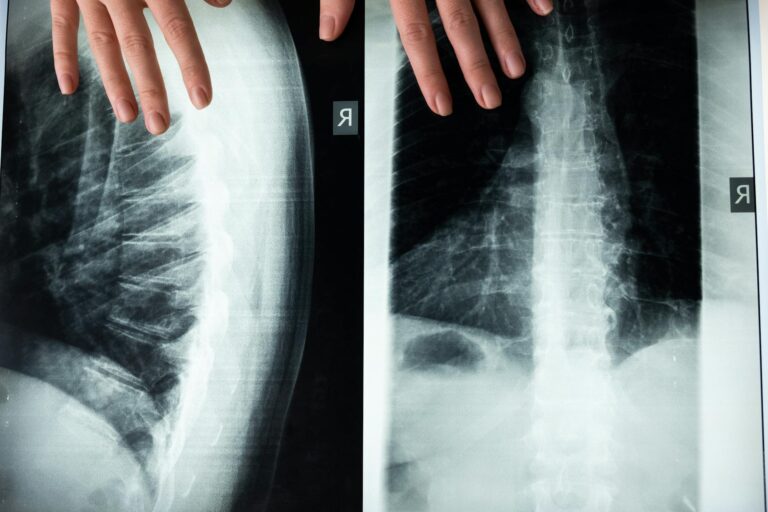
Lumbar spine injuries frequently develop so gradually that people fail to notice them until movement becomes painful or limited. The earliest warning signs—a subtle stiffness in the morning, a slight numbness in the groin or foot, a feeling that your flexibility isn’t quite what it used to be—are easily mistaken for the normal aging process. By the time symptoms become obvious enough to seek treatment, the underlying injury has often progressed significantly.
Understanding these ten gradual-onset symptoms matters especially for older adults and caregivers, because early recognition can prevent the cascade of mobility loss that leads to falls, dependence, and complications. This article walks through the symptoms that develop insidiously in lumbar spine injuries, why they’re so easy to overlook, and what distinguishes them from normal aging. With 619 million people globally experiencing low back pain and low back pain being the leading cause of disability worldwide since 1990, recognizing these gradual warning signs can be the difference between early intervention and chronic disability.
Table of Contents
- What Are the Gradually Worsening Symptoms of Lumbar Spine Injuries?
- How Gradual Symptoms Get Mistaken for Normal Aging
- Specific Symptom #1-3: Back and Lower Extremity Stiffness
- Symptoms #4-6: Weakness, Numbness, and Sensory Changes
- Symptoms #7-9: Radicular Pain and Sciatica
- Symptom #10: Progressive Loss of Function and Mobility
- Age-Related Differences and Future Risk Projections
- Conclusion
What Are the Gradually Worsening Symptoms of Lumbar Spine Injuries?
lumbar spine injuries rarely announce themselves with sudden, dramatic pain. Instead, they evolve through a pattern of creeping symptoms that get slowly worse over weeks or months. A person might notice their back feels “off” one morning, then attribute the stiffness to sleeping wrong. By the next month, that stiffness has become a chronic ache. By month three, they realize they can’t bend forward as far as they used to.
This gradual progression is partly why 90% of back pain cases—which involve spine, muscle, and joint dysfunction—go unaddressed until significant damage has accumulated. The verified symptoms that develop gradually include subtle motor impairment (progressive weakness in the legs and feet), sensory disturbances (numbness or tingling), and flexibility loss in the hips, groin, and legs. These can extend into sciatica, where pain radiates down the back of the leg or into the foot. Radicular pain—nerve pain that follows a specific path down the spine—is another hallmark of gradual lumbar injury. None of these typically appears overnight; they build over time in ways that feel like aging rather than injury.

How Gradual Symptoms Get Mistaken for Normal Aging
One of the biggest obstacles to early diagnosis is that gradual lumbar spine symptoms genuinely mimic the aging process. A 65-year-old who gradually loses hip flexibility might assume it’s just what happens after 65. Someone who notices slight numbness in their foot might chalk it up to circulation changes.
This is partly why older adults have a dramatically higher prevalence of degenerative disc disease, facet arthropathy, osteoporotic compression fractures, and spinal stenosis—these conditions accumulate slowly and silently. However, there’s a critical difference: true age-related changes develop uniformly across the body, while nerve-related symptoms from spine injuries follow specific patterns and typically affect one side more than the other. If you feel numbness only in your right foot, or weakness only down your left leg, that pattern points to a spine issue, not simple aging. In adults ages 60-69, the incidence of lumbar fractures increased 3.24-fold between 2003 and 2022, and falls account for 76.6% of these injuries in older populations—yet many of these injuries go unrecognized until they become severe.
Specific Symptom #1-3: Back and Lower Extremity Stiffness
The most common entry point into gradual lumbar spine injury is stiffness. You might wake up stiff—which happens to everyone sometimes—but then realize you’re still stiff after coffee, after a shower, after walking around. Over weeks, this stiffness becomes your new baseline. You find yourself moving more carefully, taking stairs differently, or avoiding activities that used to feel natural. This stiffness often worsens with certain positions (like sitting hunched at a desk) and improves with gentle movement or walking.
Following closely are subtle pain and loss of flexibility. The pain often feels like a deep ache rather than sharp discomfort, and people commonly describe it as a “nagging” sensation. It may be localized to the lower back, or it may be felt across the entire lower spine region. Loss of flexibility—the inability to bend forward, twist, or extend backward as far as you once could—compounds the stiffness. A person might notice they can’t tie their shoes as easily, or that touching their toes has become impossible, changes that develop so gradually they don’t mark the date when it started.

Symptoms #4-6: Weakness, Numbness, and Sensory Changes
As lumbar nerve roots become compressed or irritated, weakness in the legs develops insidiously. You might notice you’re not taking stairs as quickly, or that a walk that used to feel easy now leaves your legs feeling fatigued sooner. This isn’t the obvious muscle weakness of a stroke; it’s a subtle, progressive loss of power. Some people describe it as “my legs don’t respond like they used to” or “I feel less stable on my feet.” Numbness and tingling typically start in unexpected places: the outer thigh, the groin, the foot, or around the buttock.
These sensory disturbances often come and go initially—present on some days and absent on others—which makes them easy to dismiss. Over time they become constant. The pattern matters: if numbness appears only on the right side of your body or affects only specific dermatomes (the areas of skin supplied by a single nerve root), that pattern indicates a specific spine problem. Contrast this with age-related circulation changes, which would affect both legs equally and wouldn’t follow nerve pathways.
Symptoms #7-9: Radicular Pain and Sciatica
Radicular pain is pain caused by nerve compression or irritation at the spine, and it follows the exact path that the affected nerve travels to the rest of the body. When the lumbar spine irritates the sciatic nerve—which is enormous and travels from the lower spine all the way down the back of the leg and into the foot—you get sciatica. This pain might start as a subtle ache in the buttock and gradually progress down the back of the thigh, eventually reaching the foot. It’s typically felt on one side only (unilateral), which is a key distinguishing feature.
However, if sciatica pain is constant and severe from day one, that’s typically an acute injury, not a gradual lumbar problem. The gradual presentation involves mild symptoms that slowly worsen—a tingling sensation that becomes throbbing, an ache that becomes sharp. Some people report that certain movements make it worse: sitting for long periods, bending, twisting, or walking in a particular pattern. Over weeks and months, this progressive pain can significantly limit activity and lead to secondary problems like muscle atrophy from avoiding movement.

Symptom #10: Progressive Loss of Function and Mobility
The tenth and often most consequential symptom is the gradual loss of functional ability. This might manifest as an inability to perform previously routine activities: difficulty getting out of a chair without using your hands, trouble lifting things, changes in gait, or an increasing reliance on railings and supports. This functional decline is insidious because it compounds over time. A person reduces activity to avoid pain, which leads to deconditioning, which makes activity even harder, which leads to further reduction.
For older adults and those with cognitive concerns, this functional decline deserves special attention. Falls account for 76.6% of lumbar spine injuries in older populations, yet the reverse is also true: lumbar spine injuries that affect mobility increase fall risk significantly. Someone with a gradual lumbar injury may not consciously notice their balance is worse, but their nervous system knows their spine is compromised, and compensation patterns develop that subtly increase fall risk. This creates a dangerous feedback loop that can lead to serious injury.
Age-Related Differences and Future Risk Projections
The way lumbar spine injuries develop and present changes dramatically with age. Younger individuals tend to suffer acute muscular strain, ligamentous injury, or disc herniation—injuries that often announce themselves loudly. Older adults, by contrast, more commonly experience degenerative changes that accumulate silently: the discs dry out and crack, the facet joints develop arthritis, the spinal canal narrows.
These conditions are often present for years before causing noticeable symptoms, and when symptoms do appear, they’re easily attributed to aging. The statistics paint a sobering picture: with 36.4% increase in low back pain cases projected by 2050 compared to 2020, and over 800 million people expected to have low back pain globally by 2050, gradual lumbar spine injuries will become even more common. This means the window for early intervention—catching these gradually developing symptoms before they cause severe disability—becomes increasingly important for maintaining independence and quality of life in older age.
Conclusion
The ten symptoms of gradually developing lumbar spine injuries—from subtle morning stiffness and sensory disturbances to progressive weakness, radicular pain, and functional decline—are almost universally mistaken for normal aging. Because these symptoms develop so slowly and pattern-match to aging so closely, many people lose years of mobility and function before seeking help. The key to early intervention is recognizing these specific patterns: stiffness and pain that progressively worsen, weakness and numbness that follow nerve pathways rather than diffusing across the body, and functional decline that accumulates over months rather than occurring suddenly.
If you notice any combination of these gradual symptoms—especially those that follow a one-sided pattern or that noticeably limit activities you once performed easily—discuss them with a healthcare provider. Early evaluation can determine whether you’re experiencing normal aging or a lumbar spine injury that benefits from intervention. With 90% of back pain cases involving mechanical dysfunction of the spine and muscles, conservative treatment often succeeds when applied early, making prompt recognition of these gradual symptoms valuable for preserving mobility and independence.