercises target specific stabilizing muscles that walking alone does not adequately strengthen. The best outcomes come from combining both.
What if the person refuses to exercise?
Resistance to exercise is common in dementia and does not always mean the person dislikes the activity. It may reflect confusion about what is being asked, pain, fatigue, or mood. Try different times of day, use demonstration rather than instruction, or embed movements into activities the person already enjoys. If resistance is persistent, a brief break of several days followed by a different approach often helps more than pushing through.
Is it safe to do these exercises without a physical therapist present?
The lying-down and seated exercises — pelvic tilts, bridges, clamshells, and seated marches — are generally safe for most people to do at home with caregiver supervision. Standing exercises and bird dogs carry more fall risk and ideally should be taught by a physical therapist first before being continued independently.